Tendon Anatomy & Healing - Cable Care 101
- Anatomy:
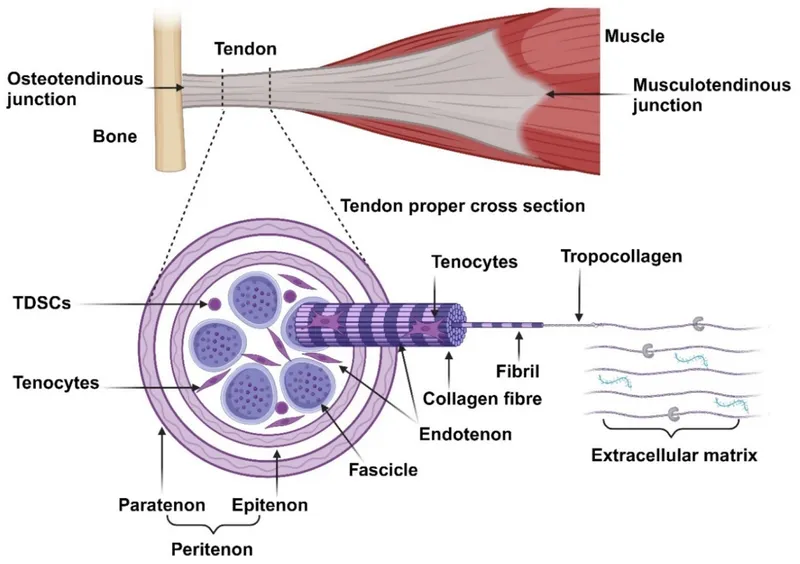
- Composition: Primarily Type I collagen (~95%), tenocytes (specialized fibroblasts), elastin, proteoglycans.
- Structure: Fibrils → Fibers → Fascicles → Tendon. Covered by Epitenon (outer, vascular layer) & Endotenon (inner, surrounds fascicles).
- Blood Supply:
- Intrinsic: Myotendinous & osteotendinous junctions.
- Extrinsic: Vincula (long & short for flexors), paratenon/mesotenon (for extensors).
- Healing Phases (Approximate):
-
- Inflammatory (0-5 days): Hematoma formation, migration of inflammatory cells (neutrophils, macrophages). Weakest phase; defect filled by clot.
-
- Proliferative/Reparative (5 days - 3 weeks): Fibroblasts proliferate, synthesize Type III collagen. ↑ vascularity & cellularity.
-
- Remodeling/Maturation (3 weeks - 1 year+): Type III collagen gradually converts to Type I. ↑ tensile strength, collagen cross-linking & reorientation along stress lines.
-
- Key Factors Influencing Healing: Age, smoking, diabetes, nutrition, vascularity, type of injury, gap size, infection, controlled early mobilization (crucial!).
⭐ Sutured tendons typically regain ~50-60% of their original strength by 6 weeks; achieving near-normal strength can take up to 1 year or more, and it may never reach 100% pre-injury levels.
Flexor Tendon Injuries - Flexor Fails & Fixes
- Anatomy & Function:
- FDS (Flexor Digitorum Superficialis): Flexes PIP joint.
- FDP (Flexor Digitorum Profundus): Flexes DIP joint.
- Vincula: Segmental blood supply to tendons.
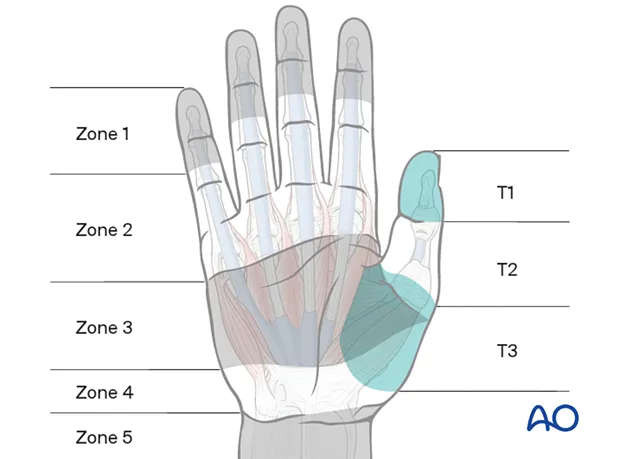
- Verdan's Zones: Critical for management & prognosis.
- Zone I: FDP only (distal to FDS insertion). Common:
Extensor Tendon Injuries - Extensor Wrecks & Repairs
- Extensor tendons: flatter, less robust than flexors; lie superficially, prone to injury. Less retraction due to juncturae tendinum. Poorer blood supply.
- Repair often challenging due to thinness and risk of adhesions. Early motion protocols crucial.
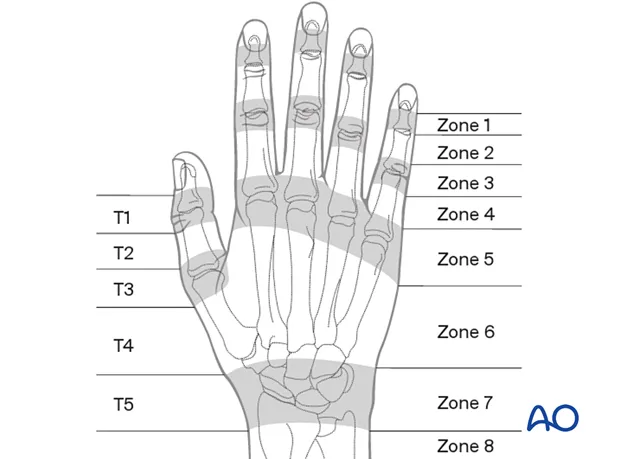
- Common Injuries & Deformities:
- Mallet Finger (Zone I/II): Injury to terminal extensor tendon insertion on distal phalanx.
- Cause: Forced flexion of extended DIP.
- Presentation: DIP joint rests in flexion (~45°); inability to actively extend DIP.
- Treatment: Uninterrupted splinting of DIP in full extension for 6-8 weeks. Surgical pinning if large fracture fragment or subluxation.
- Boutonniere Deformity (Zone III/IV): Injury to central slip insertion on middle phalanx.
- Pathophysiology: Central slip disruption → lateral bands displace volarly → PIP flexion & DIP hyperextension.
- Treatment: PIP joint splinted in full extension for 4-6 weeks, allowing DIP motion.
- Mallet Finger (Zone I/II): Injury to terminal extensor tendon insertion on distal phalanx.
⭐ Elson's test is used to diagnose a central slip rupture (potential Boutonniere): PIP flexed to 90° over edge of table, patient attempts to extend middle phalanx. Weakness/absence of extension with fixed DIP indicates rupture.
High‑Yield Points - ⚡ Biggest Takeaways
- Zone II flexor injuries ("No Man's Land") have poorest prognosis due to adhesion risk.
- Mallet finger: Terminal extensor tendon disruption (Zone I), causing DIP droop.
- Boutonnière deformity: Central slip injury (Zone III), causing PIP flexion, DIP hyperextension.
- Jersey finger: FDP avulsion (Zone I flexor), often ring finger, unable to flex DIP.
- Early active motion is key post-flexor repair to prevent adhesions.
- Primary repair is ideal for acute tendon injuries.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

