Biopsy Basics - The First Cut
- Purpose: Diagnose (benign/malignant), grade, stage; guide treatment. Crucial before definitive surgery.
- Indications: Suspicious lesion on imaging (X-ray, MRI).
- Core Principles:
- Longitudinal incision, planned for future resection.
- Prevent tumor seeding; meticulous hemostasis.
- Biopsy tract must be resectable with specimen.
- Adequate, representative tissue.
- Avoid neurovascular structures, joint spaces.
- Pathologist coordination: fresh tissue (special studies), formalin (routine).
- ⚠️ Poor technique compromises limb salvage.
⭐ Biopsy tract is considered contaminated; must be excised en bloc with the tumor during definitive surgery.
Needle vs. Knife - The Great Debate
-
Needle Biopsy (Percutaneous):
- Core Needle Biopsy (CNB) preferred over FNAC for sarcomas (provides architecture).
- Pros: Minimally invasive, local anesthesia, ↓cost, ↓morbidity, outpatient. Often image-guided (USG/CT).
- Cons: ↑Sampling error risk (heterogeneous tumors). Coaxial technique ↓seeding.
- Accuracy: CNB ~90-95% with experience.
-
Open Biopsy (Surgical):
- Incisional (representative sample) vs. Excisional (entire lesion - rare for primary bone malignancy).
- Pros: Gold standard. Ample tissue for definitive diagnosis, grading, molecular studies.
- Cons: Invasive, general/regional anesthesia, ↑cost, ↑hospital stay, ↑complications (infection, hematoma, pathological fracture).
- Crucial: Longitudinal incision, planned for en bloc resection with tumor.
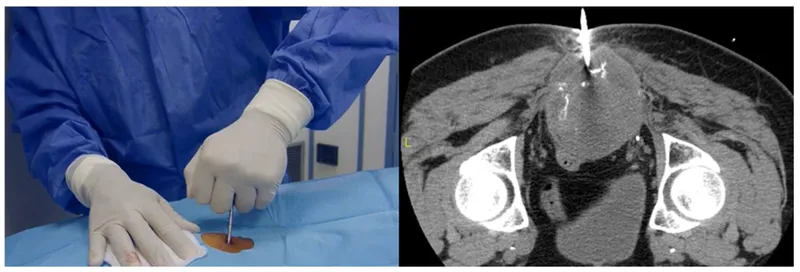
⭐ Biopsy tract MUST be resectable en bloc with tumor at definitive surgery to prevent recurrence.
The Perfect Path - Biopsy Blueprint
- Pre-Biopsy Protocol: Foundation for Success
- MDT consensus; review all imaging (X-ray, MRI ± CT).
- Biopsy after full staging investigations.
- Definitive surgeon plans/performs biopsy.
- Longitudinal incision: tract designed for en-bloc excision.
- Avoid: Neurovascular bundles, joint spaces, reactive zones.
- Technique & Specimen Logistics:
- Obtain adequate, representative tissue (avoid necrosis).
- Meticulous hemostasis to prevent hematoma.
- Gentle handling; label specimen accurately.
- Samples: Histopathology (formalin), Microbiology (saline), Cytogenetics (RPMI/saline), Fresh for research.
- Frozen section: confirms diagnostic yield.
- Closure & Considerations:
- Secure hemostasis.
- Layered closure; drain (if used) exits in line with incision.
> ⭐ A poorly planned biopsy can compromise limb salvage options or even curative intent.
Oops & Uh-Ohs - Complication Control
- Hemorrhage/Hematoma:
- Prevention: Avoid large vessels, careful technique, pressure.
- Management: Pressure; rarely embolization.
- Infection:
- Prevention: Strict asepsis; prophylactic antibiotics (deep biopsies).
- Management: Antibiotics, debridement.
- Tumor Seeding/Contamination: ⚠️
- Prevention: Longitudinal incision, tract excision with surgery, avoid new compartments.
⭐ Biopsy tract: orient longitudinally, plan for en-bloc resection with tumor during definitive surgery to prevent local recurrence.
- Pathological Fracture:
- Prevention: Gentle handling (lytic lesions); core needle for weak bone.
- Management: Stabilization.
- Neurovascular Injury:
- Prevention: Image guidance, anatomy knowledge.
- Management: Repair if needed.
- Non-Diagnostic Sample:
- Prevention: Multiple cores, viable tissue, intra-op check.
- Management: Repeat biopsy_
High‑Yield Points - ⚡ Biggest Takeaways
- Biopsy tract must be planned for en-bloc excision with definitive surgery.
- Core needle (Tru-Cut) biopsy is standard initial diagnosis for most suspected sarcomas.
- Open biopsy offers most tissue but ↑ risk of contamination and hematoma.
- FNAC is limited for sarcoma diagnosis; better for metastatic carcinoma or lymphoma.
- Longitudinal incisions are preferred; transverse incisions compromise limb salvage.
- Frozen section during open biopsy confirms diagnostic tissue, not definitive diagnosis.
- Biopsy after complete imaging (X-ray, MRI) to avoid altering findings.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

