Introduction - Deep Skin Invaders
- Fungi invade dermis, subcutaneous tissue, muscle, fascia.
- Chronic, localized infections.
- Caused by diverse, saprophytic fungi.
- Portal of entry: Skin trauma (thorns, splinters).
- Organisms reside in soil, decaying vegetation.
- Infections often indolent, slowly progressive.
- Host immunity plays a key role in disease manifestation.
⭐ Subcutaneous mycoses typically result from traumatic inoculation of fungi from soil or vegetation into deeper skin layers.
- Common in tropical/subtropical regions, agricultural workers.
- Diagnosis: Microscopy, culture, histopathology, molecular tests (PCR).
Sporotrichosis - Rose Gardener's Revenge
- Agent: Sporothrix schenckii (thermally dimorphic fungus).
- Transmission: Traumatic inoculation from soil, sphagnum moss, rose thorns.
- Clinical Forms:
- Lymphocutaneous (most common): Initial papule → ulcerates. Nodules ascend along lymphatics ("sporotrichoid spread").
- Fixed cutaneous: Solitary chronic plaque/ulcer.
- Disseminated: Rare; in immunocompromised (joints, lungs).
- Diagnosis:
- Culture (gold standard): Tissue/pus. Yeast at 37°C, mold at 25°C.
- Biopsy: Granulomatous inflammation; cigar-shaped yeast cells.
⭐ The presence of asteroid bodies (Splendore-Hoeppli phenomenon) surrounding yeast cells is characteristic but not pathognomonic for sporotrichosis.
- Treatment:
- Itraconazole (DOC for cutaneous/lymphocutaneous).
- SSKI (Saturated Solution of Potassium Iodide).
- Amphotericin B (severe/disseminated).

Chromo & Phaeo - Dark Fungi Drama
- Caused by dematiaceous (dark-walled/pigmented) fungi.
- Chromoblastomycosis:
- Etiology: Fonsecaea pedrosoi, Phialophora verrucosa, Cladophialophora carrionii.
- Clinical: Chronic, progressive; verrucous, crusted, warty, “cauliflower-like” plaques/nodules. Often on lower limbs.
- Diagnosis: Histopathology shows pathognomonic sclerotic bodies (Medlar bodies, “copper pennies”).
- Treatment: Itraconazole, terbinafine, local heat therapy, surgery.
- Phaeohyphomycosis:
- Etiology: Heterogeneous group of pigmented fungi (e.g., Exophiala, Wangiella, Bipolaris).
- Clinical: Highly variable; subcutaneous cysts/abscesses, sinusitis, keratitis, brain abscess (especially in immunocompromised).
- Diagnosis: Pigmented (brown/black) septate hyphae, yeast-like cells, or pseudohyphae in tissue; NO sclerotic bodies.
- Treatment: Surgical excision + antifungals (e.g., itraconazole, voriconazole, amphotericin B).
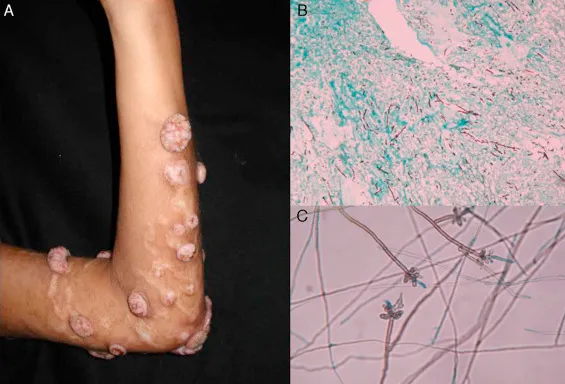
⭐ Sclerotic bodies (Medlar bodies or 'copper pennies') are pathognomonic for chromoblastomycosis and represent fungal cells undergoing cell division by fission.
Mycetoma - Grainy Swellings Saga

- Chronic granulomatous infection: skin, subcutaneous tissue. Often foot (Madura foot), hand.
- Triad: Painless swelling, multiple sinuses, discharge of grains.
- Types & Grains:
- Eumycetoma (fungal): Madurella mycetomatis (black grains). Slower progression.
- Actinomycetoma (bacterial): Nocardia, Actinomadura (white/yellow/red grains). Faster progression. 📌 "Actino Ants March with Sulfa Drugs" (Actinomycetoma treated with antibiotics like sulfonamides).
⭐ The color of grains discharged from sinuses in mycetoma (e.g., black, white, yellow, red) can provide a clue to the causative organism (eumycetoma vs. actinomycetoma).
- Dx: Clinical, grain microscopy (KOH, Gram), culture, imaging (X-ray, USG, MRI - "dot-in-circle" sign).
- Rx:
- Eumycetoma: Antifungals (e.g., itraconazole) + surgical debridement.
- Actinomycetoma: Antibiotics (e.g., Welsh regimen: TMP-SMX + Dapsone/Amikacin).
High‑Yield Points - ⚡ Biggest Takeaways
- Sporotrichosis: "Rose gardener's disease", lymphocutaneous spread along lymphatics; Sporothrix schenckii.
- Mycetoma: Triad: tumefaction, draining sinuses, grains/granules; Madurella mycetomatis (eumycetoma, black grains).
- Chromoblastomycosis: Verrucous/warty lesions, pathognomonic sclerotic bodies (Medlar bodies/copper pennies).
- Rhinosporidiosis: Nasal/ocular friable polyps; R. seeberi showing large sporangia with endospores.
- Typically from traumatic inoculation of soil fungi; diagnosis by microscopy (KOH, biopsy) & culture.
- Treatment: Prolonged systemic antifungals (e.g., Itraconazole) often combined with surgical debridement.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

