Raised ICP & Herniation - Skull's Squeeze
- Normal ICP < 15 mmHg; Pathological > 20-25 mmHg.
- Monro-Kellie Doctrine: Brain (80%), Blood (10%), CSF (10%) in fixed skull.
- $CPP = MAP - ICP$; Target 60-70 mmHg. Low CPP → ischemia.
- Signs: Headache, vomiting, ↓LOC, papilledema.
- 📌 Cushing's Triad (late): Hypertension, Bradycardia, Irregular respirations.
- Herniation Syndromes:
- Subfalcine: Cingulate gyrus under falx.
- Uncal (Transtentorial): Medial temporal lobe → tentorial hiatus.
⭐ Uncal: Ipsilateral CN III palsy (fixed dilated pupil), contralateral hemiparesis (Kernohan's notch phenomenon: ipsilateral).
- Central (Transtentorial): Diencephalon, midbrain downward.
- Tonsillar (Foraminal): Cerebellar tonsils → foramen magnum.
- Management: Stepwise approach.


Status Epilepticus - Brain on Fire
- Definition: Seizure >5 min OR ≥2 seizures, no full recovery between.
- Goal: Rapid termination to prevent neuronal injury.
- Types: Convulsive (GCSE), Non-Convulsive (NCSE).
- cEEG for Refractory SE (RSE) & suspected NCSE.
⭐ NCSE: suspect in unexplained Altered Mental Status (AMS) in ICU.
Acute Stroke in ICU - Clot & Bleed Chaos
📌 FAST (Face, Arms, Speech, Time) for rapid recognition. ICU: Stabilize (ABC), prevent secondary injury (edema, ↑ICP, seizures), manage complications.
| Feature | Ischemic Stroke (Clot) | Hemorrhagic Stroke (Bleed) |
|---|---|---|
| Primary Goal | Restore blood flow (reperfusion), neuroprotection | Limit hematoma growth, control Intracranial Pressure (ICP) |
| BP Target | Permissive HTN (<220/120 mmHg); <180/105 mmHg post-tPA | Aggressive ↓BP (SBP <140-160 mmHg for ICH) |
| Key Rx | IV Alteplase (<4.5h), Mech. Thrombectomy (<24h), Aspirin 160-325mg | Reverse anticoagulants (PCC, Vit K), Osmotic therapy, EVD, Nimodipine (SAH) |
| ICU Focus | NIHSS, edema, hemorrhagic transformation risk | GCS, ICP/CPP monitoring, seizure prophylaxis, vasospasm (SAH) |
⭐ Hemorrhagic transformation is a feared complication of thrombolysis for ischemic stroke, occurring in ~6% of patients receiving IV alteplase for acute ischemic stroke an can lead to significant worsening of neurological outcome or death.
Coma & Delirium - Mind Adrift
Coma: Unarousable. GCS < 8 → Intubate.
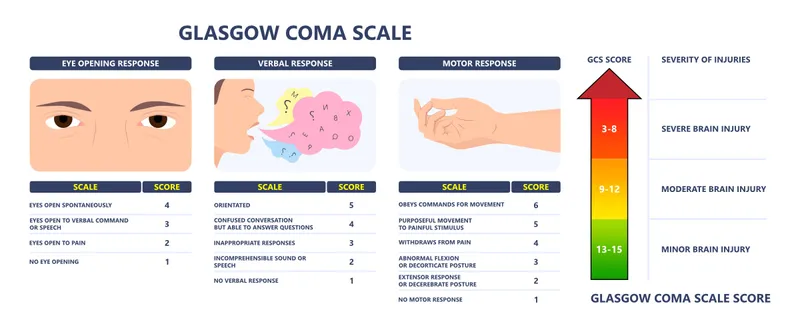
- Glasgow Coma Scale (GCS):
Comp. Response Score Eye Spont/Speech/Pain/None 4/3/2/1 Verbal Orient/Conf/Inappr/Sound/None 5/4/3/2/1 Motor Obeys/Local/Withdraw/Flex/Ext/None 6/5/4/3/2/1 Total: 3-15
-
Approach to Coma:
-
Causes (Coma): 📌 AEIOU-TIPS (Alcohol, Epilepsy, Infection, Overdose, Uremia, Trauma, Insulin, Psych, Stroke).
Delirium: Acute, fluctuating attention/awareness.
- Screen: CAM-ICU.
- Causes (Delirium): 📌 I WATCH DEATH (Infection, Withdrawal, Acute metabolic, Trauma, CNS, Hypoxia, Deficiencies, Endocrine, Acute vascular, Toxins, Heavy metals).
- Manage: Treat cause, non-pharma, cautious haloperidol.
⭐ The Confusion Assessment Method for the ICU (CAM-ICU) is a validated tool for delirium screening.
High‑Yield Points - ⚡ Biggest Takeaways
- GCS < 8 often requires intubation; crucial for neurological assessment.
- Cushing's triad (hypertension, bradycardia, irregular respirations) signals ↑ ICP.
- Manage ↑ ICP: head up (30°), mannitol/hypertonic saline, controlled hyperventilation.
- Status epilepticus (>5 min): IV lorazepam first, then phenytoin/fosphenytoin.
- Meningitis/Encephalitis: Early LP (if safe) & empiric antimicrobials are critical.
- Acute ischemic stroke: Thrombolysis/thrombectomy if eligible and within window.
- Brain death: Confirmed by coma, absent brainstem reflexes, and positive apnea test.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

