Principles & Goals - Golden Years Gains
- Primary Goal: Maximize functional independence & enhance Quality of Life (QoL).
- Core Aim: Not just ↑ lifespan, but ↑ healthspan - active, engaged years.
- Key Principles:
- Patient-centered: Tailored goals, respecting autonomy.
- Multidisciplinary Team (MDT): Physio, OT, speech, social work, physician.
- Address physiological aging: Sarcopenia, osteopenia, sensory decline, cognitive changes.
- Prevent iatrogenesis (harm from medical intervention) & deconditioning.
- Promote activity, nutrition, social engagement.
- Early mobilization & intervention.
- Assessment Cornerstone:
⭐ Comprehensive Geriatric Assessment (CGA) is the cornerstone of effective geriatric care, improving outcomes and quality of life.
- Includes functional status (ADLs, IADLs), mobility, cognition, mood, nutrition.

Conditions & Assessment - Elderly Hurdles & Measures
- Common Conditions:
- Orthopaedic: Osteoarthritis (OA), Osteoporosis (OP; DEXA T-score ≤ -2.5), Fractures (hip, vertebral).
- Systemic: Sarcopenia (↓muscle mass & strength), Frailty, Falls, Polypharmacy (≥5 drugs), Malnutrition.
- 📌 Geriatric Giants (4 Is): Immobility, Instability, Incontinence, Impaired Intellect/Memory.
- Key Assessments & Thresholds:
- Mobility:
- Timed Up and Go (TUG): >12s indicates ↑fall risk.
- Gait Speed: <0.8 m/s predicts ↑adverse outcomes.
- Balance: Berg Balance Scale (BBS): <45/56 indicates ↑fall risk.
- Frailty: Clinical Frailty Scale (CFS), Fried Frailty Phenotype.
- Nutrition: Mini Nutritional Assessment (MNA).
- Cognition: Mini-Mental State Examination (MMSE), Montreal Cognitive Assessment (MoCA).
- Mobility:
- Hurdles: ↓Physiological reserve, multiple comorbidities, psychosocial factors.
- Measures: Comprehensive Geriatric Assessment (CGA), multidisciplinary team approach.
⭐ Sarcopenia, the age-related loss of muscle mass and function, is a major contributor to frailty and disability in older adults.
Interventions & Strategies - Moves, Aids & Safety
- Therapeutic Exercise (Tailored & Progressive):
- Strength: Resistance training (e.g., weights, bands); builds muscle, bone density.
- Balance: Tai Chi, Otago exercises; reduces fall risk.
- Endurance: Walking, swimming; improves cardiovascular fitness.
- Flexibility: Stretching; maintains range of motion (ROM).
- Assistive Devices (Proper Fit & Training Crucial):
- Mobility: Canes, walkers, wheelchairs for stability & ambulation.
- ADL Aids: Grab bars, raised toilet seats, reachers to promote independence.
- Fall Prevention Strategies:
- Comprehensive fall risk assessment (e.g., Morse Fall Scale).
- Home environment modification (lighting, remove hazards).
- Medication review (esp. psychotropics, polypharmacy).
- Vitamin D supplementation if deficient.

⭐ The Otago Exercise Programme, an individually prescribed home-based program of muscle-strengthening and balance-retraining exercises, reduces falls by 30-40% in at-risk older adults.
Special Aspects & Teamwork - Holistic Geriatric Care
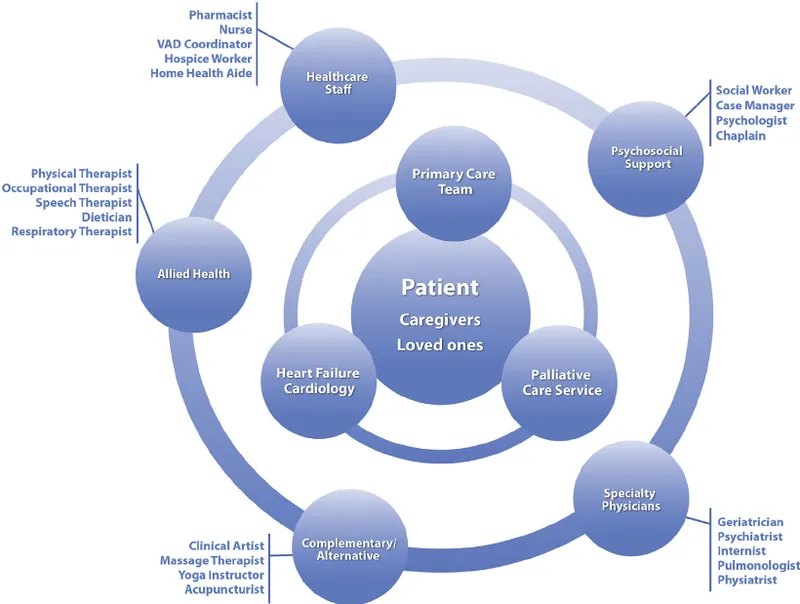
- Multidisciplinary Team (MDT): Essential for holistic care.
- Core: Geriatrician, Ortho Surgeon, PT, OT, Nurse, Social Worker.
- Special Geriatric Considerations:
- Polypharmacy: Systematic review, de-prescribing to ↓ADEs.
- Cognitive Impairment: Assess for dementia, delirium; manage.
- Psychosocial Support: Address mood, isolation, family involvement.
- Nutritional Optimization: Crucial for recovery.
- Falls Prevention: Multifactorial assessment & interventions.
⭐ Addressing polypharmacy through systematic review and de-prescribing is crucial to minimize adverse drug events and improve functional outcomes in geriatric patients.
High‑Yield Points - ⚡ Biggest Takeaways
- Geriatric rehabilitation aims for maximal functional independence and enhanced quality of life in elderly patients.
- A multidisciplinary team (MDT) is vital for comprehensive assessment, planning, and management.
- Key priorities: fall prevention strategies, sarcopenia management, and effective pain control.
- Addresses common issues: osteoporosis-related fractures, post-stroke sequelae, and arthritic limitations.
- Cognitive status (e.g., dementia) significantly impacts rehabilitation; requires adapted strategies.
- Patient-centered goals, family involvement, and polypharmacy review are critical.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

