Bone Cells & ECM - Tiny Bone Builders
- Osteoblasts: Bone-forming cells from MSCs.
- Synthesize osteoid (unmineralized matrix): Type I collagen, osteocalcin.
- Marker: Alkaline Phosphatase (ALP).
- Osteocytes: Mature osteoblasts in lacunae; mechanosensors.
- Regulate osteoblast/osteoclast activity.
⭐ Osteocytes are the most abundant bone cells (90-95%), acting as master regulators.
- Osteoclasts: Bone-resorbing multinucleated cells from hematopoietic stem cells (monocyte-macrophage).
- In Howship's lacunae; create acidic environment.
- Markers: TRAP, Cathepsin K.
- Bone Lining Cells: Quiescent osteoblast derivatives on resting bone surfaces.
- Extracellular Matrix (ECM):
- Organic (~35%): Type I collagen (tensile strength), proteoglycans.
- Inorganic (~65%): Hydroxyapatite $Ca_{10}(PO_4)_6(OH)_2$ (compressive strength).
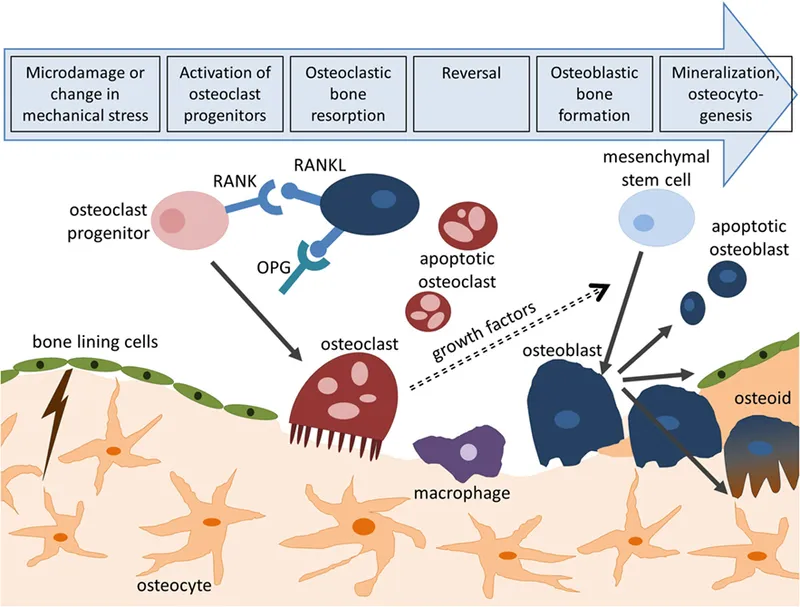
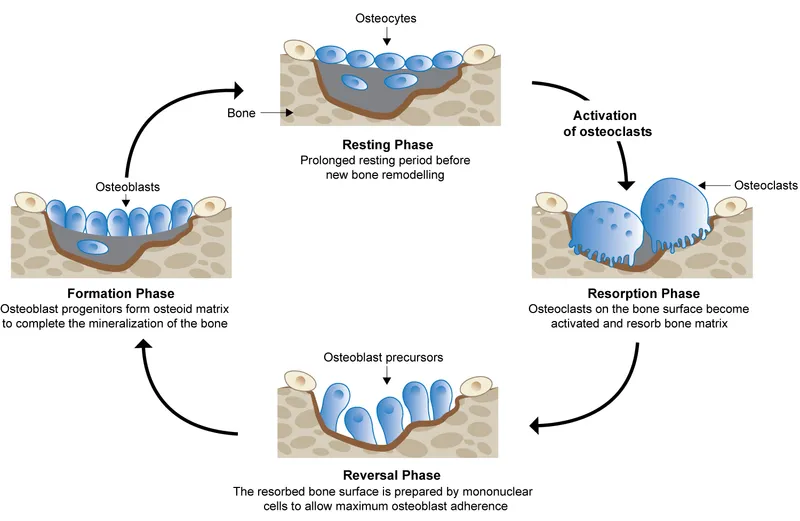
Bone Remodeling Cycle - Renew & Rebuild
Continuous, lifelong physiological process where old or damaged bone is resorbed and replaced by new, healthy bone. Essential for skeletal integrity, micro-damage repair, and calcium/phosphorus homeostasis. Orchestrated by Basic Multicellular Units (BMUs).
📌 Mnemonic for phases: ARRF-Q (Activation, Resorption, Reversal, Formation, Quiescence)
- Key Cells:
- Osteoclasts (OCs): Resorb bone (Howship's lacunae). Stimulated by RANKL.
- Osteoblasts (OBs): Form new bone (osteoid). Promote OPG to inhibit OCs.
- Coupling: Resorption & formation tightly linked; imbalance leads to bone pathology.
- Duration: Cycle ~4-6 months (trabecular); significantly longer for cortical bone.
- Key Regulators: PTH, Vitamin D, Calcitonin, Estrogen, androgens, mechanical load.
⭐ The OPG/RANKL ratio is pivotal: ↑OPG/RANKL favors bone formation by inhibiting osteoclastogenesis, ↓OPG/RANKL favors resorption.
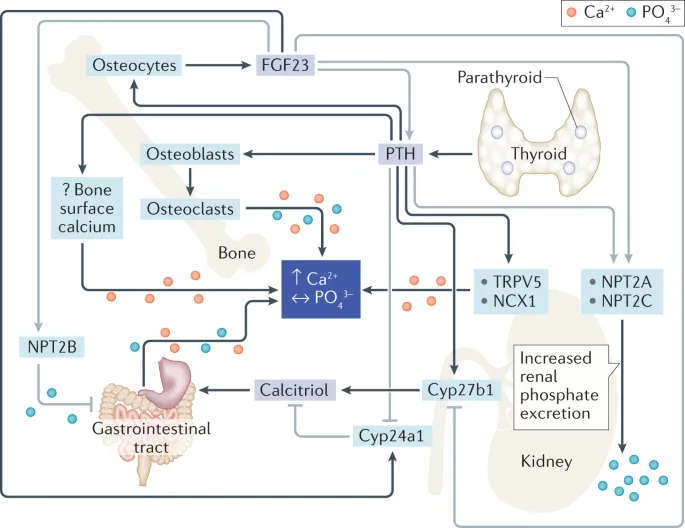
Hormonal Control Tower - Bone's Bosses
- Parathyroid Hormone (PTH): Chief Ca²⁺ regulator. 📌 PTH = Phosphate Trashing Hormone (↓ renal PO₄³⁻ reabsorption) & Pushes The Calcium High.
- Source: Parathyroid glands.
- Action: ↑ serum Ca²⁺, ↓ serum PO₄³⁻.
- Bone: Primarily ↑ resorption (indirectly, via RANKL on osteoblasts stimulating osteoclasts).
- Kidney: ↑ Ca²⁺ reabsorption, ↓ PO₄³⁻ reabsorption, ↑ $1,25(OH)_2D_3$ synthesis.
- Vitamin D (Calcitriol - $1,25(OH)_2D_3$): Ca²⁺ & PO₄³⁻ absorption champion.
- Source: Skin (UV), diet; activated in liver (25-OH) then kidney ($1,25(OH)_2D_3$).
- Action: ↑ serum Ca²⁺ & ↑ serum PO₄³⁻.
- Intestine: Major site for ↑ Ca²⁺ & PO₄³⁻ absorption.
- Bone: Promotes mineralization; regulates osteoblast/osteoclast activity.
- Calcitonin: "Tones down" serum Ca²⁺.
- Source: Thyroid C-cells (parafollicular cells).
- Action: ↓ serum Ca²⁺ (minor physiological role in humans).
- Bone: ↓ osteoclast activity.
- Other Influencers:
- Estrogen: ↓ bone resorption (protects bone). Deficiency → osteoporosis.
- Glucocorticoids (chronic excess): ↓ bone formation, ↑ bone resorption → osteoporosis.
- Growth Hormone (GH)/IGF-1: Stimulate bone formation & longitudinal growth.
- Thyroid Hormones (T3/T4): Essential for skeletal development; excess → ↑ turnover, net bone loss.
⭐ PTH exhibits a dual effect: continuous high levels promote bone resorption, whereas intermittent low-dose administration (e.g., Teriparatide) is anabolic, stimulating bone formation and is used to treat osteoporosis.
Key Minerals & Markers - CaP & Clues
- Key Minerals:
- Calcium (Ca): Serum 8.5-10.5 mg/dL; Ionized 4.5-5.6 mg/dL (active).
- Phosphorus (P): Serum 2.5-4.5 mg/dL.
- Ca x P product: > 55-60 mg²/dL² → ↑ risk soft tissue calcification.
- Bone Formation Markers (Osteoblast ↑):
- Alkaline Phosphatase (ALP): Total & Bone-Specific (BSAP).
- Osteocalcin (OC).
- Procollagen type I N-terminal propeptide (PINP).
- Bone Resorption Markers (Osteoclast ↑):
- C-telopeptide of type I collagen (CTX) - serum/urine.
- N-telopeptide of type I collagen (NTX) - urine.
- Tartrate-Resistant Acid Phosphatase (TRAP 5b).
⭐ PINP (formation) and CTX (resorption) are highly sensitive Bone Turnover Markers (BTMs).
High‑Yield Points - ⚡ Biggest Takeaways
- Wolff's Law: Bone remodels based on applied load.
- Osteoblasts (bone formation) are identified by ALP and Osteocalcin.
- Osteoclasts (resorb bone), marked by TRAP, are regulated by RANKL/OPG.
- PTH elevates serum Ca²⁺ by stimulating osteoclasts; Calcitonin has the opposite effect.
- Vitamin D is essential for calcium absorption and bone mineralization.
- Estrogen deficiency accelerates bone resorption, leading to postmenopausal osteoporosis.
- Bisphosphonates and Denosumab are key drugs inhibiting osteoclast function.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

