DDH Fundamentals - Hip Hitch 101
- Definition: DDH is a spectrum of developmental abnormalities affecting the immature hip joint, ranging from subtle acetabular dysplasia to frank dislocation of the femoral head.
- Incidence: 1-3 cases per 1000 live births.
- Key Risk Factors:
- 📌 Female sex (4-6x higher risk)
- 📌 Firstborn child
- 📌 Family history of DDH
- 📌 Frank breech presentation
- 📌 Fluid (Oligohydramnios)
- Left hip predominance
- Improper swaddling (legs extended, adducted)
⭐ Breech presentation is a highly significant risk factor for DDH.
Pathoanatomy & Diagnosis - Spotting Wobbly Joints
Pathoanatomy:
- Acetabular Dysplasia: Shallow, oblique socket (↑ Acetabular Index).
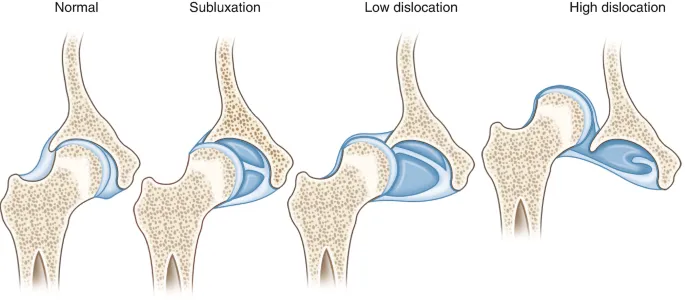
- Femoral Head: Subluxated/dislocated, often superolateral.
- Capsule & Ligaments: Stretched, lax; ligamentum teres hypertrophy.
- Soft Tissue Obstacles: Inverted limbus, pulvinar, tight adductors/iliopsoas.
Clinical Diagnosis:
- Neonates/Infants (<3 months):
- Barlow Maneuver: Dislocates (Adduct + Posterior pressure). 📌 "Barlow = Bad / Back"
- Ortolani Maneuver: Reduces (Abduct + Anterior pressure). 📌 "Ortolani = Out / Open"
- Infants (3-12 months):
- Limited hip abduction (< 60°).
- Galeazzi Sign: Unequal knee heights (femoral shortening).
- Asymmetric thigh/gluteal skin folds.
- Walking Child (>12 months):
- Painless limp / Trendelenburg gait.
- Waddling gait (if bilateral DDH).
⭐ Ortolani and Barlow tests are most reliable in the first 2-3 months; sensitivity decreases later due to soft tissue contractures.
Imaging:


Management Strategy - Align & Conquer
Goal: Achieve stable, concentric hip reduction. Treatment guided by age at diagnosis.
- Key Principles:
- Early intervention yields best outcomes.
- Avoid forceful abduction (↑ AVN risk).
- Regular follow-up for growth & AVN monitoring.
- Pavlik Harness (0-6 months):
- Dynamic flexion (100-110°) & abduction (30-50°) orthosis.
- Worn 23 hrs/day. Wean after USG normalisation.
- Monitor weekly initially.
- ⚠️ Complications: Femoral nerve palsy, AVN, skin issues.
⭐ Pavlik harness "safe zone" (Ramsey): Hip flexion 90-110°, abduction 30-60°. Crucial to prevent AVN & ensure reduction.
-
Closed Reduction (CR) + Spica Cast (6-18 months):
- Under GA; adductor tenotomy common.
- Confirm reduction: arthrogram, CT ("CT stabogram").
- Cast duration: ~3 months.
-
Open Reduction (OR):
- If CR fails or older children (>18 months).
- Often requires femoral and/or pelvic osteotomies for stability.
- Pelvic: Salter, Dega, Pemberton.
- Femoral: Shortening, Varus Derotation Osteotomy (VDRO).

Complications & Long-Term - Pitfalls & Prognosis
- Avascular Necrosis (AVN): Most serious. Risk: forceful reduction, extreme abduction.
- Residual Dysplasia: Leads to early Osteoarthritis (OA), chronic pain.
- Redislocation/Subluxation
- Joint Stiffness: Especially limited abduction.
- Gait Abnormalities: Persistent limp, waddling.
- Leg Length Discrepancy
- Premature Physeal Arrest
- Prognosis: Good if treated <6 months. Delayed diagnosis ↑ long-term OA risk.
⭐ Avascular necrosis (AVN) of the femoral head is the most common serious complication following reduction maneuvers for DDH.
oka
High‑Yield Points - ⚡ Biggest Takeaways
- Neonatal screening: Barlow (dislocates), Ortolani (relocates); Galeazzi sign in older infants.
- Risk factors: Female, Firstborn, Family Hx, Frank breech (4Fs).
- Diagnosis: Ultrasound < 6 months; X-ray > 6 months (Shenton's line, ↑ Acetabular Index).
- Treatment < 6 months: Pavlik harness (flexion, abduction).
- Treatment 6-18 months: Closed reduction & spica cast; Open reduction if older/failed.
- Complication: Avascular necrosis (AVN) of femoral head.
- Untreated: Leads to limp, pain, early osteoarthritis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

