CLM Etiopathogenesis - Uninvited Skin Crawlers
- Causative Agents: Primarily zoonotic hookworm larvae. Humans are accidental, dead-end hosts.
- Ancylostoma braziliense (cats, dogs) - Most frequent.
- Ancylostoma caninum (dogs).
- Uncinaria stenocephala (dogs).
- Bunostomum phlebotomum (cattle).
- Transmission:
- Filariform (L3) larvae in warm, moist, sandy soil contaminated with animal feces.
- Larvae penetrate intact or abraded human skin upon contact.
- Pathogenesis:
- Larvae migrate within the epidermis or at the dermo-epidermal junction (stratum basale).
- Cannot invade deeper dermis (lack collagenases for human basement membrane).
- Intense, localized eosinophilic inflammatory response (Th2-mediated) to larval antigens and movement causes characteristic pruritic, erythematous, serpiginous (
CLM Clinical Features - Serpentine Skin Signs
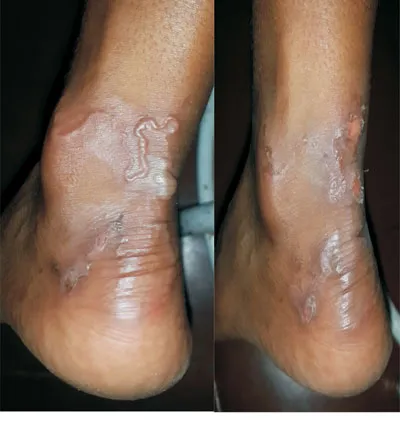
- Hallmark: Intensely pruritic, erythematous, serpiginous, or linear tracts.
- Lesions are typically 1-5 mm wide.
- Raised, palpable burrows are characteristic.
- Progression: Tracts advance as larvae migrate.
⭐ Larvae typically migrate 1-2 cm per day.
- Common Sites: (Areas of skin contact with contaminated soil/sand)
- Feet (most common)
- Buttocks
- Thighs
- Hands
- Associated Features:
- Vesicles or bullae may form along the tracts.
- Excoriations due to intense itching.
- Secondary bacterial infection (e.g., impetigo) is common from scratching.
- Symptoms:
- Intense itching (pruritus), often worse at night.
- Tingling or stinging sensation at the site of larval penetration.
- Pain is uncommon unless secondarily infected.
- 📌 Mnemonic: S.C.R.A.T.C.H. (Serpiginous, Creeping, Red, Advancing, Tracts, Causing, Horrible itch)
CLM Diagnosis - Spotting the Squiggle
- History: Exposure to soil/sand contaminated by animal (dog/cat) feces; travel to endemic tropical/subtropical areas.
- Clinical Findings:
- Intensely pruritic, erythematous, raised, serpiginous/linear tracts ("creeping eruption").
- Track advances 1-2 cm/day. Width: 2-3 mm.
- Common sites: Feet, buttocks, hands, thighs.
- Investigations (Usually not needed):
- Dermoscopy: May show larva at advancing end of the burrow.
- Biopsy (rare): Eosinophilic infiltrate. Peripheral eosinophilia possible.
⭐ Diagnosis is primarily clinical; biopsy is rarely indicated and usually not necessary for confirmation based on the characteristic presentation and history of exposure in endemic regions for Cutaneous Larva Migrans (CLM).
CLM Management - Evicting the Itch
- Goal: Kill larva, relieve itch, prevent secondary infection.
- Topical Therapy (mild/localized):
- Thiabendazole (10-15% solution/cream) BID-TID for 7-10 days.
- Cryotherapy (liquid nitrogen) to advancing end of burrow.
- Systemic Therapy (widespread/severe/failed topical):
- Ivermectin: 200 µg/kg single dose (preferred).
- Albendazole: 400 mg daily for 3-7 days.
- Symptomatic Relief:
- Antihistamines for pruritus.
- Antibiotics if secondary bacterial infection.
⭐ Oral Ivermectin (200 µg/kg single dose) or Albendazole (400 mg daily for 3-7 days) are effective systemic treatments.
- Prevention: Avoid skin contact with fecally contaminated soil (e.g., wear footwear, use protective barriers on beaches).
High‑Yield Points - ⚡ Biggest Takeaways
- Caused by larvae of animal hookworms (e.g., Ancylostoma braziliense) from fecally contaminated soil.
- Presents as intensely pruritic, erythematous, raised, serpiginous tracts on skin - "creeping eruption".
- Larvae migrate 1-2 cm/day within the epidermis; humans are accidental dead-end hosts.
- Common sites: feet, buttocks, thighs, hands (areas of direct skin contact with soil).
- Diagnosis is clinical, based on characteristic lesions and exposure history.
- Treatment: Oral Albendazole or Ivermectin; topical Thiabendazole.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

