Biofilm Basics - Slimy City Slickers
- Definition: Microbial communities adherent to surfaces and/or each other, encased in a self-produced Extracellular Polymeric Substance (EPS) matrix.
- Formation (Simplified): Attachment → Microcolonies → Maturation (EPS production) → Dispersion.
- Key Characteristics:
- Surface adherence: Biotic (tissues) or abiotic (implants).
- EPS matrix: Structural scaffold, protection.
- Enhanced resistance: ↑ to antibiotics, disinfectants, host immunity.
- Communication: Quorum sensing coordinates group behavior.
- Examples: Dental plaque, catheter/implant infections, chronic wounds, cystic fibrosis lung infections.
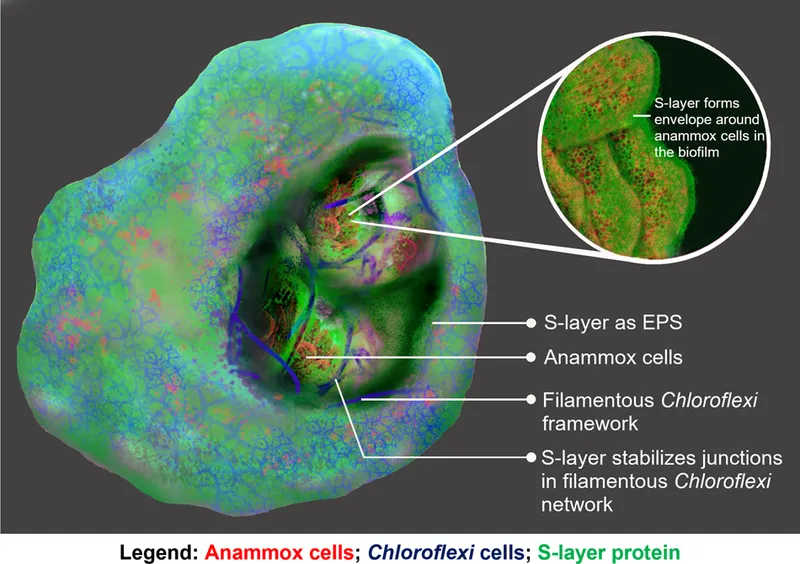
⭐ The Extracellular Polymeric Substance (EPS) matrix, composed mainly of polysaccharides, proteins, eDNA, and lipids, provides structural integrity and protection to the biofilm.
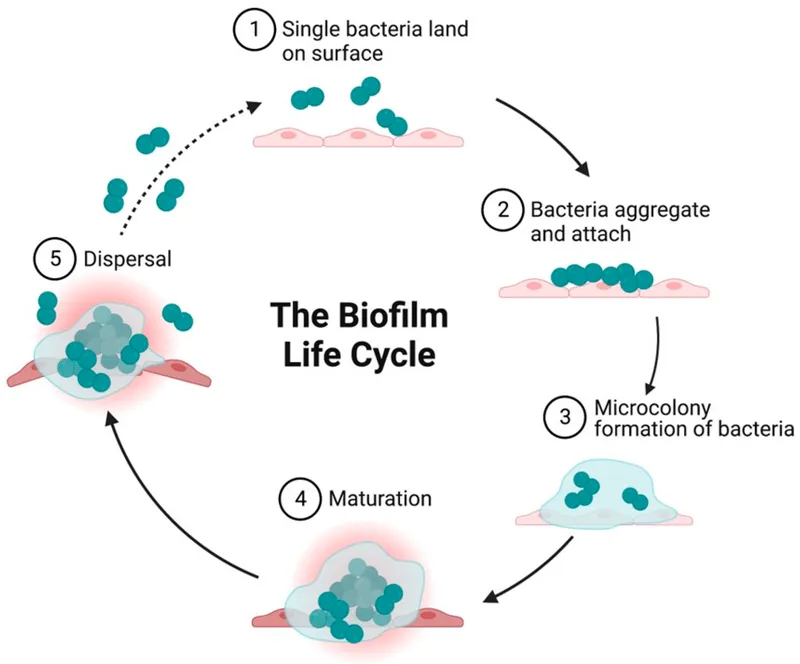
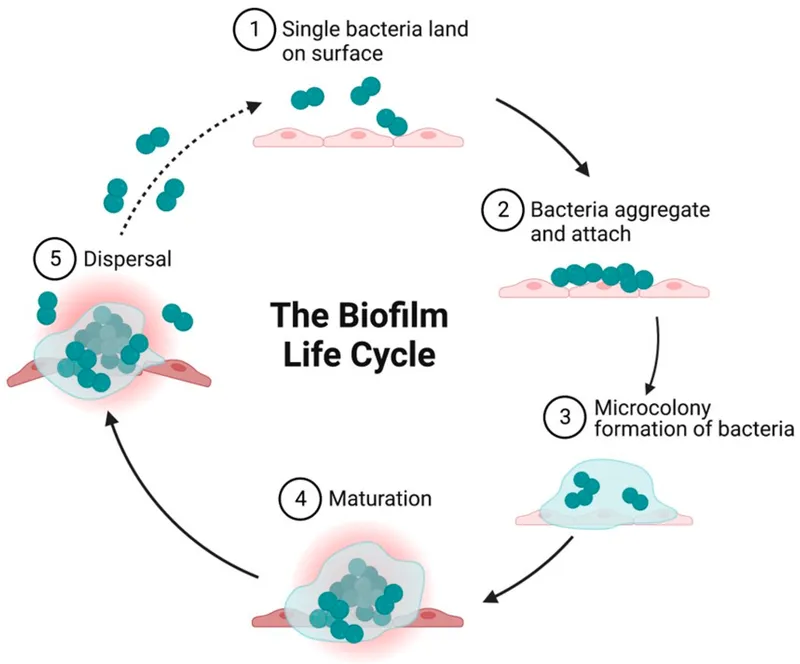
Biofilm Formation - Step-by-Step Slime
- 1. Reversible Attachment: Planktonic cells; transient surface adhesion (van der Waals).
- 2. Irreversible Attachment: Firm adhesion via adhesins (pili, fimbriae); motility lost.
⭐ Initial attachment of bacteria to a surface, often mediated by adhesins like pili and fimbriae, is a critical reversible then irreversible step in biofilm development.
- 3. Microcolony Formation: Cell proliferation & aggregation; Quorum Sensing (QS) starts.
- 4. EPS Matrix Production: Secretion of Extracellular Polymeric Substances (EPS) - "slime" (polysaccharides, proteins, eDNA); protection & structure.
- 5. Maturation: Complex 3D architecture, water channels; QS coordinates.
- 6. Dispersal: EPS degradation; planktonic bacteria released to colonize new sites.
Biofilms & Disease - The Resistance Stronghold
- Role in Chronic Infections: Key in persistent infections (e.g., cystic fibrosis pneumonia, periodontitis, chronic wounds, osteomyelitis).
- Device-Associated Infections (DAIs): Common on catheters, implants, prosthetic joints, contact lenses.
- 📌 Examples: Central Line Associated Bloodstream Infections (CLABSI), Catheter-Associated Urinary Tract Infections (CAUTI), Ventilator-Associated Pneumonia (VAP).
- Mechanisms of ↑ Antibiotic Resistance:
- EPS Matrix: Impedes antibiotic penetration; binds/inactivates drugs.
- Slow Growth Rate: Reduced metabolic activity makes cells less susceptible.
- Persister Cells: Dormant, highly tolerant subpopulation.
- Horizontal Gene Transfer (HGT): Facilitated exchange of resistance genes.
- Quorum Sensing (QS): Coordinates virulence & defense.
⭐ Biofilms exhibit significantly increased resistance to antibiotics, often 100-1000 times more than their planktonic counterparts, due to multiple factors including persister cells and impaired drug penetration.
- Clinical Challenges: Difficult to diagnose & eradicate; often require surgical removal of infected device/tissue; contribute to treatment failure & recurrence.
Quorum Sensing & Control - Biofilm Chatter & Combat
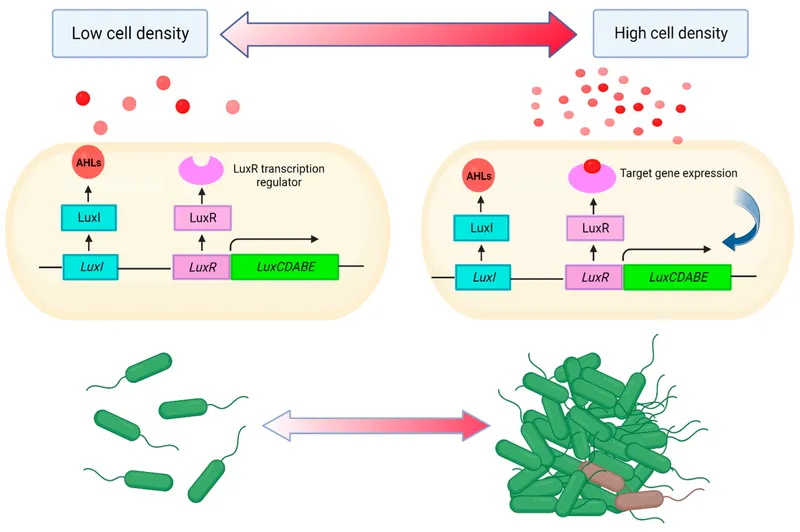
- Quorum Sensing (QS): Bacterial cell-to-cell communication; coordinates gene expression based on population density.
- Mediated by autoinducers (signaling molecules).
- Gram-negative: N-Acyl Homoserine Lactones (AHLs).
- Gram-positive: Autoinducing Peptides (AIPs).
- Regulates biofilm maturation, virulence, and dispersal.
- Mediated by autoinducers (signaling molecules).
⭐ Quorum sensing, using autoinducers like N-Acyl Homoserine Lactones (AHLs) in Gram-negative bacteria and autoinducing peptides (AIPs) in Gram-positive bacteria, regulates biofilm maturation and virulence factor expression.
- Biofilm Control Strategies:
- Quorum Quenching (QQ): Disrupting QS.
- Enzymes: AHL lactonases, acylases.
- QS inhibitors (QSIs).
- Matrix Disruption:
- Enzymes: DNases, alginate lyase, dispersin B.
- Chelators: EDTA (targets $Ca^{2+}$, $Mg^{2+}$).
- Antimicrobials often require higher doses or combination therapy.
- Quorum Quenching (QQ): Disrupting QS.
High‑Yield Points - ⚡ Biggest Takeaways
- Biofilms are structured microbial communities encased in a self-produced Extracellular Polymeric Substance (EPS) matrix.
- The EPS matrix protects against antimicrobials, host defenses, and environmental stress.
- Quorum Sensing (QS) is a key regulatory mechanism for biofilm formation, maturation, and dispersal.
- Biofilms are implicated in persistent and chronic infections, often on medical devices like catheters and implants.
- They exhibit significantly increased antimicrobial resistance compared to their planktonic counterparts.
- Common examples include Pseudomonas aeruginosa in cystic fibrosis lungs and dental plaque.
- Eradication is challenging, often requiring combination therapies or specific anti-biofilm agents.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

