Achilles Anatomy & Biomechanics - Foundation First
- Origin: Gastrocnemius & Soleus muscles.
- Insertion: Calcaneus (posterior aspect).
- Nerve Supply: Tibial nerve (S1, S2).
- Blood Supply: Branches from posterior tibial & peroneal arteries.
- Critical watershed zone: 2-6 cm proximal to insertion (hypovascular).
- Biomechanics:
- Primary ankle plantarflexor.
- Essential for push-off during gait.
- Absorbs high tensile forces.
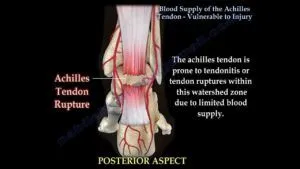
⭐ The watershed area of the Achilles tendon, 2-6 cm proximal to its insertion, is prone to rupture due to relatively poor vascularity.
Achilles Tendinopathy - Wear & Tear Woes
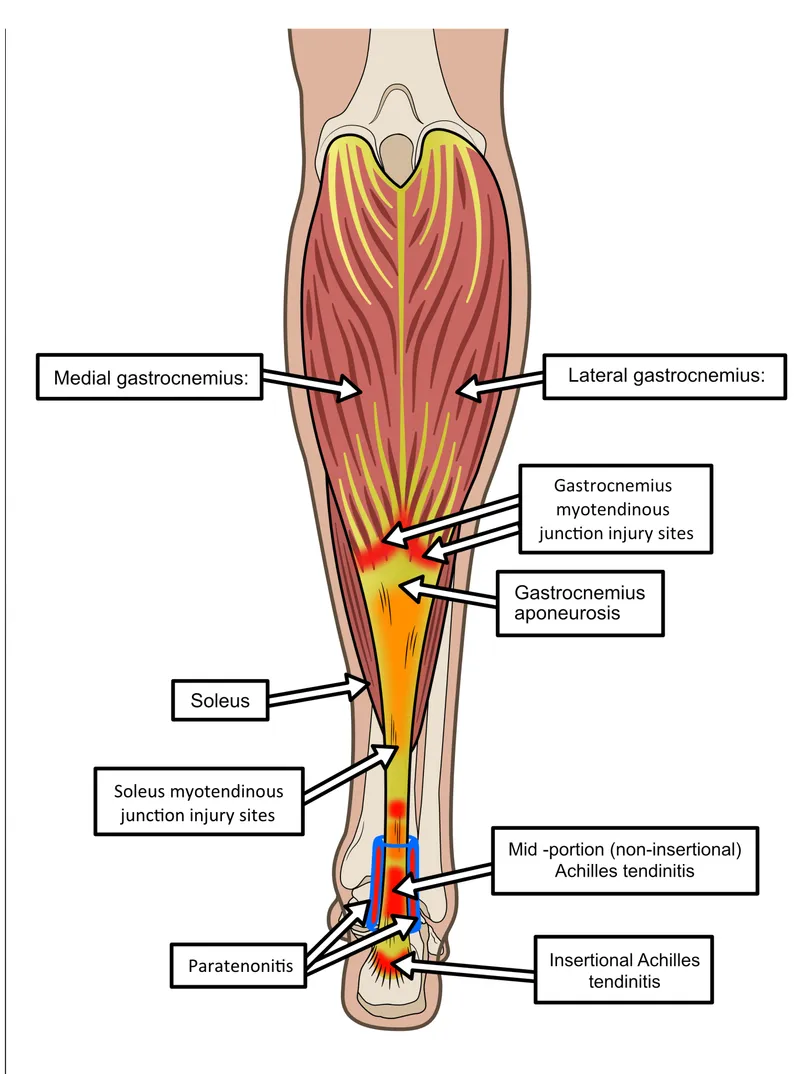
Types:
| Feature | Non-insertional Tendinopathy | Insertional Tendinopathy |
|---|---|---|
| Location | 2-7 cm proximal to calcaneal insertion | At tendon-bone interface (calcaneus) |
| Pathology | Fusiform swelling, mucoid degeneration | May involve retrocalcaneal bursa, enthesophytes |
- Overuse, training errors (↑ intensity/duration), poor footwear.
- Systemic: Fluoroquinolones, inflammatory arthropathies.
- Biomechanical: Pes planus/cavus, hindfoot malalignment, tight gastro-soleus.
Clinical Features:
- Activity-related pain, morning stiffness.
- Localized tenderness, palpable nodule/thickening.
- Painful arc sign (tender area moves with ankle motion).
Conservative Management (First-line):
- Activity modification, RICE. NSAIDs for pain.
- Eccentric loading exercises (Alfredson protocol) - cornerstone.
- Heel lifts/orthotics. ESWT for chronic cases.
⭐ The Alfredson protocol, involving eccentric heel-drop exercises, is a cornerstone of conservative management for Achilles tendinopathy.
Surgical Indications:
- Failure of >6 months comprehensive conservative Rx.
- Options: Debridement, +/- tendon transfer (e.g., FHL).
Management Flow:
Achilles Tendon Rupture - Snap, Crackle, Pop!
-
Epidemiology: 'Weekend warriors', males 30-50 yrs; hx tendinopathy, fluoroquinolone/steroid use.
-
Mechanism: Sudden eccentric load on dorsiflexed ankle; direct trauma.
-
Clinical: Audible 'pop'/'snap', sudden severe posterior ankle pain, ↓ ability to push off, palpable gap.
-
Diagnosis:
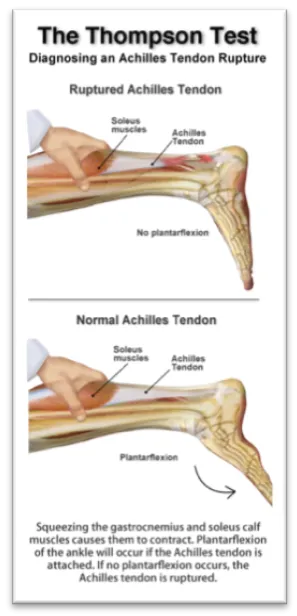
- Thompson test (Simmonds' squeeze): No plantarflexion on calf squeeze (most reliable). 📌 'No Squeeze, No Flex'.
- Matles test, O'Brien test (needle).
-
Imaging:
- Ultrasound: Confirms diagnosis, assesses gap (dynamic, cost-effective).
- MRI: Chronic/missed cases, surgical planning.
-
Management: Controversial. See table and flowchart below.
Rx Indications Outcome Profile Conservative Older, low-demand, comorbidities, gap <1 cm Higher re-rupture; Lower complications Surgical Active, athletes, larger gaps (>1 cm) Lower re-rupture; Higher complications (infection, sural nerve injury)
⭐ A positive Thompson test (absence of passive plantarflexion on calf squeeze) is highly specific for a complete Achilles tendon rupture.
Associated Conditions & Imaging - The Full Picture
- Haglund's Deformity ('Pump Bump'):
- Posterosuperior calcaneal prominence.
- Assoc: Retrocalcaneal bursitis, insertional tendinopathy.
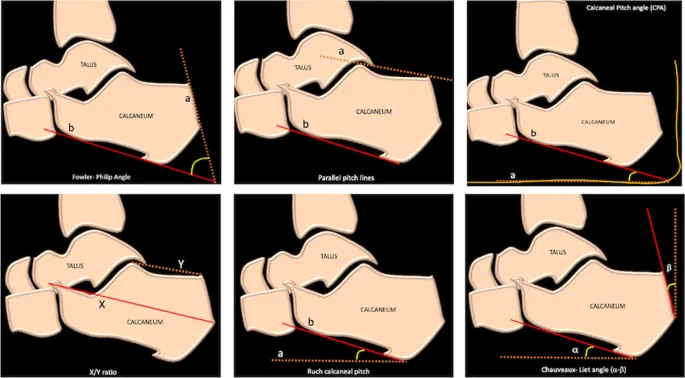
- X-ray: Fowler-Philip angle >75°.
- Retrocalcaneal Bursitis:
- Inflammation: Bursa between Achilles & calcaneus.
- Pain anterior to tendon insertion.
- Sever's Disease (Calcaneal Apophysitis):
- Traction apophysitis at Achilles insertion.
- Age: 8-14 years (skeletally immature).
- Activity-related heel pain, positive squeeze test.
- Paratenonitis:
- Paratenon sheath inflammation; crepitus.
⭐ Haglund's deformity: prominent posterosuperior calcaneal tuberosity, often causes retrocalcaneal bursitis & insertional Achilles tendinopathy.
- Imaging Summary:
- X-ray: Haglund's (Fowler-Philip angle >75°), calcifications, enthesophytes; Sever's (sclerosis/fragmentation).
- USG: Tendon thickening/tears, neovascularization (Doppler), bursitis, paratenon fluid.
- MRI: Gold standard for soft tissue; pre-op planning (complex cases).
High‑Yield Points - ⚡ Biggest Takeaways
- Achilles tendinopathy: Pain 2-6 cm proximal to insertion; Thompson test negative.
- Achilles rupture: Sudden "pop", positive Thompson test; common in "weekend warriors".
- Insertional tendinopathy: Pain at posterior heel insertion, often with Haglund's deformity.
- Key risk factors: Fluoroquinolones, corticosteroids, male sex, age >30.
- Diagnosis: Primarily clinical; Ultrasound confirms rupture or assesses tendinopathy.
- Tendinopathy treatment: Eccentric exercises are mainstay.
- Rupture treatment: Surgical repair (lower re-rupture) vs. conservative management (casting/bracing).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

