Systemic Diseases & Kidneys - Renal Rumble
- Systemic diseases frequently target kidneys, causing varied renal damage.
- Key injury patterns:
- Glomerular: Immune complex deposition (e.g., lupus nephritis), podocytopathies, amyloidosis.
- Tubulointerstitial: Acute Tubular Necrosis (ATN) from toxins/ischemia, drug-induced nephritis, infiltrative diseases (sarcoidosis).
- Vascular: Hypertensive nephrosclerosis, renal artery stenosis, vasculitis (e.g., ANCA), thrombotic microangiopathies (TMA).
- Common pathogenic pathways:
- Hemodynamic changes (e.g., ↓ renal perfusion in sepsis/heart failure).
- Direct cellular injury (e.g., myeloma light chains).
- Immune complex formation & deposition.
⭐ Diabetes Mellitus is the leading cause of End-Stage Renal Disease (ESRD) worldwide.
Diabetic Nephropathy - Sugar-Coated Kidneys
- Leading cause of CKD & ESRD; progressive damage from chronic hyperglycemia.
- Pathogenesis: Glomerular hyperfiltration, GBM thickening, mesangial expansion.
- Histo: Kimmelstiel-Wilson (KW) nodules (nodular glomerulosclerosis) pathognomonic. Diffuse form commoner.
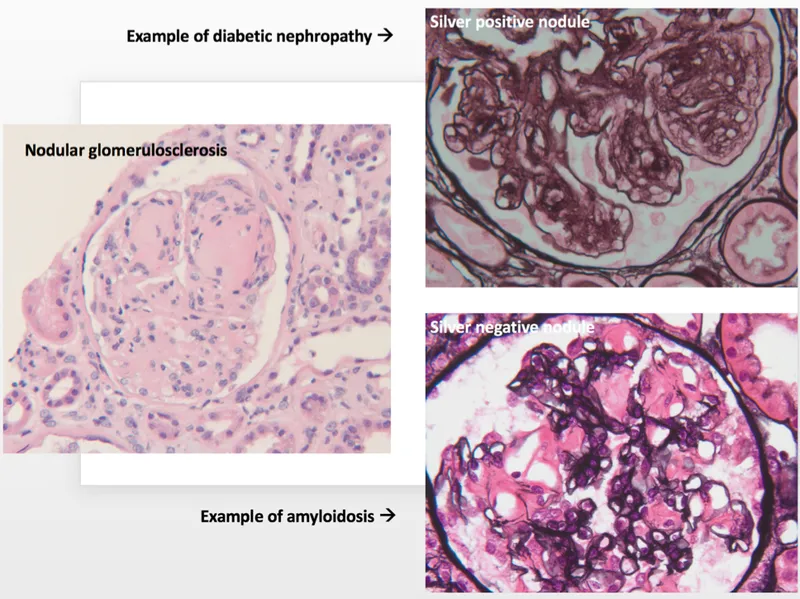
- Screening: Annual urine Albumin-to-Creatinine Ratio (AER).
- T2DM: At diagnosis.
- T1DM: 5 yrs post-diagnosis.
⭐ Earliest detectable clinical sign: Persistent microalbuminuria (AER 30-300 mg/g).
DN Stages (KDIGO Albuminuria Categories)
| Category | AER (mg/g or mg/24h) | Description |
|---|---|---|
| A1 | <30 | Normal to mild ↑ |
| A2 | 30-300 | Microalbuminuria |
| A3 | >300 | Macroalbuminuria / Overt Nephropathy |
Management:
- Glycemic control (HbA1c <7%).
- BP control: <130/80 mmHg.
- RAAS blockade (ACEi/ARB): If albuminuria.
- SGLT2 inhibitors: Renoprotective.
- Statins.
Lupus Nephritis - Lupus's Kidney PUNCH
- Immune complex glomerulonephritis in SLE; anti-dsDNA antibodies.
- "Full house" immunofluorescence: IgG, IgA, IgM, C3, C1q.
- Clinical: Proteinuria, hematuria, HTN, ↓ GFR.
- Treatment: Varies by class; immunosuppression (steroids, MMF, cyclophosphamide).
ISN/RPS Classification (2003/2018)
| Class | Name | Key LM Finding |
|---|---|---|
| I | Minimal Mesangial | Normal glomeruli |
| II | Mesangial Proliferative | Mesangial hypercellularity |
| III | Focal LN | Focal proliferation (<50% glom) |
| IV | Diffuse LN | Diffuse proliferation (≥50% glom) |
| V | Membranous LN | GBM thickening, 'spikes' |
| VI | Advanced Sclerosing | Global sclerosis (≥90% glom) |
⭐ Class IV (Diffuse Proliferative) Lupus Nephritis is the most common and severe form, often presenting with nephrotic syndrome and rapidly progressive glomerulonephritis.
Renal Vasculitis - Vessel Villainy
- ANCA-associated vasculitides (AAV) cause pauci-immune GN, often RPGN.
- Symptoms: Hematuria, proteinuria, rapid ↓ renal function.
- Urgent diagnosis & immunosuppression vital.
AAV Comparison: GPA vs MPA vs EGPA
| Feature | GPA (Wegener's) | MPA | EGPA (Churg-Strauss) |
|---|---|---|---|
| ANCA | c-ANCA/PR3 (~80-90%) | p-ANCA/MPO (~60-70%) | p-ANCA/MPO (~40-50%), Eosinophilia |
| Renal Biopsy | Pauci-immune crescentic GN, granulomas | Pauci-immune crescentic GN | Pauci-immune crescentic GN, eosinophilic infiltrates |
| Key Extra-renal | URT, LRT, sinusitis | LRT, skin, neuropathy | Asthma, neuropathy, eosinophilia |
Diagnostic Approach for RPGN (Focus on AAV)
⭐ Exam Favourite: ANCA type correlates with disease & prognosis:
- c-ANCA/PR3: GPA, higher relapse rates.
- p-ANCA/MPO: MPA & EGPA, often linked to more severe renal involvement initially.
High‑Yield Points - ⚡ Biggest Takeaways
- Lupus Nephritis Class IV (diffuse proliferative) is most common; renal biopsy is crucial for staging.
- Diabetic Nephropathy: Microalbuminuria is the earliest detectable abnormality; Kimmelstiel-Wilson nodules are specific.
- ANCA-associated vasculitis (GPA, MPA) typically causes pauci-immune crescentic glomerulonephritis.
- Goodpasture's Syndrome: Anti-GBM antibodies lead to linear IgG deposition; presents as pulmonary-renal syndrome.
- Myeloma Kidney: Due to light chain cast nephropathy; characterized by Bence Jones proteinuria.
- Scleroderma Renal Crisis: Presents with abrupt severe hypertension and acute kidney injury; ACE inhibitors are vital.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

