AK Basics - Shaping Sight
- Goal: Surgically correct astigmatism by reshaping the cornea.
- Mechanism: Peripheral corneal incisions (transverse or arcuate) flatten the steepest meridian.
- Effect: Improves vision by reducing astigmatic error.
- Coupling: Flattening in incised meridian couples with steepening in orthogonal meridian (coupling ratio, e.g., $1:1$).
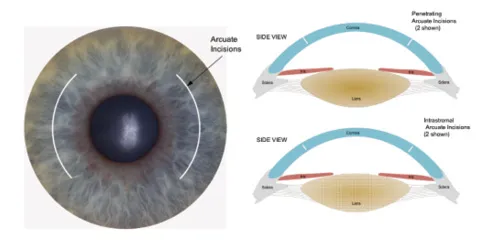
⭐ AK primarily corrects naturally occurring astigmatism but is also valuable for managing post-cataract surgery or post-penetrating keratoplasty (PKP) astigmatism.
Patient Selection - Ideal Candidates
- Age >18 years, stable refraction (≥1 year).
- Regular, symmetric corneal astigmatism (1-4D).
- Adequate Central Corneal Thickness (CCT).
- Normal corneal topography (no ectasia/keratoconus).
- Realistic patient expectations.
- No active ocular disease, severe dry eye.
⭐ AK is less predictable for high astigmatism (typically >4D) compared to excimer laser procedures like LASIK or PRK.
Incisions & Techniques - Precision Cuts
- Incision Types:
- Arcuate (curved): Most common; follow corneal curvature.
- Transverse (straight/linear): Less common.
- Paired incisions: Often used for symmetrical effect.
- Critical Parameters:
- Depth: 85-95% of peripheral corneal thickness.
- Optical Zone (OZ): Typically 6.0-8.0 mm. Smaller OZ = ↑ effect.
- Length & Number: Guided by nomograms; ↑ length/number = ↑ correction.
- Placement: Along the steepest corneal meridian.
- Nomograms: Essential for planning; consider patient age, magnitude & axis of astigmatism.
- Surgical Tools: Diamond knife (manual) or Femtosecond laser (for enhanced precision & safety).
- Coupling Effect: Flattening in incised meridian, steepening 90° away (ratio varies, ideally 1:1).
⭐ Arcuate incisions placed at a larger optical zone (e.g., >7 mm) have less corrective effect but induce less irregular astigmatism and glare compared to smaller OZ incisions for the same correction amount.
Potential Pitfalls - Complication Corner
⭐ Corneal perforation is a significant intraoperative complication, risk increased by inaccurate pachymetry or excessive incision depth.
| Phase | Complication | Management |
|---|---|---|
| Intra-op | Corneal Perforation | Stop procedure, suture defect, consider aborting |
| Incision Errors | Recalculate, adjust; may need secondary procedure | |
| Microperforation | Often self-sealing; bandage contact lens (BCL) | |
| Post-op | Refractive Surprise | Spectacles, contact lenses, surgical enhancement |
| Irregular Astigmatism | RGP lenses, CXL, topography-guided ablation | |
| Glare/Halos | Usually transient; topical brimonidine | |
| Infection (Keratitis) | Intensive fortified topical antibiotics | |
| Wound Dehiscence | Resuturing of incision |
Aftercare & Results - Vision Victory
- Post-op Care:
- Topical antibiotics & steroids (tapered schedule).
- Frequent lubricating eye drops for comfort.
- Protective eye shield, especially at night initially.
- Expected Outcomes:
- Significant ↓ in astigmatism; improved Uncorrected Visual Acuity (UCVA).
- Vision typically stabilizes within 1-3 months.
- High patient satisfaction is common.
- Predictability & Enhancements: Good with modern nomograms; enhancements possible if needed.
⭐ Undercorrection is more common than overcorrection with modern AK techniques and nomograms. oka
High‑Yield Points - ⚡ Biggest Takeaways
- Astigmatic Keratotomy (AK) corrects astigmatism with corneal incisions in the steepest meridian.
- Incisions cause flattening in that meridian, steepening 90° away (coupling effect).
- Arcuate incisions are common; Limbal Relaxing Incisions (LRIs) are peripheral AK, often with cataract surgery.
- Effect determined by incision depth (target 85-95% stroma), length, and optical zone.
- Risks: Over/undercorrection, irregular astigmatism, glare, infection, perforation.
- Used for low to moderate regular astigmatism; results less predictable than laser_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

