Mediastinal Anatomy - Chest Central
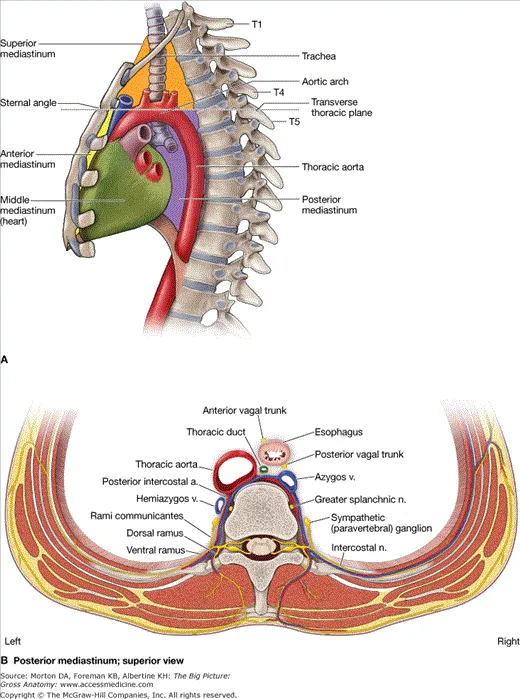
- Divided by transverse thoracic plane (sternal angle of Louis to T4-T5 IV disc).
- Superior Mediastinum: Above this plane.
- Contents: Thymus, great vessels (SVC, aortic arch & branches), trachea, esophagus, thoracic duct, phrenic & vagus nerves.
- Inferior Mediastinum: Below this plane; subdivided.
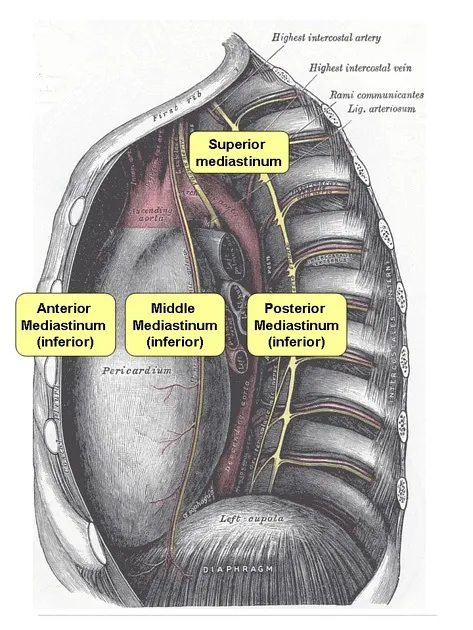
- Anterior: Sternum to pericardium. Contents: Thymus remnants, lymph nodes, fat.
- Middle: Contains pericardium & heart. Contents: Heart, great vessel roots (ascending aorta, pulm. trunk, SVC), phrenic nerves.
- Posterior: Pericardium to vertebrae (T5-T12). Contents: Esophagus, descending aorta, azygos/hemiazygos veins, thoracic duct.
- Superior Mediastinum: Above this plane.
⭐ The posterior mediastinum is the most common location for neurogenic tumors (e.g., schwannoma, neurofibroma).
Mediastinal Masses - Compartment Clues
Mediastinal masses are localized by compartment, aiding differential diagnosis.
- Anterior Mediastinum: (📌 "4 T's")
- Thymoma: Associated with Myasthenia Gravis.
- Teratoma/GCT (Germ Cell Tumors): Fat, fluid, calcification.
- Thyroid (goiter): Retrosternal extension.
- Terrible Lymphoma: Hodgkin's & Non-Hodgkin's.
- Middle Mediastinum:
- Lymphadenopathy: Sarcoidosis, TB, lymphoma, metastases.
- Cysts: Bronchogenic (most common), pericardial, esophageal duplication.
- Vascular: Aortic aneurysms, vessel anomalies.
- Posterior Mediastinum: (Neurogenic tumors are most common)
- Neurogenic tumors: Schwannoma, neurofibroma, ganglioneuroma.
- Esophageal lesions: Tumors, diverticula, achalasia.
- Paravertebral: Abscess, hematoma, EMH (Extramedullary Hematopoiesis).
⭐ 30-50% thymoma pts develop Myasthenia Gravis; 10-15% MG pts have thymoma.
Clinical Syndromes - Red Flag Roundup
- Compressive Symptoms:
- SVC Syndrome: Facial/arm swelling, plethora, JVD. (Common with Lung Ca, lymphoma).

- Airway (Trachea/Bronchi): Dyspnea, cough, stridor, post-obstructive pneumonia.
- Esophagus: Dysphagia.
- Nerves:
- Recurrent Laryngeal: Hoarseness.
- Phrenic: Diaphragmatic paralysis (elevated hemidiaphragm).
- Sympathetic Chain: Horner's Syndrome (ipsilateral ptosis, miosis, anhydrosis).
- SVC Syndrome: Facial/arm swelling, plethora, JVD. (Common with Lung Ca, lymphoma).
- Paraneoplastic Syndromes:
- Thymoma: Myasthenia Gravis (MG), pure red cell aplasia, hypogammaglobulinemia.
- Germ Cell Tumors: ↑AFP (non-seminomatous), ↑β-hCG (choriocarcinoma, some seminomas).
- Lymphoma: B-symptoms (fever, drenching night sweats, weight loss >10% in 6 months).
⭐ Myasthenia Gravis is the most common paraneoplastic syndrome associated with Thymoma, occurring in 30-50% of patients with thymoma.
Diagnostics & Key Disorders - Scan & Solve
-
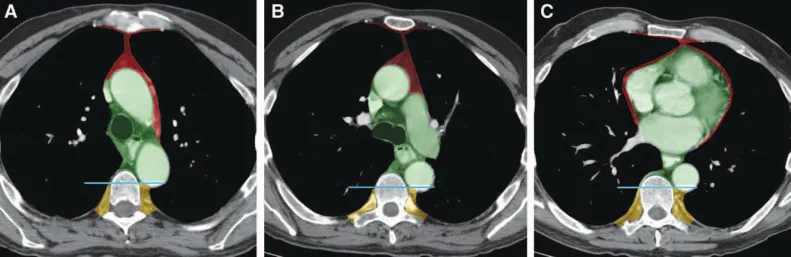
Imaging: CXR (initial), CT+C (gold standard), MRI (neuro/vascular), PET (malignancy).
-
Markers: AFP (NSGCT), β-hCG (GCT), LDH (Lymphoma).
-
Biopsy: EBUS-TBNA, CT-guided, Mediastinoscopy, VATS.
-
Key Disorders:
- Thymoma: Anterior; Myasthenia Gravis (30-50%).
- Lymphoma: Most common; Hodgkin/NHL.
- GCT: Anterior; Teratoma, Seminoma, NSGCT.
- Neurogenic: Posterior; Schwannoma.
- Mediastinitis: Acute (post-op/rupture), Chronic (fibrosing). 📌 Anterior: Thymoma, Teratoma, Thyroid, (Terrible) Lymphoma.
⭐ Lymphoma is the most common primary mediastinal tumor.
High‑Yield Points - ⚡ Biggest Takeaways
- Anterior mediastinum: Key masses are Thymoma, Teratoma/Germ cell tumors, Thyroid, and Lymphoma (the 4 T's).
- Thymoma is frequently linked to Myasthenia Gravis.
- Posterior mediastinum: Neurogenic tumors are most common here and overall.
- SVC syndrome: Caused by compression (e.g., lung cancer, lymphoma); presents with facial/arm swelling.
- Germ cell tumors can elevate AFP and/or β-hCG.
- Acute mediastinitis: Often due to esophageal perforation (Boerhaave's); a surgical emergency.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

