Chemotherapy Principles - Cell Cycle Killers
- Cell Cycle Specific (CCS) Agents: Exert cytotoxic effects during specific phases of the cell cycle. Most effective against high growth fraction tumors.
- G1 Phase (Presynthetic Growth):
- L-Asparaginase: Depletes asparagine.
- Corticosteroids: Lympholytic.
- S Phase (DNA Synthesis): 📌 Suspect AntiMetabolites, Hydroxyurea, Irinotecan, Topotecan.
- Antimetabolites: Methotrexate (MTX), 5-Fluorouracil (5-FU), Cytarabine (Ara-C).
- Hydroxyurea: Inhibits ribonucleotide reductase.
- Topoisomerase I inhibitors: Irinotecan, Topotecan.
- G2 Phase (Premitotic Growth & DNA Repair):
- Bleomycin: Causes DNA strand breaks.
- Etoposide, Teniposide: Inhibit Topoisomerase II.
- M Phase (Mitosis - Microtubule Targets):
- Vinca Alkaloids (e.g., Vincristine, Vinblastine): Inhibit microtubule polymerization.
- Taxanes (e.g., Paclitaxel, Docetaxel): Stabilize microtubules.
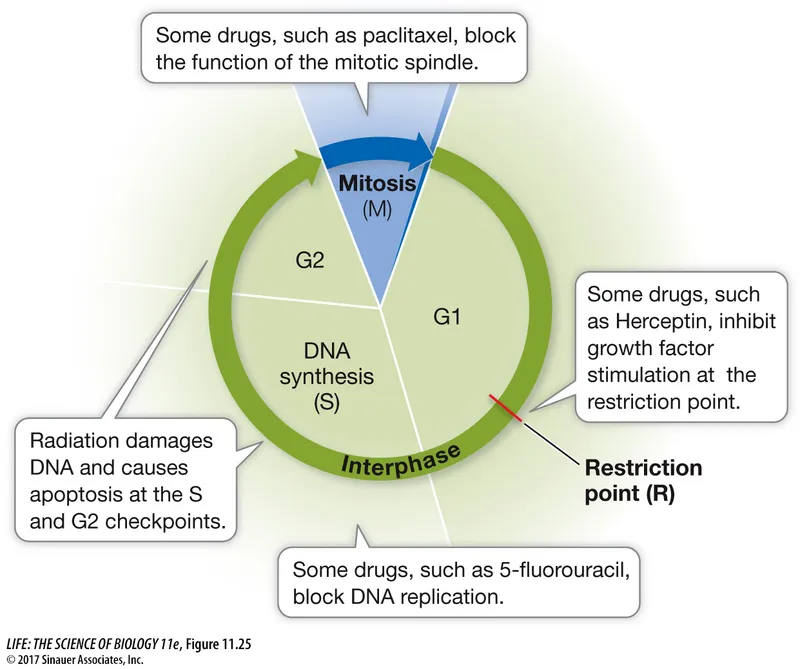
- G1 Phase (Presynthetic Growth):
⭐ Vincristine is known for its neurotoxicity (peripheral neuropathy) and is typically dose-capped, while Vinblastine is more myelosuppressive.
Chemo Toxicities & Resistance - Toxic Turmoil
- General Toxicities
- Myelosuppression: Nadir 7-14 days.
- Neutropenia (ANC < 1500/µL; Febrile if fever > 38.3°C + ANC < 500/µL)
- Anemia
- Thrombocytopenia
- Nausea/Vomiting (N/V): Ondansetron, Aprepitant.
- Mucositis, Alopecia, Fatigue.
- Myelosuppression: Nadir 7-14 days.
- Key Organ Toxicities
- Doxorubicin: Cardiotoxicity (max 450-550 mg/m²; Dexrazoxane).
- Trastuzumab: Cardiotoxicity.
- Bleomycin: Pulmonary fibrosis.
- Methotrexate (MTX): Pneumonitis, Nephrotoxicity (crystalluria; alkalinize urine), Mucositis.
- Cisplatin: Nephrotoxicity (ATN; Amifostine, hydration), Ototoxicity, Peripheral neuropathy.
- Vinca alkaloids: Peripheral neuropathy.
- Taxanes: Peripheral neuropathy.
- Cyclophosphamide/Ifosfamide: Hemorrhagic cystitis (Acrolein; MESNA).
- Chemoresistance
- Mechanisms: ↑Efflux (P-glycoprotein/MDR1), ↓Uptake, Drug inactivation, Target alteration (mutations), ↑DNA repair, Apoptosis evasion.
⭐ P-glycoprotein (MDR1 gene product) is a major mechanism of multi-drug resistance, actively pumping chemo drugs out of cancer cells.
oka
Immunotherapy Principles - Immune System Unleashed
- Core: Enhances body's immune system to fight cancer.
- Mechanisms:
- Immune Checkpoint Inhibitors (ICIs): Release T-cell "brakes".
- CTLA-4 inh. (Ipilimumab): Early T-cell priming (lymph node).
- PD-1 inh. (Nivolumab, Pembrolizumab): Act on T-cells in TME.
- PD-L1 inh. (Atezolizumab): Target ligand on tumor/immune cells (TME).
- Adoptive Cell Therapy (ACT):
- CAR T-cells: Engineered T-cells (Chimeric Antigen Receptors) target tumor antigens (e.g., CD19).
- Monoclonal Abs (mAbs): Target tumor antigens (Rituximab-CD20); opsonization, ADCC.
- Immune Checkpoint Inhibitors (ICIs): Release T-cell "brakes".
- Immune-Related Adverse Events (irAEs):
- Overactive immunity: Dermatitis, colitis, hepatitis, pneumonitis, endocrinopathies (hypophysitis, thyroiditis).
- Manage: Corticosteroids, therapy interruption/discontinuation.
⭐ > Ipilimumab (anti-CTLA-4) was the first ICI to show survival benefit in metastatic melanoma.

Targeted Therapy Principles - Precision Strikes
- Precision medicine: Exploits specific molecular alterations in cancer cells.
- Requires biomarker identification (e.g., EGFR, HER2, BRAF, ALK, PD-L1).
- Often cytostatic; side effects target-dependent (e.g., EGFR inhibitor rash).
- Key types:
- Monoclonal Antibodies (mAbs): "-mab" suffix.
- Target extracellular/surface molecules (e.g., Trastuzumab for HER2).
- Mechanisms: ADCC, CDC, direct signaling block, payload delivery (ADCs).
- Small Molecule Inhibitors (SMIs/TKIs): "-nib" suffix.
- Target intracellular kinases/pathways (e.g., Imatinib for BCR-ABL).
- Monoclonal Antibodies (mAbs): "-mab" suffix.
- Resistance can develop via target mutation or pathway bypass.
⭐ Trastuzumab (Herceptin) targets HER2 receptor; essential for HER2-positive breast cancer and gastric cancer treatment regimens where HER2 is overexpressed/amplified.
High‑Yield Points - ⚡ Biggest Takeaways
- CCS drugs target specific cell cycle phases; CCNS drugs act phase-independently.
- Nadir (lowest blood counts) typically 7-14 days post-chemo; risk of infection.
- Tumor Lysis Syndrome (TLS): ↑K⁺, ↑PO₄³⁻, ↑Uric acid, ↓Ca²⁺. Manage with hydration, Allopurinol/Rasburicase.
- Checkpoint Inhibitors (PD-1, CTLA-4) cause immune-related Adverse Events (irAEs).
- Targeted Therapy: MAbs (Rituximab-CD20, Trastuzumab-HER2) & TKIs (Imatinib-BCR-ABL).
- Febrile Neutropenia (ANC < 500/µL + fever): oncologic emergency, immediate antibiotics.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

