Overview of Complications - Risky Business
Skull base surgery: complex, high-risk. Complications impact morbidity & mortality. Broadly:
- Intraoperative:
- Vascular injury (ICA, major sinuses) → major bleed.
- Cranial nerve (CN) damage → functional loss.
- Brain/brainstem injury.
- Postoperative:
- CSF Leak: 📌 Most common. Increases meningitis risk.
- Infection: Meningitis, wound, abscess.
- Neurological deficits: CN palsies, stroke, seizures.
- Pneumocephalus.
- Hemorrhage/Hematoma.
- Endocrine dysfunction (pituitary/suprasellar).
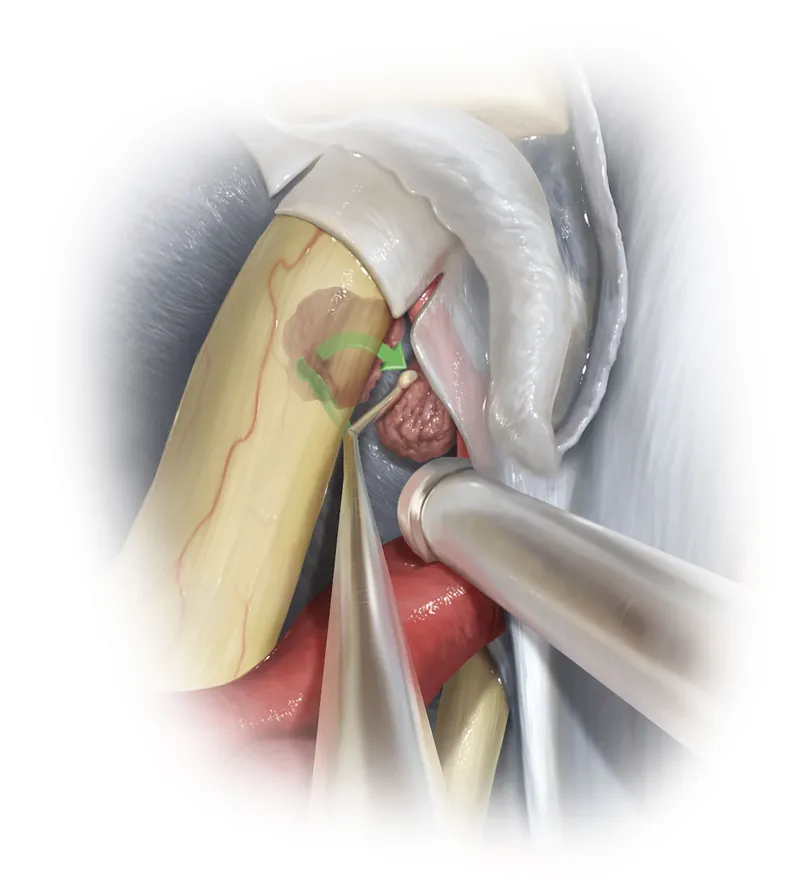
⭐ CSF leak, occurring in up to 5-20% of cases, is the most frequent complication, potentially leading to life-threatening meningitis.
CSF Leaks - The Unwanted Flow
- Most common complication post-skull base surgery. Dural/arachnoid breach allows CSF escape.
- Etiology: Iatrogenic (surgery), trauma, spontaneous (e.g., ↑ICP, congenital defects).
- Common Sites: Anterior fossa (cribriform, ethmoid, sphenoid), middle fossa (tegmen).
- Clinical Features:
- Clear, watery rhinorrhea/otorrhea (salty taste).
- Postural headache (worse upright).
- Halo/Ring sign on linen.
- Glucose test: CSF glucose typically >30 mg/dL or ~60% of serum glucose.
- Diagnosis:
- Clinical suspicion crucial.
- Imaging: High-resolution CT, CT cisternography, MRI (T2 CISS/FIESTA).
⭐ β2-Transferrin assay: Gold standard, highly specific for CSF.
- Management Approach:
- Complications: Meningitis (most feared, 10-25% risk if untreated), pneumocephalus, brain abscess. 📌 Mnemonic for meningitis risk: "LEAKY BRAIN = PAIN".
Neurological Deficits - Nerve Alarms
- Cranial Nerve (CN) palsies are significant risks; type depends on surgical approach.
- CN I (Olfactory): Anosmia, esp. anterior approaches (e.g., craniofacial resection).
- CN II (Optic): Visual loss, chiasmal injury (e.g., pituitary, parasellar surgery).
- CN III, IV, VI: Diplopia, ophthalmoplegia (e.g., cavernous sinus involvement).
- CN V (Trigeminal): Facial numbness, corneal reflex ↓, mastication weakness.
- CN VII (Facial): Palsy (most common motor CN injury), taste loss.
- CN VIII (Vestibulocochlear): Sensorineural hearing loss, vertigo.
- CN IX, X, XI, XII (Lower CNs): Dysphagia, hoarseness, aspiration, shoulder droop, tongue deviation.
- Intraoperative Neuromonitoring (IONM) essential as "nerve alarm".
- Techniques: EMG (for CN VII, X, XI, XII), BAEP/ABR (CN VIII), VEP (CN II), SSEP, MEP.
- ⚠️ Alarm: e.g., >50% drop in amplitude or 10% increase in latency.
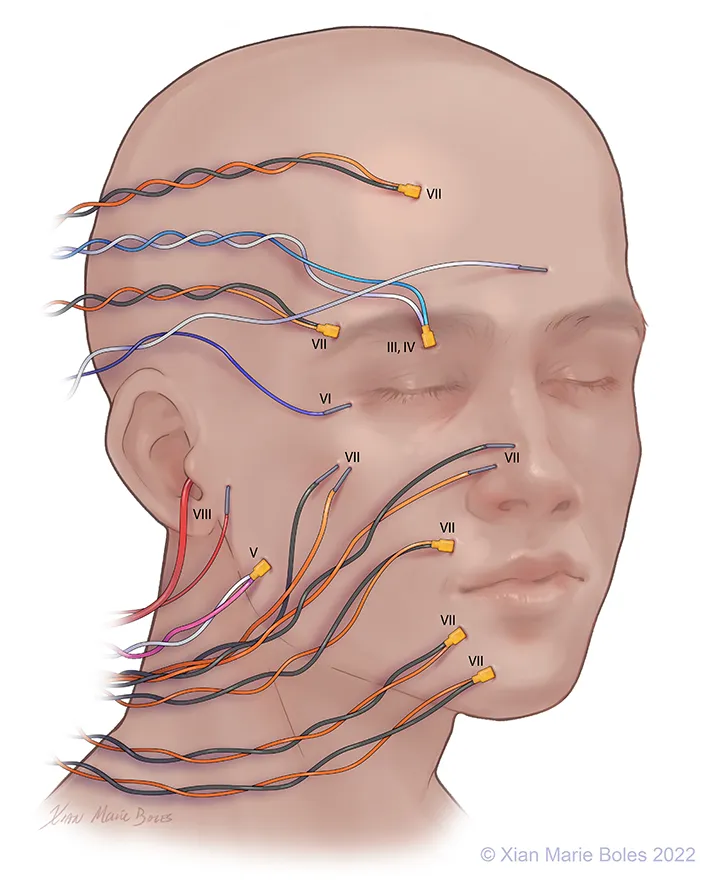
⭐ Facial nerve (CN VII) is the most frequently monitored (and injured) motor cranial nerve in lateral skull base surgery; preservation is a key surgical goal.
Vascular & Other Major Complications - Code Red Events
- ICA Injury: Catastrophic bleed, stroke risk. Manage: packing, endovascular repair (stent/coil), bypass.
- Venous Sinus Laceration: (e.g., Cavernous, Sigmoid) Massive hemorrhage, air embolism risk. Manage: packing, repair.
- Fulminant Meningitis/Ventriculitis: Rapid neurological decline, sepsis. Aggressive IV antibiotics, CSF diversion.
- Brain Abscess: Focal infection, mass effect. Surgical drainage, prolonged antibiotics.
- Tension Pneumocephalus: Acute neurological deterioration. Urgent decompression.
⭐ Pseudoaneurysm is a delayed but critical complication of ICA injury, often requiring endovascular treatment to prevent rupture and stroke.
Prevention & Management - Safety Nets
- Prevention:
- Meticulous surgical technique, detailed pre-op planning (imaging, neuronavigation).
- Judicious use of prophylactic antibiotics.
- Robust, watertight multilayered dural/skull base reconstruction.
- Management:
- Vigilant post-op monitoring for early complication recognition.
- Prompt, evidence-based intervention.
- Collaborative multidisciplinary team (MDT) approach.
- CSF leak: initial conservative (bed rest, lumbar drain); surgical repair for persistence.
⭐ Beta-2 transferrin is highly specific for identifying CSF leaks.
High‑Yield Points - ⚡ Biggest Takeaways
- CSF leak is the most frequent complication, predisposing to meningitis.
- Cranial nerve deficits, especially facial nerve (VII) and lower cranial nerves (IX-XII), are significant risks.
- Major vascular injury (e.g., internal carotid artery, venous sinuses) can be catastrophic.
- Pneumocephalus, seizures, and hydrocephalus are important neurological complications.
- Endocrine dysfunction is a key concern after pituitary or parasellar region surgeries.
- Postoperative infections like meningitis or wound site infections require vigilance.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

