Laryngomalacia - Floppy Larynx Fun
- Most common congenital laryngeal anomaly & cause of stridor.
- Pathophysiology: Immature, "floppy" supraglottic structures (arytenoids, epiglottis) collapse inward during inspiration.
- Features:
- Inspiratory stridor, onset by 4-6 weeks.
- Worse: Supine, crying, feeding. Better: Prone.
- Normal cry.
- Severe cases: FTT, GERD, apnea.
- Diagnosis: Flexible laryngoscopy (awake) shows dynamic collapse; classic "omega-shaped" epiglottis.

- Management:
- Most resolve spontaneously by 18-24 months (conservative).
- Severe: Supraglottoplasty.
⭐ Laryngomalacia is the most common cause of congenital stridor, typically presenting with inspiratory stridor that worsens in the supine position or during agitation.
Tracheo/Bronchomalacia - Weak Windpipe Woes
⭐ Tracheomalacia often presents with a characteristic expiratory barking cough and can be associated with tracheo-esophageal fistula.
- Pathophysiology: Excessive compliance & dynamic collapse of tracheal/bronchial walls during expiration.
- Etiology:
- Primary (Intrinsic): Congenital cartilage weakness.
- Secondary (Extrinsic): Compression (e.g., vascular ring), post-intubation, inflammation.
- Clinical Features:
- Expiratory stridor/wheeze, characteristic barking cough (worsens with crying, feeding, supine position).
- Recurrent respiratory infections; severe cases: cyanotic spells (“dying spells”).
- Symptoms may improve in prone position.
- Diagnosis:
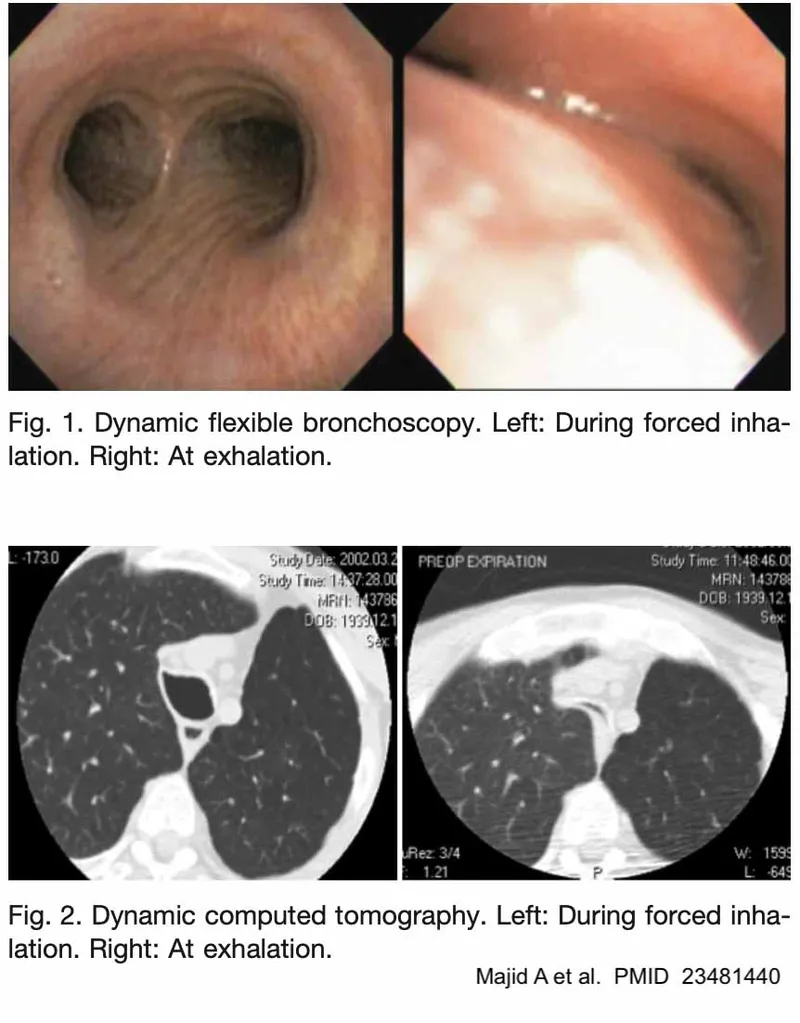
- Gold Standard: Flexible bronchoscopy (shows >50% luminal collapse during expiration).
- Fluoroscopy, CT/MRI (to identify extrinsic compression).
- Management:
- Conservative: Most resolve spontaneously by 1-2 years. Humidification, chest physiotherapy, GERD management.
- CPAP/BiPAP for moderate symptoms.
- Surgical (severe/refractory): Aortopexy, tracheopexy, tracheostomy.
Subglottic Stenosis & Webs - Narrow Escape Routes
Subglottic Stenosis (SGS): Airway narrowing below vocal cords.
- Types:
- Congenital: Developmental (cricoid anomaly).
- Acquired: Post-intubation (commonest), trauma, GERD.
- Symptoms: Biphasic stridor, barking cough, recurrent croup, dyspnea; worsens with URI.
- Diagnosis: Endoscopy (flex/rigid). X-ray (steeple sign, non-specific).
⭐ Congenital subglottic stenosis is often defined as a subglottic diameter <4mm in a full-term infant; Cotton-Myer grading is used for severity.
- Cotton-Myer Grading (% obstruction):
- Grade I: 0-50%
- Grade II: 51-70%
- Grade III: 71-99%
- Grade IV: No lumen
Subglottic Webs: Thin membrane in subglottis; rare.
- Symptoms: Symptoms like SGS; severity varies.
- Diagnosis: Endoscopy.
Management Approach:

- SGS Treatment: Observation, dilation, laser, cricoid split, LTR, CTR. Tracheostomy if severe.
- Web Treatment: Endoscopic division (cold knife/laser).
Vascular Rings & Slings - Artery Squeeze Play
- Anomalous vessels compress trachea/esophagus.
- Types & Features:
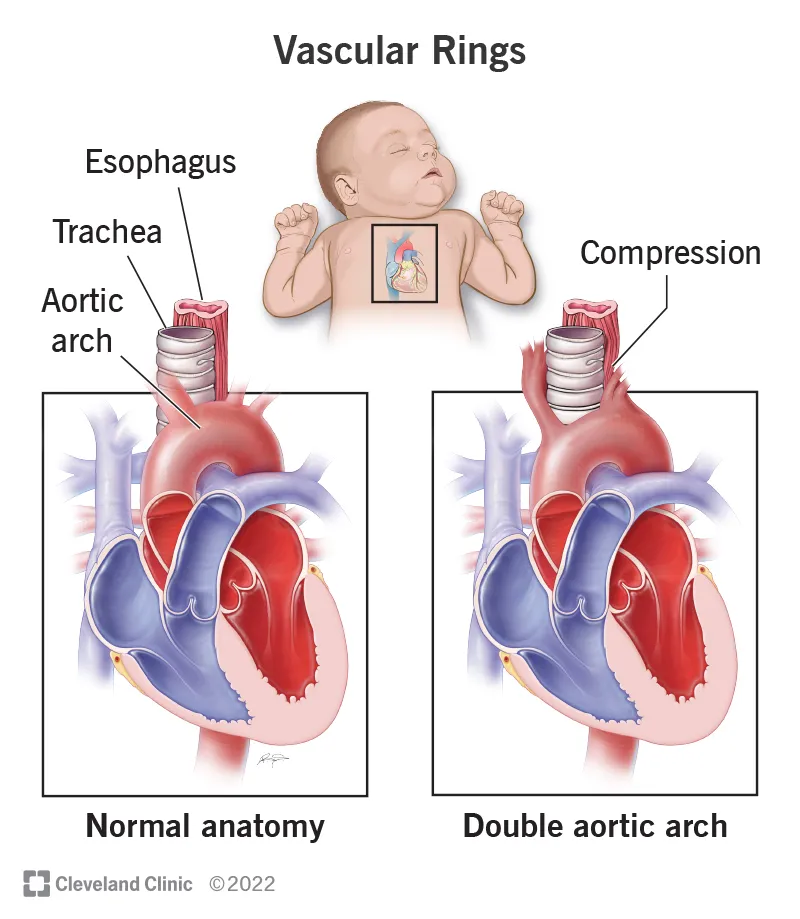
- Double Aortic Arch: Complete ring; tracheal & esophageal squeeze.
⭐ A double aortic arch is the most common symptomatic vascular ring, causing both tracheal and esophageal compression.
- Right Aortic Arch with Aberrant Left Subclavian Artery: Lig. arteriosum completes ring. Dysphagia lusoria.
- Pulmonary Artery Sling: L. PA from R. PA, between trachea & esophagus. Posterior tracheal squeeze. Assoc. tracheal stenosis (ring-sling complex).
- Innominate Artery Compression: Anterior tracheal squeeze by innominate artery.
- Double Aortic Arch: Complete ring; tracheal & esophageal squeeze.
- Symptoms:
- Respiratory: Stridor (biphasic, expiratory ↑), wheeze, cough, apnea.
- Esophageal: Dysphagia, feeding issues.
- Symptoms worsen with feeding, crying, neck flexion.
- Diagnosis:
- CXR, Barium swallow (indentations).
- CT Angiography / MRI: Gold standard.
- Bronchoscopy: Pulsatile compression, assess tracheomalacia.
- Management: Surgical division of ring/vessel reimplantation (PA sling).
High‑Yield Points - ⚡ Biggest Takeaways
- Laryngomalacia: Most common cause of stridor in infants; inspiratory stridor, often self-resolving.
- Subglottic Stenosis: Biphasic stridor; most common anomaly needing tracheostomy in young children.
- Vocal Cord Paralysis: Unilateral (weak cry, aspiration); Bilateral (severe stridor, airway compromise).
- Choanal Atresia: Bilateral is a neonatal emergency (cyanosis with feeding); CHARGE syndrome association.
- Tracheomalacia: Expiratory stridor/barking cough; dynamic collapse; associated with TEF.
- Laryngeal Webs: Stridor, weak cry/aphonia; incomplete recanalization; glottic most common.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

