Intro & B-Cell Deficiencies - Antibody Alarms
- Types: Primary (congenital) vs. Secondary (acquired).
- Hallmark: Recurrent, severe, unusual infections.
Key B-Cell Deficiencies:
-
X-Linked Agammaglobulinemia (XLA/Bruton's)
- Defect: BTK gene → no B-cell maturation.
- Cells: ↓ B-cells (CD19+), ↓ all Ig. Normal T-cells.
- Infections: Encapsulated bacteria post-6 months (maternal IgG wanes).
- 📌 Boys, Bruton's, BTK, no B-cells, Bacterial.
⭐ XLA presentation typically after 6 months (maternal IgG protection).
-
Common Variable Immunodeficiency (CVID)
- Onset: Later. Normal B-cells, ↓ plasma cells, ↓ IgG, IgA.
- Infections: Sinopulmonary, Giardia. ↑ Autoimmune risk.
-
Selective IgA Deficiency
- Most common. Often asymptomatic.
- Labs: Serum IgA < 7 mg/dL. Normal IgG, IgM.
- Risks: Sinopulmonary/GI infections, anaphylaxis to IgA in blood products.

T-Cell & Combined Deficiencies - Cellular Commandos Down
-
DiGeorge Syndrome: Chromosomal 22q11.2 deletion. Thymic aplasia/hypoplasia → ↓ T-cells, parathyroid hypoplasia → hypocalcemia. 📌 CATCH-22: Cardiac defects, Abnormal facies, Thymic hypoplasia, Cleft palate, Hypocalcemia.
-
Severe Combined Immunodeficiency (SCID): Multiple genetic defects. Most common: X-linked (IL2RG gene). Also, Adenosine Deaminase (ADA) deficiency. Results in severe T-cell deficiency; B-cell & NK-cell numbers/function vary by type. Recurrent severe infections, failure to thrive.
⭐ SCID is a pediatric emergency; live vaccines are contraindicated.
- Wiskott-Aldrich Syndrome (WAS): X-linked recessive, WASP gene defect. 📌 TIE: Thrombocytopenia (small platelets), Infections (recurrent), Eczema. ↓ IgM, ↑ IgA, ↑ IgE.
- Ataxia-Telangiectasia (AT): Autosomal recessive, ATM gene defect (DNA repair). Triad: cerebellar Ataxia, oculocutaneous Telangiectasias, Immunodeficiency (esp. IgA deficiency). ↑ AFP. Increased risk of malignancy (lymphoma, leukemia).
Phagocyte & Complement Defects - Clean-up Crew Crisis
-
Phagocyte Defects:
- Chronic Granulomatous Disease (CGD):
- Defect: NADPH oxidase (↓ Reactive Oxygen Species, ROS). X-linked/AR.
- Infections: Catalase (+) organisms (📌 PLACēS: Pseudomonas, Listeria, Aspergillus, Candida, E.coli, S.aureus, Serratia). Granulomas.
- Dx: Nitroblue tetrazolium (NBT) test (negative), Dihydrorhodamine (DHR) flow cytometry (↓ oxidative burst).
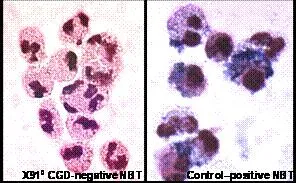
- Leukocyte Adhesion Deficiency (LAD-1):
- Defect: CD18 (integrin $\beta$2 subunit).
- Features: Recurrent bacterial infections, impaired wound healing, neutrophilia.
- ⭐ > Delayed umbilical cord separation (>30 days) is a hallmark of LAD-1.
- Dx: Flow cytometry (↓CD18).
- Chediak-Higashi Syndrome (CHS):
- Defect: LYST gene (lysosomal trafficking regulator). AR.
- Features: Pyogenic infections, partial albinism, neuropathy, giant granules in neutrophils.
- Dx: Peripheral smear (giant granules).
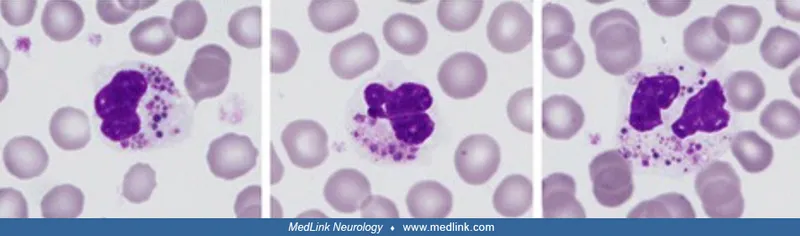
- Chronic Granulomatous Disease (CGD):
-
Complement Defects:
- C3 Deficiency:
- Impact: Impaired opsonization & MAC formation.
- Infections: Encapsulated bacteria (e.g., S. pneumoniae, H. influenzae).
- C5-C9 Deficiency (MAC Complex):
- Impact: Inability to form Membrane Attack Complex.
- Infections: Recurrent Neisseria spp. (meningitis, gonococcal).
- Dx (General): CH50 assay (↓ total complement activity), specific component assays.
- C3 Deficiency:
Dx & Tx Highlights - Immuno-Fixit Fast Facts
- Initial Screening Tests:
- Complete Blood Count (CBC) with differential (lymphopenia, neutropenia)
- Quantitative Immunoglobulin levels (IgG, IgA, IgM)
- CH50 assay (total classical complement activity)
- Confirmatory Diagnostic Tests:
- Lymphocyte subset enumeration by flow cytometry (T, B, NK cells; CD markers)
- Functional B & T cell proliferation assays
- Dihydrorhodamine (DHR) / Nitroblue Tetrazolium (NBT) test (for Chronic Granulomatous Disease - CGD)
- Specific genetic testing
- General Management Principles:
- Prophylactic antibiotics (e.g., TMP-SMX for Pneumocystis jirovecii pneumonia - PCP)
- Immunoglobulin (IVIG/SCIG) replacement therapy
- Hematopoietic Stem Cell Transplantation (HSCT) - often curative
- Gene therapy (emerging option for specific PIDs)
- Key Patient Precautions:
- ⚠️ Avoid ALL live attenuated vaccines (e.g., MMR, Varicella, Rotavirus, BCG, oral polio)
- ⚠️ Use irradiated, leukocyte-reduced, CMV-negative blood products if transfusion needed.
⭐ HSCT is curative for many severe PIDs like SCID and WAS.
High‑Yield Points - ⚡ Biggest Takeaways
- X-linked Agammaglobulinemia (Bruton's): Defect in BTK gene, results in no B cells; recurrent bacterial infections after 6 months of age.
- Common Variable Immunodeficiency (CVID): Most common symptomatic primary immunodeficiency (PID), characterized by low IgG, IgA, IgM; typically adult onset.
- IgA Deficiency: Most common PID overall, often asymptomatic; potential for anaphylaxis to IgA-containing blood products.
- DiGeorge Syndrome (22q11.2 deletion): Features thymic hypoplasia (leading to T-cell deficiency), hypocalcemia, and cardiac defects (CATCH-22).
- Severe Combined Immunodeficiency (SCID): Key genetic defects include IL-2R gamma chain or ADA deficiency; results in absent T and B cell function.
- Wiskott-Aldrich Syndrome (WAS): X-linked recessive disorder presenting with Thrombocytopenia, Eczema, and Recurrent infections (WATER); often ↑ IgE, IgA.
- Ataxia-Telangiectasia: Defect in ATM gene; presents with cerebellar ataxia, oculocutaneous telangiectasias, immunodeficiency (often IgA/IgG), and ↑ AFP.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

