Introduction & Etiopathogenesis - Ear Canal Calamity
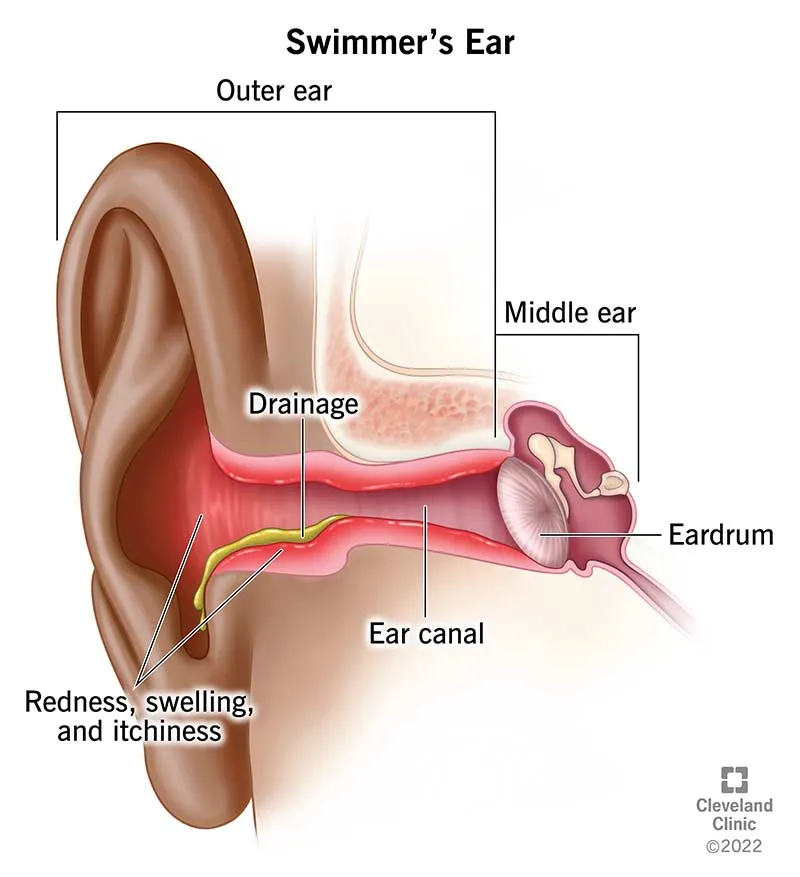
- Otitis Externa (OE): Inflammation or infection of the external auditory canal (EAC); acute diffuse type often called "Swimmer's Ear".
- Etiology:
- Bacterial (Most Common): Pseudomonas aeruginosa (predominant), Staphylococcus aureus.
- Fungal (Otomycosis): Aspergillus spp. (e.g., A. niger - black spores), Candida spp.
- Non-infectious: Eczematous, seborrheic dermatitis, contact sensitivity.
- Pathogenesis:
- Breakdown of protective skin-cerumen barrier & loss of acidic pH in EAC.
- Predisposing Factors: Moisture (swimming, humidity), trauma (e.g., cotton swabs, scratching), alkaline soaps, ↓cerumen.
- Leads to canal skin inflammation, edema, erythema, severe otalgia, and otorrhoea.
⭐ Pseudomonas aeruginosa is the predominant pathogen in up to 70% of acute diffuse otitis externa cases, thriving in moist environments.
Clinical Picture & Diagnosis - Itchy, Ouchy Ears
- Symptoms:
- Severe otalgia: ↑ with tragal/pinna movement.
- Pruritus: Esp. fungal (otomycosis).
- Otorrhea: Scanty, watery/purulent.
- Conductive hearing loss: Due to canal edema/debris.
- Aural fullness.
- Signs (Otoscopy):
- Tragal tenderness: Key sign.
- Pinna tenderness.
- External Auditory Canal (EAC): Edema, erythema.
- Debris in EAC:
- Bacterial: Wet, "blotting paper" appearance.
- Fungal: Fluffy, white/black/yellow dots (Aspergillus/Candida).
- Tympanic Membrane (TM): Usually mobile, may be obscured.
- Diagnosis: Primarily clinical. Swab for culture & sensitivity (C&S) if refractory/recurrent.
⭐ Tenderness on tragal pressure or pulling the pinna is a hallmark sign of otitis externa.
OE Variants & Red Flags - Ear's Wild Side
- Malignant (Necrotizing) OE (MOE):
- Pseudomonas aeruginosa in elderly diabetics/immunocompromised.
- Severe nocturnal otalgia, purulent discharge.
- Key: Granulation tissue at bony-cartilaginous junction.
- ⚠️ CN VII palsy common; others (IX-XII) possible.
- Dx: CT/MRI (bone erosion), biopsy crucial.
- Tx: IV antipseudomonals (e.g., Ciprofloxacin 6-8 wks), surgical debridement.

- Fungal OE (Otomycosis):
- Aspergillus spp. (black/grey spores, "wet newspaper" look).
- Candida spp. (white/creamy hyphae, "cottage cheese" look).
- Intense itching (pruritus), visible fungal debris.
- Tx: Thorough aural toilet, topical antifungals (e.g., Clotrimazole).
- Eczematous OE:
- Chronic itching, scaling, erythema. Often bilateral.
- Associated with dermatitis/psoriasis. Tx: Topical steroids.
- General Red Flags (⚠️ Refer Urgently):
- Severe pain disproportionate to findings.
- Cranial nerve deficits (esp. facial nerve).
- Immunocompromised status (Diabetes, HIV).
- No improvement in 48-72 hrs with topical Rx.
- Cellulitis spreading beyond External Auditory Canal (EAC).
⭐ Granulation tissue at the bony-cartilaginous junction of the External Auditory Canal in an elderly diabetic patient is a hallmark of Malignant Otitis Externa (Necrotizing Otitis Externa).
Management & Prevention - Soothing the Swimmer's Ear
📌 Mnemonic: CLEANSE
- Cleaning (Aural Toilet): Gentle suction/dry mopping. Essential first step.
- Local Therapy (Topical):
- Antibiotic drops: Fluoroquinolones (ciprofloxacin, ofloxacin) preferred.
- Add corticosteroids (dexamethasone) to reduce inflammation.
- Acidifying agents (e.g., 2% acetic acid) restore canal pH.
- Ear Wick: Use if canal edema obstructs drop delivery.
- Analgesia: Systemic NSAIDs (ibuprofen, paracetamol) for pain relief.
- No Water / Systemic Antibiotics:
- Keep ear dry (crucial for healing).
- Systemic oral fluoroquinolones for severe infection (cellulitis), immunocompromised, or failed topical treatment.
⭐ Topical fluoroquinolones (e.g., ciprofloxacin) are preferred over aminoglycosides if tympanic membrane integrity is uncertain, due to lower ototoxicity risk.
Prevention Strategies (Education - the final 'E' of CLEANSE):
- Keep ear canal dry: Use earplugs (swimming), thorough drying post-water.
- Avoid ear trauma: No cotton swabs, avoid scratching canal.
- Prophylactic drops: Acetic acid 2% or alcohol-based solutions after water exposure.
High-Yield Points - ⚡ Biggest Takeaways
- Most common cause: Pseudomonas aeruginosa.
- Key symptom: Severe otalgia exacerbated by tragal pressure or pinna movement.
- Malignant Otitis Externa: Aggressive infection in diabetics/immunocompromised; Pseudomonas implicated; can cause facial palsy and skull base osteomyelitis.
- Otomycosis: Fungal infection (e.g., Aspergillus, Candida); intense itching is characteristic.
- Treatment: Aural toilet, topical antibiotics +/- steroids. Systemic for severe cases.
- Prevention: Keep ears dry; avoid trauma (e.g., cotton swabs).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

