Introduction: Chordoma vs Chondrosarcoma - Tale of Two Tumors
| Feature | Chordoma | Chondrosarcoma |
|---|---|---|
| Origin | Notochordal remnants | Cartilage (synchondroses) |
| Location | Midline: Clivus, Sacrum | Off-midline: Petroclival, Parasellar |
| Age Peak | Bimodal: 30s & 50-60 yrs | 30-40 yrs |
| Key Histo | Physaliphorous cells (bubbly) | Chondroid matrix, lobulated, +/- atypia |
| Behavior | Locally aggressive, destructive | Often slow-growing, locally invasive |
| Mnemonic 📌 | Clivus, Central, Notochord | Cartilage, Off-midline |
⭐ Chordomas are slow-growing malignant tumors from embryonic notochordal remnants, most common in clivus/sacrum, typically midline.
Clinical Presentation & Diagnosis: Skull Base Tumors - Unmasking the Culprits
- Clinical Presentation: Insidious onset; symptoms location-dependent.
- Cranial Nerve (CN) Palsies: Most frequent.
- Diplopia (CN VI), facial pain/numbness (CN V), hoarseness (CN IX, X). 📌 VI for VIsion double.
- Headache: Persistent, deep-seated.
- Nasal Symptoms: Obstruction, epistaxis (with anterior extension).
- Brainstem Signs (late): Ataxia, motor deficits.
- Cranial Nerve (CN) Palsies: Most frequent.
- Diagnosis:
- Neuroimaging:
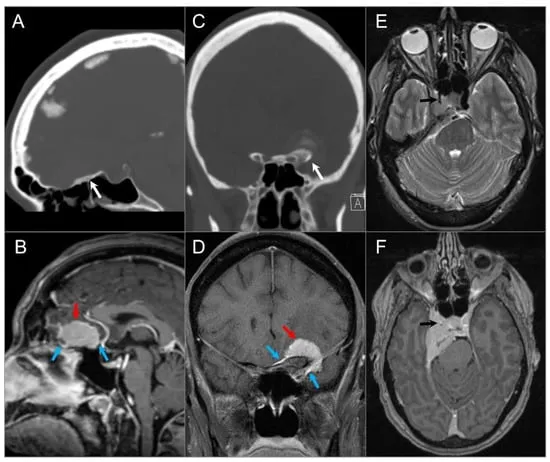
- MRI:
- Chordoma: Midline (clivus), destructive, T2 hyperintense, avid enhancement.
- Chondrosarcoma: Off-midline (petroclival), T2 hyperintense, "rings & arcs" calcification (CT better for Ca++).
- CT Scan: Details bony erosion, calcifications.
- MRI:
- Biopsy & Histopathology: Essential for confirmation.
- Chordoma: Physaliphorous cells (bubbly cytoplasm).
- Chondrosarcoma: Malignant chondrocytes in cartilaginous matrix.
- Neuroimaging:
⭐ MRI is the gold standard for diagnosis and delineating tumor extent, especially its relationship with neurovascular structures.
Histopathology & Molecular Markers: Tumor Signatures - Cellular Clues
| Feature | Chordoma | Chondrosarcoma |
|---|---|---|
| Key Cells | Physaliphorous cells (vacuolated, "soap-bubble" appearance) | Atypical chondrocytes in cartilage matrix |
| Stroma | Myxoid/chondromyxoid | Hyaline cartilaginous matrix |
| Growth Pattern | Lobulated | Lobular; graded (cellularity, atypia, mitoses) |
| IHC: Brachyury | Positive (nuclear) | Negative |
| IHC: Cytokeratin | Positive | Negative |
| IHC: S100 | Positive | Positive |
⭐ Brachyury (TBXT) nuclear staining is a highly specific and sensitive marker for chordoma, crucial for differentiating it from chondrosarcoma.
- Chordoma variants: Conventional, chondroid (S100+, CK+, Brachyury+), dedifferentiated.
- Chondrosarcoma grading (Evans): Grade I, II, III based on cellularity, atypia, mitotic activity.
Management & Prognosis: Skull Base Lesions - Battling the Base
- Goal: Maximal safe resection & adjuvant radiotherapy (RT).
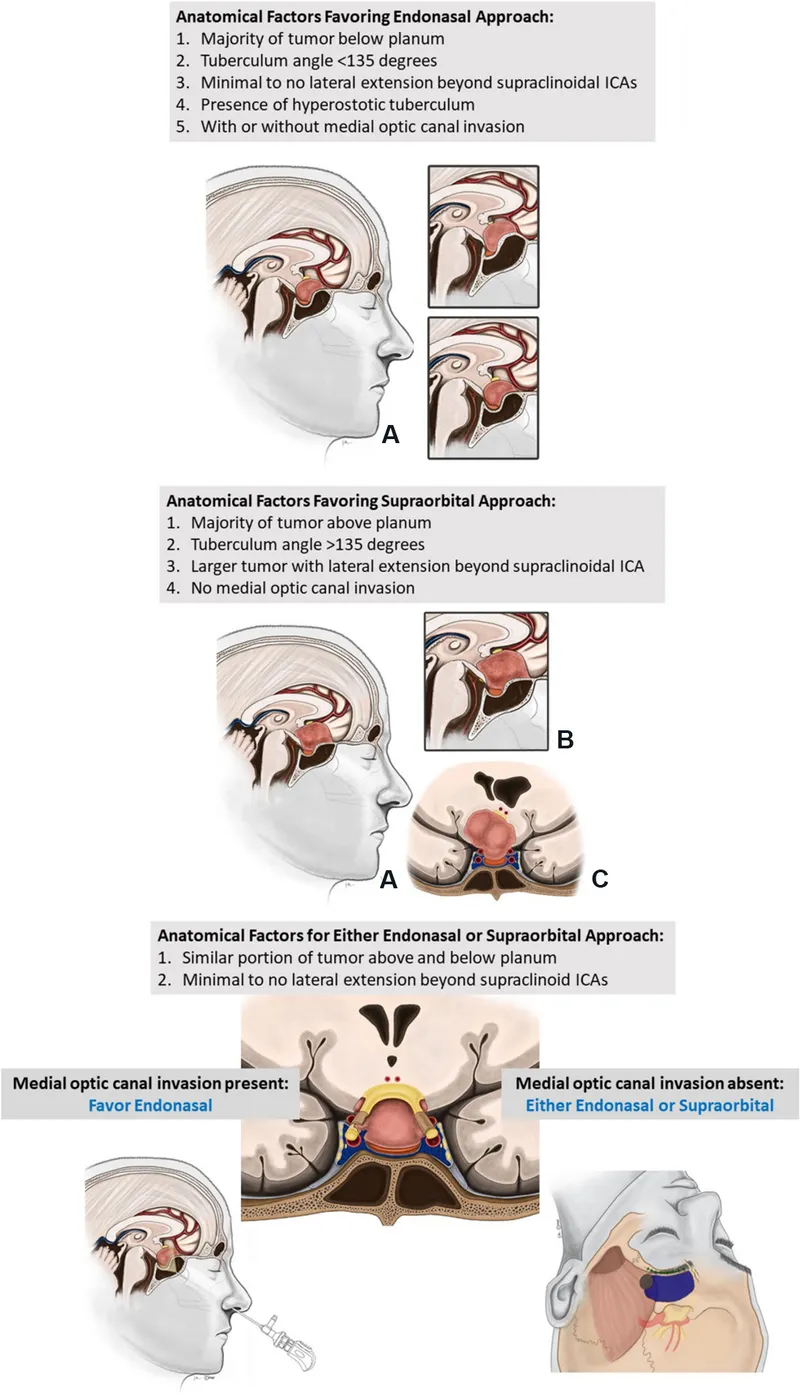
- Surgical Approaches:
- Endoscopic Endonasal Approach (EEA): Preferred for midline lesions (clivus, sella).
- Open craniotomy: For lateral/complex extensions.
- Endoscopic Endonasal Approach (EEA): Preferred for midline lesions (clivus, sella).
- Radiotherapy: Crucial for local control.
- Proton Beam Therapy (PBT): Preferred for chordomas due to Bragg peak precision, minimizing dose to surrounding critical structures. Dose: ~70-80 GyE.
- Photon RT (IMRT/Stereotactic): For chondrosarcomas or when PBT unavailable.
- Prognosis:
- Chordomas: Locally aggressive, high recurrence. 5-yr survival ~50-70%.
- Chondrosarcomas: More indolent, better prognosis. 5-yr survival ~80-90%.
- Negative factors: Large size, brainstem involvement, incomplete resection, RT delays.
⭐ For skull base chordomas, maximal safe surgical resection followed by high-dose adjuvant radiotherapy (preferably proton beam therapy) is the standard of care and offers the best local control.
📌 Chordoma = Clivus common, Challenging, Consider PBT. Chondrosarcoma = Cartilaginous, Comparatively better prognosis.
High‑Yield Points - ⚡ Biggest Takeaways
- Chordomas: Notochord remnants, midline (clivus). Chondrosarcomas: Cartilage origin, often off-midline (petroclival).
- Symptoms: Cranial nerve palsies (esp. VI nerve), headaches.
- Chordomas: Physaliphorous cells; midline destructive, T2 hyperintense on MRI.
- Chondrosarcomas: Malignant chondrocytes; may show chondroid matrix calcification (rings/arcs).
- Treatment: Maximal safe resection + adjuvant radiotherapy (proton beam for chordomas).
- Chondrosarcomas have better prognosis; Chordomas show high local recurrence.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more