Silicosis & CWP - Gritty Lung Grief
- Silicosis: Caused by inhaling crystalline silica ($SiO_2$) dust.
- Occupations: Mining, sandblasting, stone cutting, pottery.
- Pathology: Fibrotic silicotic nodules (macrophage response).
- Diagnosis: CT scan is superior for early detection and detailed assessment; X-ray findings include:
- Upper lobe predominant small, rounded opacities.
- "Eggshell calcification" of hilar lymph nodes (classic).
- Progressive Massive Fibrosis (PMF): opacities >1 cm (general guideline; criteria may vary).
⭐ Silicosis significantly increases risk of pulmonary tuberculosis (silicotuberculosis). No cure exists; lung scarring is irreversible.
- Complications: TB, PMF, lung cancer, COPD, cor pulmonale.
- Treatment: Symptom management, complication prevention, anti-fibrotic agents.
- Coal Worker's Pneumoconiosis (CWP): From coal dust inhalation.
- Simple CWP: Coal macules (pigmented macrophages); often asymptomatic.
- Complicated CWP (PMF): Large opacities >1 cm; progressive, severe impairment.
- Anthracosis: Asymptomatic carbon pigment in lungs/nodes.
- Caplan Syndrome: Pneumoconiosis (Silicosis/CWP) + Rheumatoid Arthritis + intrapulmonary nodules.
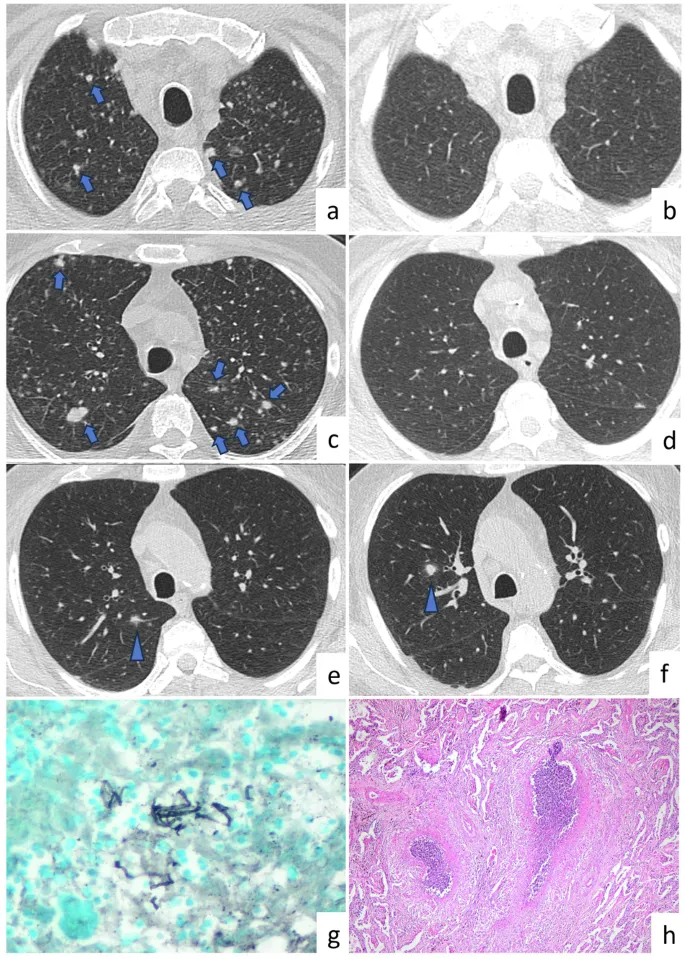
Asbestosis & Malignancies - Fibrous Fatalities
- Etiology: Inhalation of asbestos fibers. Amphiboles (crocidolite, amosite) more fibrogenic than serpentine (chrysotile).
- Pathology:
- Diffuse interstitial fibrosis, predominantly lower lobes.
- Asbestos bodies (ferruginous bodies): Golden-brown, beaded rods with iron-protein coat.
- Long latency: 15-20+ years for asbestosis.
- Manifestations: Progressive dyspnea, inspiratory crackles, clubbing.
- Pleural Involvement:
- Pleural plaques (parietal, diaphragmatic; often calcified) - hallmark of exposure.
- Benign asbestos pleural effusion.
- Malignancies:
- Bronchogenic carcinoma: Most common cancer. Risk synergistically ↑ with smoking.
- Malignant mesothelioma: Highly specific. Arises from pleura/peritoneum. Latency 25-40 years.
⭐ While mesothelioma is highly specific to asbestos exposure, bronchogenic carcinoma is the most common malignancy associated with asbestos.
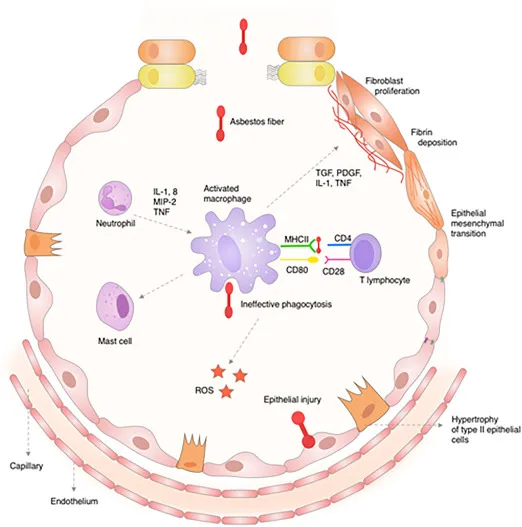
Organic Dusts & Hypersensitivity - Allergen Afflictions
- Hypersensitivity Pneumonitis (HP): Immune-mediated lung inflammation from organic dust inhalation; non-IgE.
- Common Types & Sources (📌 Mnemonic: Farmers BAG MAlt SHrooms & BIRds):
- Farmer's Lung: Moldy hay (Saccharopolyspora rectivirgula).
- Byssinosis: Cotton, flax, hemp dust (endotoxin).
⭐ Byssinosis, or 'Monday fever', is characterized by chest tightness and dyspnea that typically worsens on the first day of returning to work after a break.
- Bagassosis: Moldy sugarcane (Thermoactinomyces sacchari).
- Bird Fancier's Lung: Avian proteins.
- Malt Worker's Lung: Moldy barley (Aspergillus clavatus).
- Mushroom Worker's Lung: Thermophilic actinomycetes.
- Symptoms: Acute onset (4-8 hrs post-exposure) with fever, cough, dyspnea. Chronic exposure leads to fibrosis.
- Diagnosis: Exposure history, PFTs (restrictive), HRCT (ground-glass, nodules).
- Management: Antigen avoidance, corticosteroids.
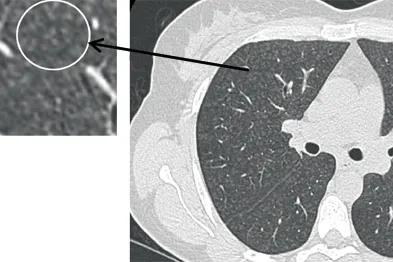
Occupational Asthma & Irritants - Chemical Chaos
- Occupational Asthma (OA): Airway hyperresponsiveness & inflammation due to workplace agents. Airway hyperresponsiveness is a cardinal feature of asthma, but its magnitude and presence can vary over time with disease activity, specific exposures, or treatment. It can be measured to confirm or exclude a diagnosis of asthma, classify the severity of asthma, or monitor asthma control.
- Sensitizer-induced OA: Latency period present. Immune-mediated (IgE or non-IgE).
- High Molecular Weight (HMW) agents: Flour, animal dander, enzymes.
- Low Molecular Weight (LMW) agents: Isocyanates, wood dust, anhydrides.
- Irritant-induced OA / Reactive Airways Dysfunction Syndrome (RADS): No latency. Develops after single, high-level exposure to irritant.
- Symptoms: Asthma-like, persistent for months.
- Causative agents: Chlorine, ammonia, smoke.
- Sensitizer-induced OA: Latency period present. Immune-mediated (IgE or non-IgE).
⭐ Isocyanates (e.g., in spray painting, foam manufacturing) are a leading cause of sensitizer-induced occupational asthma.
- Diagnosis: Detailed history, spirometry (pre/post-shift), peak expiratory flow monitoring, specific inhalation challenge (gold standard).
- Management: Removal from exposure, pharmacotherapy (ICS, bronchodilators).
High‑Yield Points - ⚡ Biggest Takeaways
- Silicosis: Sandblasting/mining; egg-shell calcification (hilar nodes), ↑ TB risk; upper lobes.
- CWP: Coal dust; Caplan syndrome (CWP + RA), Progressive Massive Fibrosis (PMF); upper lobes.
- Asbestosis: Shipbuilding/insulation; ferruginous bodies, pleural plaques; ↑ mesothelioma & bronchogenic ca; lower lobes.
- Byssinosis: Cotton/flax/hemp dust; "Monday fever" pattern; symptoms improve off work.
- Berylliosis: Aerospace/electronics; non-caseating granulomas (mimics sarcoidosis).
- Farmer's Lung: Hypersensitivity pneumonitis from moldy hay (actinomycetes).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

