Osteomyelitis - Bone's Fiery Foe
Bone inflammation, typically infectious.
-
Classification by Route:
- Hematogenous (blood-borne)
- Contiguous focus (spread from adjacent infection)
- Direct inoculation (trauma, surgery)
-
Common Pathogens:
- Staphylococcus aureus: Most common overall.
- Neonates: Group B Strep (GBS), E. coli.
- IVDU, Puncture wounds (e.g., foot): Pseudomonas aeruginosa.
-
⭐ In sickle cell disease, Salmonella species are a characteristic cause.
-
Types:
Feature Acute Osteomyelitis Chronic Osteomyelitis Onset Sudden, < 2 weeks Insidious, > 2 weeks Symptoms Fever, intense pain, local inflammation Draining sinus, recurrent pain, deformity X-ray (early) Soft tissue swelling; normal bone Sclerosis, sequestrum, involucrum Pathology Acute inflammation, bone necrosis Dead bone (sequestrum), new bone (involucrum)
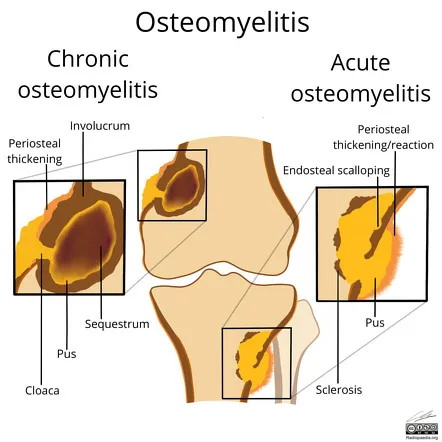
- Diagnosis & Management:
- Antibiotics: Typically 4-6 weeks IV; may be followed by oral.
- Surgical debridement often for chronic cases/abscess.
Septic Arthritis - Joint Under Siege
Bacterial invasion of synovial joint space. A medical emergency requiring prompt diagnosis and treatment.
- Pathogens by Age Group:
- Neonates: GBS, S. aureus, Gram-negative bacilli.
- Children <5y: S. aureus, S. pyogenes.
- Older children/Adults: S. aureus.
- Sexually active: N. gonorrhoeae.
- IVDU: Pseudomonas aeruginosa, S. aureus.
- Synovial Fluid Analysis: WBC >50,000/mm³ (often >100,000), PMNs >75%, ↓Glucose, Gram stain (+ in ~50-70%), Culture (+ in ~70-90%).
- 📌 Kocher's Criteria (Pediatric Septic Hip):
- Fever >38.5°C
- Non-weight bearing
- ESR >40 mm/hr
- WBC >12,000/mm³ (≥3 criteria suggest high probability)
⭐ Kocher criteria are highly useful for differentiating septic arthritis from transient synovitis in children with an irritable hip.
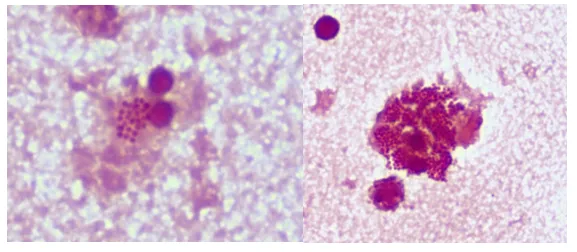
Prosthetic Joint Infections - Implant Invasion
- Infection involving a joint prosthesis and adjacent tissues; biofilm formation on implant is key.
- Classification by Onset & Common Pathogens:
| Onset | Timing | Common Pathogens |
|---|---|---|
| Early | <3 mo | S. aureus, Gram-negative bacilli |
| Delayed | 3-12/24 mo | Coagulase-negative staphylococci (CoNS), C. acnes |
| Late | >12/24 mo | CoNS (e.g., S. epidermidis), C. acnes |
⭐ Biofilm formation by bacteria like Staphylococcus epidermidis is a major challenge in prosthetic joint infections, often necessitating implant removal.
Specific Bone/Joint Infections - Unique Bone Invaders
- Tuberculous Spondylitis (Pott's Disease)
- Site: Thoracolumbar spine.
- Features: 'Cold abscess', psoas abscess, gibbus deformity.
- Paradoxical reaction. ATT: 9-12 months.
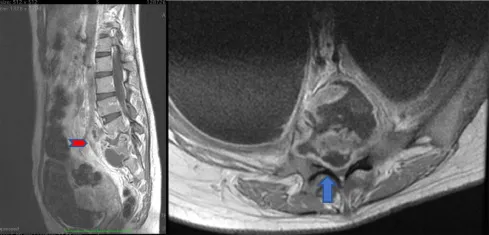
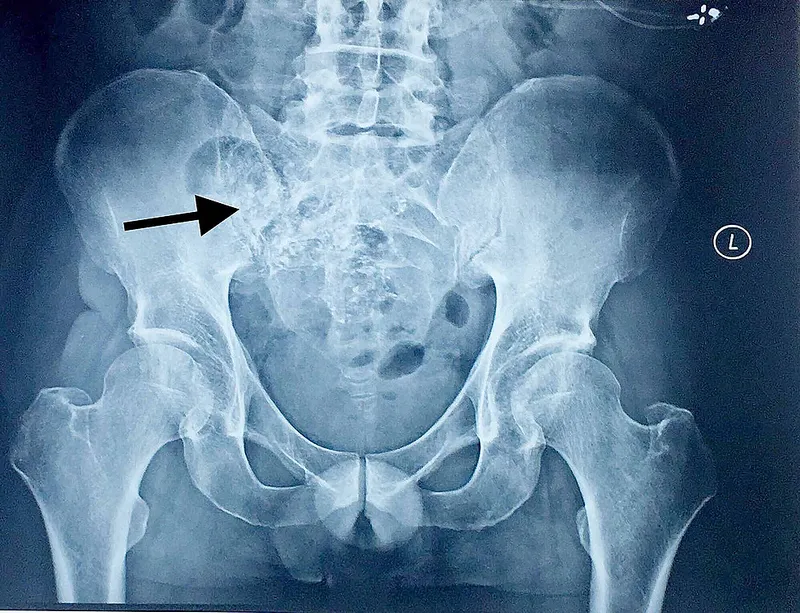
- Brucellar Spondylitis
- Key: Sacroiliitis.
- Signs: 'Pedro Pons' sign' (vertebral erosion), undulant fever.
- Fungal Osteomyelitis
- Agents: Candida, Aspergillus.
- Risks: Immunocompromised, IVDU, TPN.
⭐ > Pott's disease (tuberculous spondylitis) most commonly affects the lower thoracic and upper lumbar vertebrae, and can lead to characteristic 'cold abscesses' and kyphotic deformity (gibbus).
High‑Yield Points - ⚡ Biggest Takeaways
- Staphylococcus aureus is the most common cause of osteomyelitis and septic arthritis.
- In neonates, consider Group B Streptococcus and E. coli.
- Salmonella is characteristic in sickle cell disease patients with osteomyelitis.
- Pseudomonas aeruginosa is common in puncture wounds and IV drug users.
- Kingella kingae is a key pathogen for septic arthritis in children < 4 years.
- Mycobacterium tuberculosis can cause Pott's disease (vertebral osteomyelitis).
- Brucellosis often involves the sacroiliac joints and spine (spondylitis).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

