Definitions & Etiology - Gasping for Glossary
- Birth Asphyxia: Impaired placental or pulmonary gas exchange leading to fetal hypoxemia & hypercapnia.
- Hypoxic-Ischemic Encephalopathy (HIE): Neurological dysfunction resulting from birth asphyxia.
- Etiology (Intrapartum Events Most Common):
- Maternal: Placental abruption, uterine rupture, severe hypotension.
- Fetal: Cord prolapse/compression, nuchal cord.
- Utero-placental insufficiency.
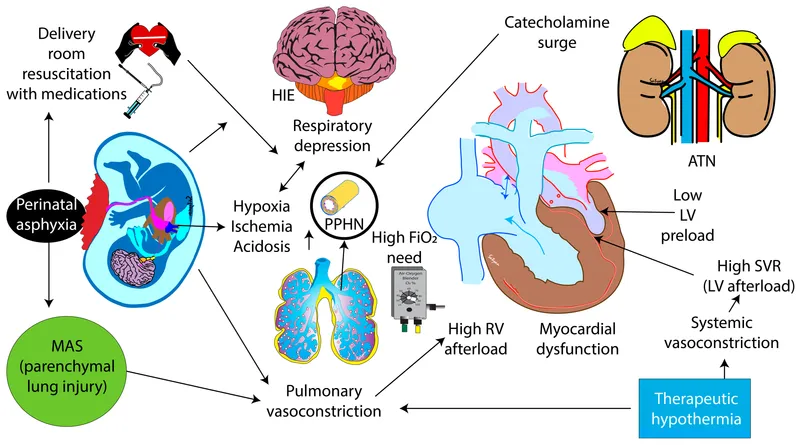
⭐ Apgar scores at 1 and 5 minutes are crucial indicators, but HIE diagnosis relies on a broader clinical picture including acidosis (pH < 7.0 or base deficit ≥ 12 mmol/L) and neurological signs.
Pathophysiology of HIE - Brain's Energy Crash
Brain injury in Hypoxic-Ischemic Encephalopathy (HIE) unfolds in phases:
- Primary Energy Failure (Minutes)
- Hypoxia/ischemia → ↓ ATP.
- Na⁺/K⁺ pump fails → cell swelling.
- Anaerobic glycolysis → ↑ lactic acid ($CH_3CH(OH)COOH$).
- Early glutamate release.
- Latent Phase (Reperfusion: 1-6 hours)
- Brief, partial restoration of cerebral metabolism.
- Crucial therapeutic window.
⭐ The 'latent phase' between primary and secondary energy failure (typically lasting 1-6 hours) represents a critical therapeutic window for neuroprotective interventions.
- Secondary Energy Failure (Hours to Days: 6-72 hours)
- Mitochondrial dysfunction.
- Excitotoxicity: ↑ glutamate, ↑ Ca²⁺ influx.
- Oxidative stress: free radical damage.
- Inflammation: cytokine release.
- Leads to apoptosis & necrosis.
Clinical Features & Staging - Sarnat's Symptom Scan
- Assesses HIE severity via clinical signs & EEG.
- Guides prognosis & therapeutic hypothermia.
| Feature | Stage I (Mild HIE) | Stage II (Moderate HIE) | Stage III (Severe HIE) |
|---|---|---|---|
| Consciousness | Hyperalert, irritable | Lethargic, obtunded | Stuporous, comatose |
| Muscle Tone | Normal or mild hypo | Significant hypotonia | Flaccid |
| Reflexes (primitive) | Exaggerated | Overactive/Suppressed | Absent |
| Autonomic Signs | Sympathetic excess | Parasympathetic excess | Both systems depressed |
| Seizures | None | Frequent, focal/multi | Infrequent; decerebration |
| EEG | Normal / mild diffuse | Seizures, low voltage | Burst-suppression / flat |
Management & Prognosis - Chill, Control, Conquer
- Immediate: Stabilize (NRP), identify HIE.
- Therapeutic Hypothermia (Cooling): Neuroprotection.
-
Criteria: ≥36wks GA, <6hrs old, mod-severe HIE.
-
Target: 33.5-34.5°C for 72hrs (within 6hrs birth).
-
Rewarm: Slow (0.2-0.5°C/hr).
-
- Key Supportive Care: ABCs; seizure control (phenobarbital); normoglycemia.
- Prognosis: Sarnat score. MRI (Day 7-14), EEG. Long-term: CP, epilepsy, delay.
⭐ Therapeutic hypothermia, when initiated within 6 hours of birth for moderate to severe HIE in term/near-term infants, significantly reduces mortality and major neurodevelopmental disability at 18-24 months.
High‑Yield Points - ⚡ Biggest Takeaways
- Birth asphyxia: Defined by intrapartum hypoxia-ischemia causing multi-organ dysfunction.
- APGAR scores: Persistently low (<7 at 5-10 min) are significant for HIE.
- Sarnat Staging: Clinically grades HIE (I-III) by consciousness, tone, seizures.
- Therapeutic Hypothermia: Key for mod/sev HIE; start <6h, cool 33.5-34.5°C for 72h.
- Key causes: Placental abruption, cord prolapse, uterine rupture.
- Cord blood gas: ↑lactate, ↓pH, and significant base deficit are diagnostic.
- Long-term risks: Cerebral palsy, epilepsy, cognitive impairment.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

