Hyperemesis Gravidarum: Intro & Risks - Beyond Morning Sickness
- Severe, intractable nausea & vomiting of pregnancy (NVP).
- Diagnostic pointers:
- Persistent vomiting unrelated to other causes
- Weight loss >5% of pre-pregnancy body weight
- Ketonuria, dehydration
- Electrolyte imbalances (e.g., hypokalemia)
- Onset usually <9 weeks gestation; often resolves by 20 weeks.
- Risk Factors:
- Multiple gestation (e.g., twins)
- Molar pregnancy (hydatidiform mole)
- History of HG in prior pregnancy
- Female fetus
- Hyperthyroidism
- Nulliparity
⭐ HG is strongly associated with elevated levels of human chorionic gonadotropin (hCG) and estradiol, often seen in molar or multiple pregnancies.
HG Pathophysiology - Hormonal Havoc
- hCG Overdrive: ↑↑ Human Chorionic Gonadotropin (hCG) is a key culprit.
- Specific hCG isoforms are more emetogenic.
- hCG structurally similar to TSH, can stimulate thyroid → gestational transient thyrotoxicosis.
- Estrogen & Progesterone: ↑ Estrogen may sensitize vomiting centers. ↑ Progesterone relaxes GI smooth muscle, delaying gastric emptying.
- GDF15: Placental Growth Differentiation Factor 15 (GDF15) acts directly on brainstem chemoreceptor trigger zone.

⭐ hCG levels often peak around 9-10 weeks gestation, coinciding with the typical peak of HG symptoms.
HG Clinical Features & Diagnosis - Unmasking the Misery
- Key Manifestations:
- Severe, intractable Nausea & Vomiting (NVP).
- Significant weight loss: >5% of pre-pregnancy body weight.
- Ketonuria (marker of starvation).
- Dehydration signs: Tachycardia, hypotension, dry mucous membranes, oliguria.
- Electrolyte imbalances: Hypokalemia, hyponatremia, hypochloremic alkalosis.
- Ptyalism (excessive salivation).
- Rare: Wernicke's encephalopathy (thiamine deficiency).
- Diagnostic Process:
- Primarily a clinical diagnosis of exclusion.
- Rule out other causes (e.g., UTI, gastroenteritis, molar pregnancy, thyroid disease).
-
⭐ Gestational transient thyrotoxicosis (↓TSH, ↑free T4) is common (50-60%), typically resolving by 20 weeks without specific antithyroid treatment.
HG Complications & Workup - Danger Signs
- Maternal:
- Weight loss >5%
- Dehydration, electrolyte imbalance (↓K⁺, ↓Na⁺, alkalosis)
- Ketonuria
- Wernicke's encephalopathy (thiamine deficiency) 📌 (B1)
- Mallory-Weiss tear, liver/renal issues
- Fetal: IUGR, low birth weight, preterm birth.
- Workup:
- Urine ketones, electrolytes, LFTs, RFTs, TSH.
- USG: Exclude molar/multiple pregnancy.
- Danger Signs: Persistent vomiting, weight loss >5%, dehydration (↓urine, tachycardia), neurological symptoms (confusion, ataxia), jaundice.
⭐ Prophylactic thiamine (B1) is crucial in severe HG to prevent Wernicke's encephalopathy.
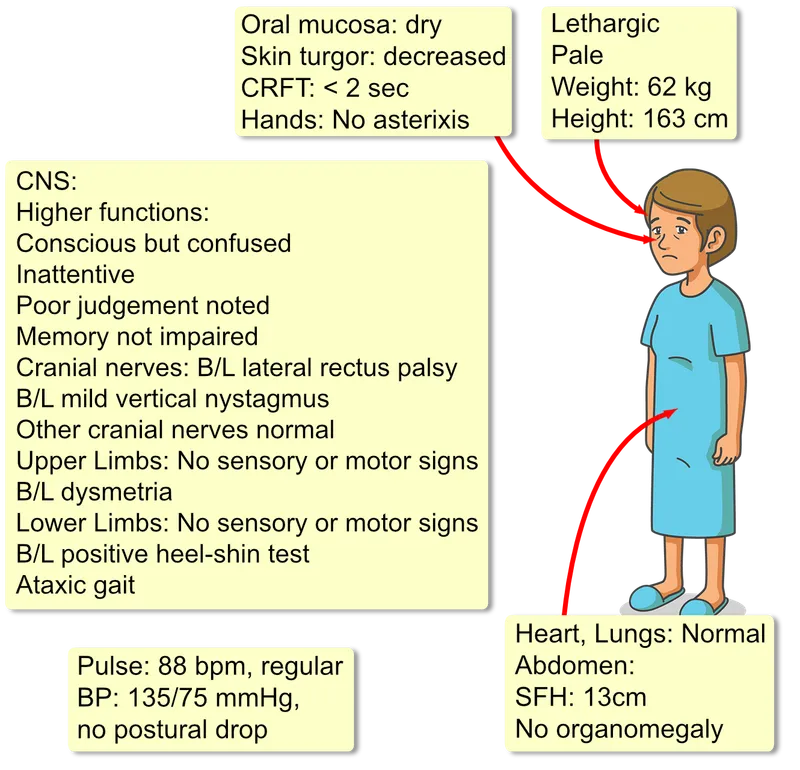
HG Management - Stemming the Storm
- Initial: Small, frequent, bland meals; avoid triggers. Hydration (ORS).
- Pharmacotherapy (Stepwise):
- 1st Line: Pyridoxine (Vit B6) ± Doxylamine.
- 2nd Line: Antihistamines (Promethazine), Dopamine antagonists (Metoclopramide).
- 3rd Line: Ondansetron (⚠️ QTc prolongation; caution in 1st trimester).
- Refractory: Corticosteroids (e.g., Prednisolone 10-20mg TDS, after 10 weeks gestation, taper slowly).
- Severe HG (Inpatient):
- IV fluids: Normal Saline + KCl. Correct dehydration & electrolytes.
- Thiamine 100mg IV/IM daily (prevent Wernicke's).
- Nutritional support: Enteral/Parenteral if oral intake fails.
⭐ In severe HG, always administer thiamine before glucose-containing IV fluids to prevent precipitating Wernicke's encephalopathy.
High‑Yield Points - ⚡ Biggest Takeaways
- Severe NVP causing >5% weight loss, dehydration, ketonuria, and electrolyte imbalance (hypokalemia).
- Onset usually <9 weeks, peaks 10-12 weeks, typically resolves by 20 weeks.
- Strongly linked to high hCG levels (e.g., molar pregnancy, multiple gestations).
- Diagnosis of exclusion: rule out UTI, gastroenteritis, thyrotoxicosis.
- Management: IV hydration, antiemetics (e.g., ondansetron), thiamine to prevent Wernicke's encephalopathy.
- Ptyalism can occur; risk factors include nulliparity and prior HG history.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

