TED Pathogenesis - Autoimmune Attack
- Primary Antigen: Thyrotropin receptor (TSH-R) on orbital fibroblasts & thyrocytes.
- Autoantibodies: TSH-R antibodies (TRAbs), particularly stimulating antibodies (TSI), cross-react with TSH-R on orbital fibroblasts.
- Orbital Fibroblast Activation: Leads to:
- Adipogenesis (↑ fat volume).
- Glycosaminoglycan (GAG) production (e.g., hyaluronic acid) → osmotic swelling.
- Release of pro-inflammatory cytokines (TNF-α, IL-1, IL-6).
- Immune Cells: T-cells & B-cells infiltrate orbit, perpetuating inflammation.
- Consequences: Muscle swelling, proptosis, optic nerve compression.
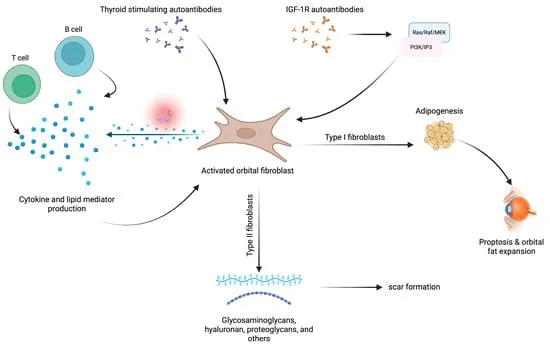
⭐ Orbital fibroblasts are the key effector cells in TED, differentiating into adipocytes and myofibroblasts, and producing excess GAGs under autoimmune stimulation, primarily by TSH-R antibodies and IGF-1R activation pathway.
📌 Mnemonic: TSH-R Antibodies Go For Orbits (TSH-R Antibodies, GAGs, Fibroblasts, Orbitopathy).
Clinical Showcase - Grave Signs
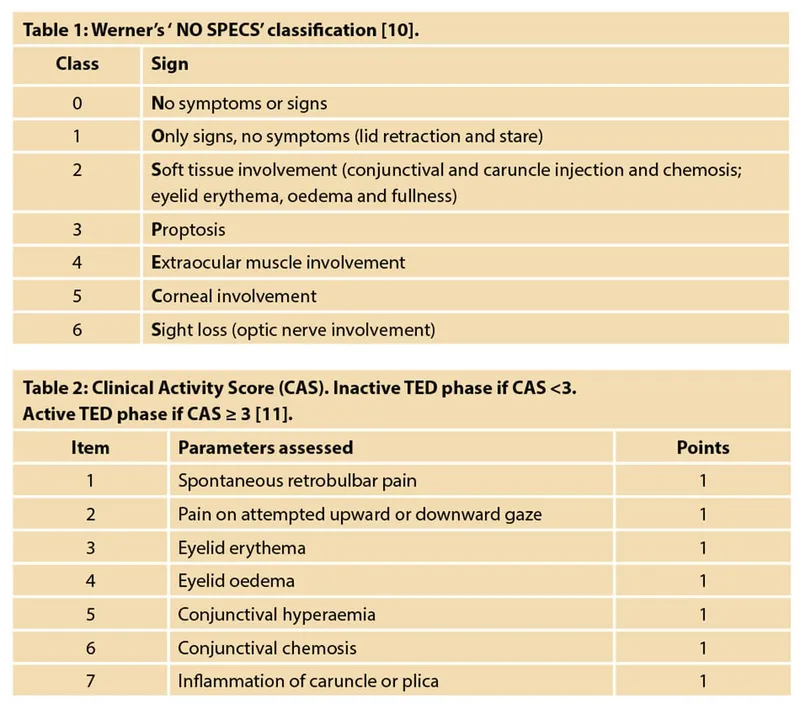
- Signs follow 📌 NOSPECS classification (severity increases down the list):
- No signs/symptoms.
- Only signs (no symptoms):
- Lid retraction (Dalrymple's sign: stare).
- Lid lag (von Graefe's sign: on downgaze).
- Soft tissue involvement: Periorbital edema, chemosis, conjunctival injection, lid fullness.
- Proptosis: Axial globe displacement > 21mm (Hertel exophthalmometer). Often asymmetric.
- Extraocular muscle (EOM) involvement: Diplopia due to restrictive myopathy.
- Common order of involvement: Inferior Rectus (IR), Medial Rectus (MR), Superior Rectus (SR), Lateral Rectus (LR) (📌 IMSLO).
- Corneal involvement: Exposure keratopathy from proptosis & lid retraction; leads to punctate erosions, ulceration.
- Sight loss (Optic Neuropathy): Due to optic nerve compression by enlarged EOMs at orbital apex. Presents with ↓ visual acuity, ↓ color vision, Relative Afferent Pupillary Defect (RAPD).
⭐ The Inferior Rectus is the most commonly affected extraocular muscle, leading to vertical diplopia (worse on upgaze) and restricted elevation of the eye.
Diagnostic Toolkit - Unmasking TED
- Clinical Suspicion: Proptosis, lid retraction (Darlymple's sign), diplopia, compressive optic neuropathy.
- Lab Confirmation:
- TFTs: TSH, fT3, fT4 (patient may be hyper-, hypo-, or euthyroid).
- Autoantibodies: TRAb (Thyroid Stimulating Hormone Receptor Ab) highly specific; Anti-TPO Ab.
- Orbital Imaging (CT/MRI):
- Fusiform EOM belly enlargement, tendon sparing (key feature).
- Apical crowding, optic nerve changes.
- 📌 IMSLOw: Common EOM involvement order (Inferior > Medial > Superior > Lateral > Obliques).
- Activity Assessment:
- Clinical Activity Score (CAS): Assesses 7 inflammatory parameters. Score ≥ 3/7 indicates active disease requiring potential immunomodulation.
- Severity Grading:
- EUGOGO classification (Mild, Moderate-to-Severe, Sight-threatening).
- NOSPECS classification (0-No signs/symptoms, 1-Only signs, 2-Soft tissue, 3-Proptosis, 4-EOM, 5-Cornea, 6-Sight loss).
⭐ In TED, extraocular muscle enlargement typically spares the tendons, a key differentiator from orbital myositis where tendons are often involved.
Treatment Playbook - Orbital Rescue
⭐ Teprotumumab, an IGF-1R inhibitor, is a significant advancement for active, moderate-to-severe Thyroid Eye Disease, reducing proptosis and diplopia.
High‑Yield Points - ⚡ Biggest Takeaways
- Most common cause of adult proptosis, often bilateral.
- Autoimmune, strongly linked to Graves' disease; can occur in euthyroid/hypothyroid states.
- Key pathology: Glycosaminoglycan (GAG) deposition and fibroblast proliferation in orbital tissues.
- NO SPECS mnemonic guides clinical assessment of severity.
- Inferior rectus (IR) and medial rectus (MR) most affected, causing diplopia and motility restriction.
- Dysthyroid Optic Neuropathy (DON) from apical compression is a major sight threat; smoking cessation is crucial_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

