Anatomy & Basics - Bones & Bands Bonanza
- Bones: Tibia (medial malleolus, posterior malleolus), Fibula (lateral malleolus), Talus.
- Malleoli: Medial (tibia), Lateral (fibula), Posterior (tibia).
- Syndesmosis (Distal Tibiofibular):
- Anterior Inferior Tibiofibular Ligament (AITFL)
- Posterior Inferior Tibiofibular Ligament (PITFL)
- Interosseous Ligament (IOL)
- Transverse Ligament
- Major Ligaments:
- Medial: Deltoid complex (superficial & deep)
- Lateral: Anterior Talofibular (ATFL), Calcaneofibular (CFL), Posterior Talofibular (PTFL).

⭐ The posterior malleolus is an extension of the posterior tibial plafond and its fracture often indicates significant injury and potential instability requiring fixation if >25% of articular surface or >2 mm displacement is involved.
📌 Mnemonic (Lateral Ligaments): Always Take Five Lads; Can Feel Love; Please Take Five Lasses (ATFL, CFL, PTFL from anterior to posterior).
Classification Systems - Cracking the Codes
Predict stability & guide treatment:
-
Lauge-Hansen Classification: Mechanism-based. 📌 SAD, SER, PAB, PER.
Type Fibula Fracture Medial Injury Other Key Injuries SAD Transverse, below syndesmosis Vertical Med. Mall. SER Spiral, at syndesmosis Med. Mall. / Deltoid Post. Mall. # / PITFL tear PAB Trans/Obl, above syndesmosis Med. Mall. / Deltoid Syndesmotic injury PER High Spiral, above syndesmosis Med. Mall. / Deltoid Ant/Post Syndesmotic, Interosseous memb. -
Danis-Weber Classification: Fibular # level to syndesmosis.
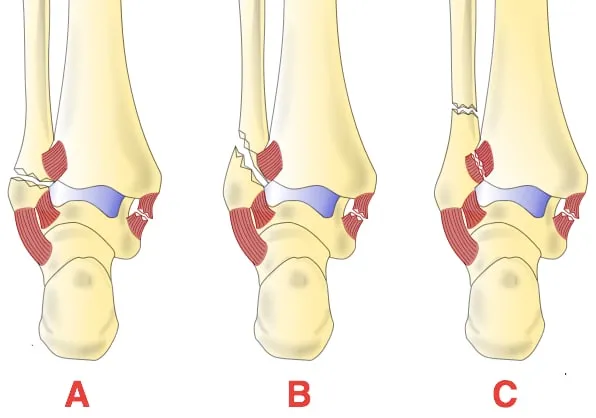
- Type A: Fibula # below syndesmosis. Intact. Stable.
- Type B: Fibula # at syndesmosis. Injury variable.
- Type C: Fibula # above syndesmosis. Disrupted. Unstable.
⭐ Weber C fractures, with fibular fracture proximal to the syndesmosis, are considered unstable and often require syndesmotic screw fixation.
Clinical Features & Diagnosis - Spotting the Snaps
- Presentation: Acute pain, swelling, deformity, ecchymosis, can't bear weight.
- Examination: Palpate: tenderness, crepitus. Stability: Squeeze, external rotation, Cotton tests.
- 📌 Ottawa Ankle Rules: Guides X-ray. Malleolar/midfoot pain + bone tenderness (post. malleoli, navicular, 5th MT base) OR no weight bearing (4 steps).
- Imaging:
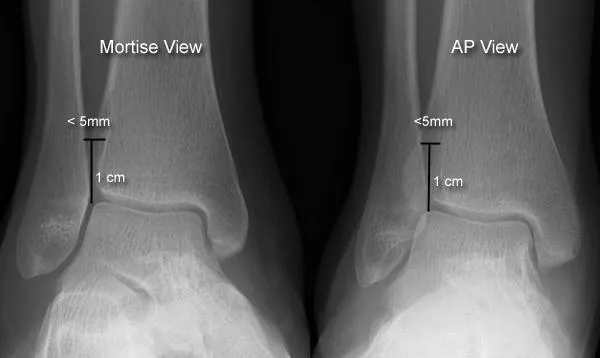
- X-rays: AP, Lateral, Mortise (for syndesmosis; medial clear space, tibiofibular overlap).
- CT: Complex fractures, pre-op planning.
- MRI: Ligamentous/soft tissue injuries.
- X-rays: AP, Lateral, Mortise (for syndesmosis; medial clear space, tibiofibular overlap).
⭐ The mortise view X-ray is crucial for assessing ankle joint congruity; a medial clear space >4mm suggests deltoid ligament injury and instability.
Management Principles - Mending Methods
Principles: Anatomical reduction, stable internal fixation, early mobilization.
- Non-Operative Treatment:
- Indications: Stable, undisplaced fractures (e.g., isolated Weber A).
- Methods: Below-knee cast, walking boot.
- Operative Treatment (ORIF):
- Indications: Unstable fractures, displaced fractures >2mm, open fractures, syndesmotic disruption, bimalleolar/trimalleolar fractures.
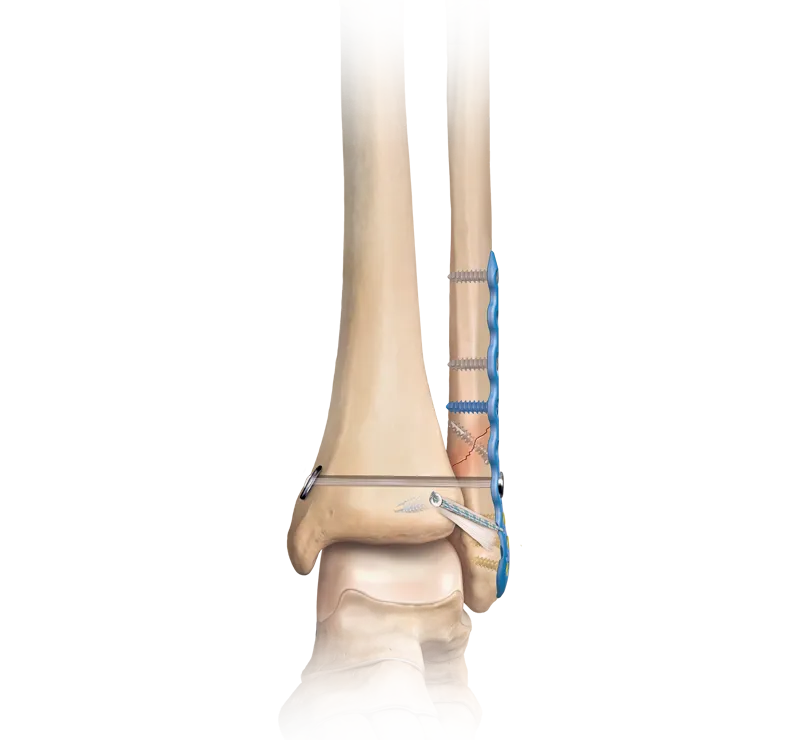
- Techniques:
- Lateral Malleolus: Anatomical plate & screws (lag screw if possible).
- Medial Malleolus: Cannulated screws, anti-glide plate, tension band wiring.
- Posterior Malleolus: Screws (direct posterior/posterolateral approach), buttress plate.
- Syndesmosis: Screws (e.g., 1-2 trans-syndesmotic screws, 3 or 4 cortices), suture button devices.
⭐ Anatomical reduction of the ankle mortise is paramount; even 1mm of lateral talar shift can reduce the tibiotalar contact area by approximately 42%, leading to early arthritis.
Complications - Pitfalls & Problems
- Early:
- Wound infection, skin necrosis
- Neurovascular injury (nerve/vessel)
- Compartment syndrome (↑ pressure)
- DVT/PE
- Late:
- Malunion (deformity), nonunion (no union)
- Stiffness, ↓ range of motion
- Post-traumatic osteoarthritis (PTOA)
- Implant issues (pain, loosening)
- Chronic pain, CRPS
⭐ Post-traumatic osteoarthritis is the most common long-term complication following an ankle fracture, particularly if anatomical reduction is not achieved.
High‑Yield Points - ⚡ Biggest Takeaways
- Lauge-Hansen classification: mechanism-based (foot position, deforming force).
- Weber classification: fibular fracture level relative to syndesmosis (A: infra-, B: trans-, C: supra-).
- Maisonneuve fracture: proximal fibula fracture + syndesmotic injury ± medial injury.
- Tillaux fracture: Salter-Harris III of anterolateral distal tibial epiphysis.
- Bosworth fracture-dislocation: rare, irreducible posterior fibular dislocation.
- Unstable syndesmotic injuries often require surgical fixation.
- Trimalleolar fracture involves medial, lateral, and posterior malleoli.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

