TM Perforation: Anatomy & Intro - The Drum Breach
- Definition: A defect or hole in the tympanic membrane (TM), separating the external auditory canal from the middle ear.
- Anatomy of TM:
- Layers (3): Outer squamous epithelium, middle fibrous (radial & circular fibers), inner mucosal. 📌 Mnemonic: Elephants Find Mice (Epithelial, Fibrous, Mucosal).
- Parts: Pars Tensa (inferior, larger, taut, 3 layers, main vibratory part); Pars Flaccida (Shrapnell's membrane; superior, smaller, lax, 2 layers - lacks fibrous layer).
- Significance: Impairs sound conduction (hearing loss) & protection.

⭐ The absence of the middle fibrous layer in Pars Flaccida makes it more susceptible to retraction and the development of attic cholesteatoma.
TM Perforation: Etiology & Types - Why Drums Burst
- Etiology:
- Traumatic:
- Direct: Q-tip injury, foreign body, iatrogenic (e.g., syringing).
- Indirect: Barotrauma (slap, blast, diving), temporal bone fracture.
- Infective:
- Acute Suppurative Otitis Media (ASOM): Pus bursts through TM.
- Chronic Suppurative Otitis Media (CSOM): Persistent perforation.
- Traumatic:
- Types (Site):
- Central (Tubotympanic): Pars tensa; TM remnant all around. Generally safer.
- Marginal (Atticoantral): Involves annulus; cholesteatoma risk ↑.
- Attic (Atticoantral): Pars flaccida; cholesteatoma risk ↑.
⭐ Marginal & Attic perforations are considered unsafe/dangerous due to high cholesteatoma risk.
- Types (Size): Small (<25%), medium (25-50%), large (>50%), subtotal.
 oka
oka
TM Perforation: Clinical Features - Hole Telltales
- Symptoms:
- Hearing loss: Conductive, severity varies with size/location.
- Otorrhea: If infected; mucoid, purulent, or blood-tinged.
- Tinnitus: Whistling, especially with small perforations.
- Otalgia: Usually brief, with acute injury or infection.
- Signs (Otoscopy):
- Visible perforation: Central, marginal, or attic.
- Loss of landmarks: Cone of light, handle of malleus may be visible through hole.
- Middle ear mucosa: May be visible, normal or inflamed.
⭐ Rinne test negative (bone conduction > air conduction) in affected ear; Weber test lateralizes to affected ear (conductive hearing loss).
TM Perforation: Diagnosis - Spotting the Split
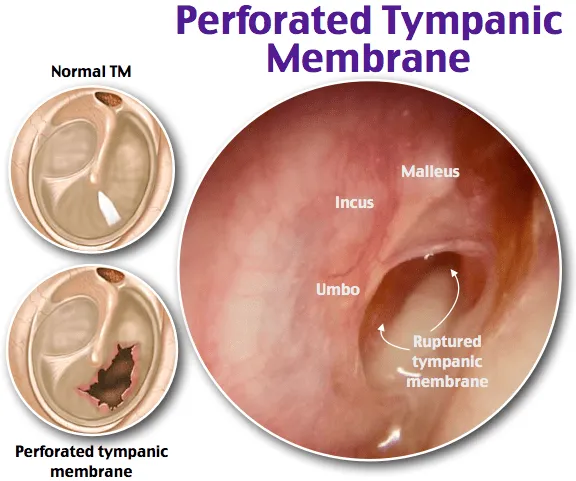
- Otoscopy:
- Direct visualization of perforation (site, size, shape).
- Margins: Acute (sharp edges), Chronic (rounded, epithelialized).
- Middle ear mucosa may be visible.
- Tuning Fork Tests (512 Hz):
- Rinne: Negative (BC > AC) in affected ear.
- Weber: Lateralizes to affected ear.
- Audiometry:
- Pure Tone Audiometry (PTA): Conductive Hearing Loss (CHL); degree varies with size/site.
- Tympanometry: Type B curve (large ear canal volume).
⭐ In PTA, an air-bone gap > 15-20 dB is significant for CHL in TM perforation contexts.
TM Perforation: Management & Complications - Mending & Mayhem

Management Strategy:
- Conservative:
- Keep ear dry (water precautions).
- Antibiotic ear drops if signs of infection (e.g., ciprofloxacin).
- Observation for spontaneous healing (common in traumatic perforations).
- Surgical (Myringoplasty):
- Indications: Perforation persisting > 3-6 months, recurrent otorrhea, significant hearing loss.
- Techniques: Underlay, Overlay (temporalis fascia commonest graft).
Potential Complications:
- Hearing Loss (Conductive/Mixed).
- Chronic Suppurative Otitis Media (CSOM) - persistent discharge.
- Cholesteatoma formation (especially marginal perforations).
- Tympanosclerosis.
- Recurrent infections.
⭐ Most traumatic TM perforations, especially small to moderate central ones, heal spontaneously within 6-8 weeks to 3 months. Water precautions are crucial during this period.
High‑Yield Points - ⚡ Biggest Takeaways
- Most common causes: Trauma (e.g., slap, Q-tip injury) and Acute Suppurative Otitis Media (ASOM).
- Most common site: Pars tensa, especially the anteroinferior quadrant.
- Key symptoms: Conductive hearing loss (CHL), tinnitus; otorrhea if infected.
- "Safe" vs. "Unsafe": Central perforations are generally safe; marginal and attic perforations are unsafe due to cholesteatoma risk.
- Healing: Small, dry traumatic perforations often heal spontaneously within weeks.
- Management: Keep ear dry; myringoplasty for persistent or symptomatic perforations.
- Blast injury: Often causes multiple perforations or subtotal/total loss of the tympanic membrane.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

