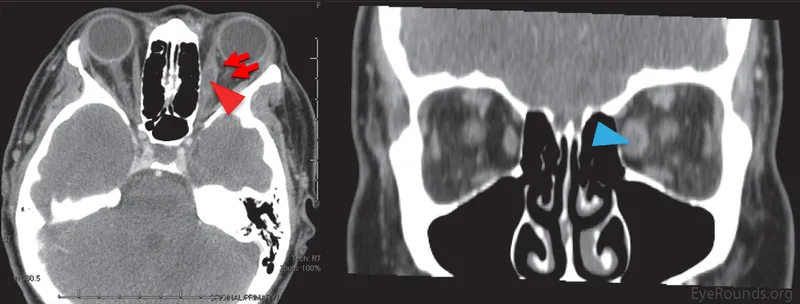
Orbital Cellulitis - Eyelid Emergency
Infection posterior to orbital septum. Sight-threatening emergency.
- Etiology:
- Most common: Ethmoid sinusitis (>90%).
- Others: Dacryocystitis, dental infection, trauma.
- Key Differentiator from Preseptal:
- Preseptal: No proptosis, normal vision & eye movements.
- Clinical Triad (📌 POV):
- Proptosis (painful)
- Ophthalmoplegia (painful)
- Vision ↓ (may include RAPD)
- Other Signs: Eyelid edema, erythema, chemosis, fever.
- Diagnosis: CT scan (orbit & sinuses) gold standard.
- Management:
- Urgent hospital admission.
- IV broad-spectrum antibiotics (e.g., Vancomycin + Ceftriaxone).
- Surgical drainage if abscess, no improvement in 24-48 hrs, or vision decline.
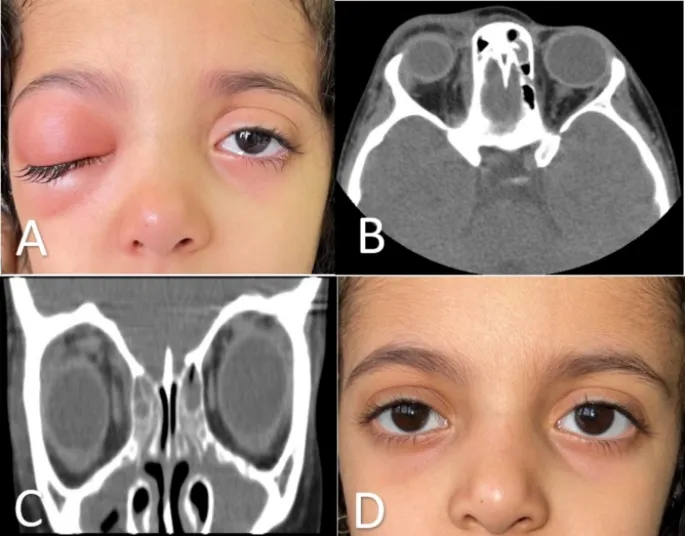
⭐ Orbital cellulitis is distinguished from preseptal cellulitis by the presence of proptosis, painful ophthalmoplegia, and/or decreased visual acuity.
Thyroid Eye Disease - Graves' Gaze
- Autoimmune disorder; most common cause of bilateral/unilateral proptosis in adults.
- Associated with Graves' hyperthyroidism; can be euthyroid or hypothyroid.
- Pathophysiology: TSH receptor antibodies (TRAb) stimulate orbital fibroblasts → glycosaminoglycan (GAG) deposition & adipogenesis → extraocular muscle (EOM) & orbital fat expansion.
- Key Gaze-Related Signs:
- Proptosis (Exophthalmos): Axial, non-pulsatile.
- Eyelid Retraction (Dalrymple's sign): Staring appearance.
- Lid Lag on Downgaze (Von Graefe's sign).
- Restrictive Myopathy: Diplopia, ↑IOP on upgaze/side gaze.
- 📌 Mnemonic for EOM involvement: "I'M SLOW" (IR → MR → SR → LR → Obliques).
- Compressive Optic Neuropathy (DON): Risk of vision loss.
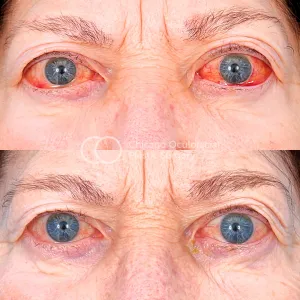
- Investigations: TFTs (TSH, T3, T4, TRAb), CT/MRI orbits (fusiform EOM belly enlargement, tendon sparing).
- Management: Control thyroid status. Mild: lubricants. Active moderate-severe: IV corticosteroids, orbital radiotherapy, teprotumumab. Inactive/Stable: orbital decompression, strabismus surgery, eyelid surgery.
⭐ The Inferior Rectus (IR) is the most commonly involved extraocular muscle, leading to restricted elevation and vertical diplopia looking up.
Idiopathic Orbital Inflammation - Enigmatic Eyes
- A.k.a. Orbital Pseudotumor. Idiopathic, non-granulomatous orbital inflammation; diagnosis of exclusion.
- Clinical: Acute unilateral pain, proptosis, diplopia, ↓ vision, eyelid edema, chemosis.
- Bilateral cases: suspect systemic disease (e.g., GPA, sarcoidosis).
- Types: Myositis (most common), dacryoadenitis, anterior (scleritis/uveitis), apical, diffuse.
- Investigations:
- CT/MRI: Diffuse infiltration, muscle enlargement (tendons spared vs. TED), lacrimal gland.
- Biopsy: Rules out malignancy/infection; shows non-specific inflammation.
- Treatment:
- Corticosteroids (Prednisolone 1-1.5 mg/kg/day): Rapid, dramatic response is characteristic.
- Radiotherapy for steroid-resistant/dependent cases.
- Immunosuppressants (methotrexate) for refractory cases.
⭐ Tolosa-Hunt Syndrome: IOI of cavernous sinus/SOF, causing painful ophthalmoplegia.
Other Key Inflammations - Orbital Oddities
- Fungal Infections:
- Mucormycosis (ROCM): Aggressive. Risk: Diabetes, immunosuppression. Signs: Black eschar, proptosis, ophthalmoplegia. Dx: Biopsy (non-septate hyphae, $90°$ branching). Rx: Amphotericin B, surgery.
- Aspergillosis: Invasive or allergic forms. Dx: Biopsy (septate hyphae, acute-angle branching).
- Idiopathic Inflammations:
- Orbital Pseudotumor (IOIS): Painful proptosis, diplopia, restricted motility. Dramatic steroid response.
- Tolosa-Hunt Syndrome: Painful ophthalmoplegia (CN III, IV, V1, VI). Granulomatous. Steroid responsive.
- Systemic Associations:
- Sarcoidosis: Dacryoadenitis, uveitis, optic neuropathy.
- GPA (Wegener's): Proptosis, scleritis, NLD obstruction. c-ANCA+.

⭐ Biopsy finding in Mucormycosis: broad, non-septate hyphae with wide-angle ($90°$) branching, is a key diagnostic feature.
High‑Yield Points - ⚡ Biggest Takeaways
- Orbital cellulitis: Post-septal infection, often from sinusitis; causes proptosis, painful ophthalmoplegia, ↓vision.
- Preseptal cellulitis: Anterior to septum; eyelid swelling, but no proptosis or ophthalmoplegia.
- Thyroid Eye Disease (TED): Most common cause of adult proptosis (uni/bilateral); follow NO SPECS.
- Idiopathic Orbital Inflammation (IOI): Painful proptosis and ophthalmoplegia; diagnosis of exclusion.
- Tolosa-Hunt Syndrome: Inflammation of cavernous sinus/SOF causing painful ophthalmoplegia; responds to steroids.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more