Viability & Live Birth Signs - Tiny Life Clues
-
Viability: Infant capable of independent existence post-birth.
- Legally: The legal definition of viability in India is not strictly defined by specific gestational age, weight, or length cut-offs. Instead, it is generally understood in medical and legal contexts as the point at which a fetus is capable of surviving outside the uterus, which is typically considered to be around 24 weeks of gestation, though this can vary based on medical advancements and individual circumstances.
- Modern Age Estimation: New Ballard Score (neuromuscular and physical maturity assessment), radiological assessment, histological examination, and anthropometric measurements provide more accurate gestational age determination than historical methods.
-
Signs of Maturity (Term Infant ~40 weeks):
- External:
- Length ~50 cm, Weight ~2.5-3.5 kg.
- Nails reach fingertips.
- Testes in scrotum (males), labia majora cover minora (females).
- Radiological (Ossification Centers):
- Distal Femoral Epiphysis (DFE): ~36 weeks.
- Proximal Tibial Epiphysis (PTE): ~38 weeks.
- Cuboid: ~40 weeks.
- External:
-
Signs of Live Birth: Evidence of life (e.g., respiration) after complete expulsion.
- Key: Comprehensive examination approach under BNS framework.
- Modern Assessment Methods:
- Thorough macroscopic and microscopic organ examination.
- Food presence in stomach/intestines, healing evidence, absence of maternal blood in fetal circulation.
- Hydrostatic Test considered unreliable due to false positives/negatives.
- Lung Appearance:
- Live birth: Pink, spongy, crepitant, rounded edges.
- Stillbirth: Dark red/purple, firm, sharp edges.
- Microscopic: Expanded alveoli.
⭐ The presence of an ossification center in the cuboid bone is a strong indicator of fetal maturity at or near term (~40 weeks).
Autopsy & Cause of Death - Postmortem Puzzles
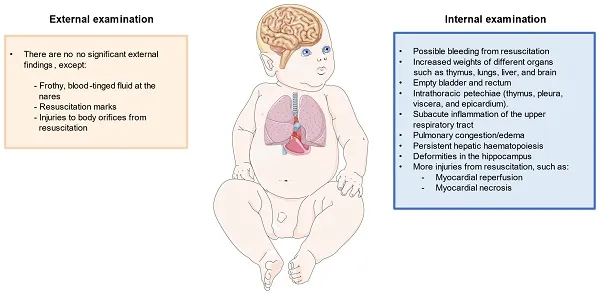
- Systematic Approach: Meticulous external & internal examination. Note injuries, signs of care/neglect.
- Key Organ Systems & Findings:
- Lungs: Crucial for live birth evidence & cause of death.
- Color: Pink (aerated) vs. dark red/purple (non-aerated).
- Consistency: Spongy & crepitant vs. firm & liver-like.
- Hydrostatic Test (Wade's/Breslau's): Considered unreliable in modern forensic practice.
- Stomach & Intestines: Presence/absence of milk, meconium, foreign material.
- Brain: Examine for hemorrhages (subdural, subarachnoid), contusions, fractures (e.g., pond fracture).
- Umbilical Cord: Signs of ligature, infection, or normal separation process.
- Lungs: Crucial for live birth evidence & cause of death.
- Common Causes of Death in Infanticide:
- Asphyxia: Smothering, throttling/strangulation, drowning, gagging.
- Head Injuries: Intentional impact, falls; skull fractures, intracranial bleeding.
- Neglect: Starvation, dehydration, abandonment leading to exposure/hypothermia.
- Stab Wounds/Other Sharp Force Trauma.
⭐ Modern forensic practice relies on comprehensive assessment including histological examination of lungs for definitive signs of respiration (distended alveoli, amniotic debris in airways), rather than the unreliable hydrostatic test. ICD-11 classification standards apply for international consistency in forensic reporting.
Special Tests & Evidence - Microscopic Missions
- Hydrostatic Test (Breslau's Second Life Test):
- Principle: Lung buoyancy in water indicates prior respiration.
- Unreliable as standalone method due to high false positive/negative rates.
- 📌 Mnemonic: "Float = Life" (but verify with other tests).
- Fallacies: False +ve (putrefaction, resuscitation); False -ve (feeble respiration, atelectasis, pneumonia, rapid death).
- Wredin's Test: Air in stomach/intestines also suggests live birth.
- Histopathology (Microscopic Examination):
- Lungs: Crucial component in multi-modal approach for live birth determination.
- Live birth: Expanded alveoli, flattened epithelium, capillaries engorged.
- Stillbirth: Unexpanded alveoli (atelectatic), cuboidal epithelium, thick septa.
- Other: Trauma (e.g., tentorial tears), infection, congenital anomalies.
- Ossification Centers: Distal femur (by 36 wks), talus, calcaneum (gestational age assessment).
- Lungs: Crucial component in multi-modal approach for live birth determination.
- Post-mortem Imaging (PMCT/PMMR):
- Modern standard: Detects lung aeration, GIT air, injuries non-invasively.
- Superior documentation and complementary to traditional methods.
- Diatom Test:
- Principle: Diatoms in deep tissues (bone marrow, brain, kidney) indicate ante-mortem drowning.
- Match diatoms with suspected water source. Crucial: meticulous technique to avoid contamination.
⭐ Modern forensic practice emphasizes integrated multi-modal approach combining histopathology, advanced imaging (PMCT/PMMR), and other autopsy findings for reliable live birth determination.
High‑Yield Points - ⚡ Biggest Takeaways
- Hydrostatic test is unreliable for live birth; modern practice uses comprehensive evaluation including histological lung examination.
- Ossification centers with advanced imaging (CT/MRI) and molecular methods provide precise infant age estimation.
- Viability varies by jurisdiction; modern threshold often 24 weeks with focus on sustained extrauterine life capacity.
- Identify cause of death: violent acts (commission) or fatal neglect (omission) under BNS provisions.
- Umbilical cord status (ligated/unligated) and signs of feeding indicate level of care.
- Maceration (skin slippage, reddish fluid) signifies intrauterine death (stillbirth).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

