Wound Healing - Healing's ABCs
📌 Mnemonic for phases: "Heavy Inflammation Produces Remodeling"
- Phases & Key Players:
- Hemostasis (mins-hrs): Platelets; PDGF, TGF-β. Platelet plug, clot.
- Inflammation (Day 1-6): Neutrophils, Macrophages; TNF-α, IL-1. Neutrophil & macrophage influx.
- Proliferation (Day 4 - Wk 3): Fibroblasts, Keratinocytes; VEGF, FGF, EGF. Granulation, re-epithelialization, new Collagen III.
- Remodeling (Wk 3 - 2 yrs): Myofibroblasts; MMPs. Collagen III → I, ↑ strength (~80% max).

- Factors Affecting Healing:
- Local: ↓O₂, infection, foreign body, poor perfusion.
- Systemic: Age, poor nutrition (Vit C, Zn, protein), DM, steroids, smoking.
- Acute vs. Chronic:
- Acute: Timely healing.
- Chronic: Stalled > 4-6 weeks.
⭐ Chronic wounds are often stalled in the inflammatory phase due to persistent stimuli or impaired cellular responses.
Wound Assessment & Prep - Clean Sweep
- Assessment Parameters:
- Site, Size (LxWxD cm), Depth (cm), Exudate (type, amount, odour)
- Wound Bed: % Necrotic (black), Sloughy (yellow), Granulating (red), Epithelializing (pink)
- Surrounding Skin: Colour, oedema, maceration, induration, cellulitis
- Infection Signs: Classic (rubor, calor, tumor, dolor), ↑exudate, delayed healing, odour.
- Cleansing:
- Solutions: Normal saline ($0.9%$ NaCl), potable water. Antiseptics (povidone-iodine) for infected wounds.
- Technique: Gentle irrigation.
- Debridement Types:
- Autolytic: Slow, selective (hydrocolloids, hydrogels).
- Enzymatic: Selective (collagenase).
- Mechanical: Non-selective (wet-to-dry, hydrotherapy); often painful.
- Sharp/Surgical: Fast; for extensive necrosis/infection.
- Biological: Selective (medical maggots). 📌 TIME Framework (wound bed prep): Tissue, Infection/Inflammation, Moisture, Edge.
⭐ The TIME framework (Tissue, Infection/Inflammation, Moisture, Edge) provides a systematic approach to wound bed preparation, guiding treatment choices.
Dressing Decisions - Material Matters
- Ideal Properties: Maintains moist environment, infection protection, non-adherent, gas exchange.
- Classification:
- Passive: Protective cover (e.g., gauze).
- Active: Promote healing.
- Interactive: Modulate wound bed (e.g., hydrocolloids).
- Common Dressing Types:
| Dressing Type | Key Feature/Mechanism | Common Indications | Advantages | Disadvantages |
|---|---|---|---|---|
| Gauze | Absorbent cotton/synthetic | Cleaning, packing, cover (dry/wet) | Cheap, versatile | Can dry, lint, may adhere |
| Films | Semi-permeable polyurethane | Superficial wounds, IV sites, secondary | Waterproof, visualize | No absorption, traps moisture |
| Foams | Absorbent polyurethane | Mod-heavy exudate | Cushioning, absorbent | Can dry small wounds, bulky |
| Hydrocolloids | Gel-forming (CMC) | Low-mod exudate, non-infected | Occlusive, autolysis | Odor, not for infected |
| Hydrogels | High water content (sheets/gels) | Dry, sloughy, necrotic, burns | Hydrates, cooling, debrides | Maceration, needs secondary |
| Alginates | Seaweed (Ca-Na exchange) | Mod-heavy exudate, bleeding | Highly absorbent, hemostatic | Can dry, needs secondary |
| Silver (Ag+) | Antimicrobial Ag+ ions | Infected or high-risk | Broad-spectrum antimicrobial | Cost, cytotoxicity |
| Honey-based | Osmotic, antimicrobial | Various acute/chronic | Debrides, anti-inflammatory | Allergy, can sting |
- Dressing Selection Principles: Match dressing to wound characteristics:
- Exudate level (low, moderate, heavy)
- Wound depth (superficial, partial, full-thickness)
- Presence of infection or necrosis
- Condition of surrounding skin
⭐ Alginate dressings are highly absorbent and suitable for wounds with moderate to heavy exudate, forming a gel that maintains a moist environment.
Specific Wound Scenarios - Tricky Spots
-
Diabetic Foot Ulcers (DFU):
- Key: Offloading, glycemic control, debridement, infection check.
- Dressings: Moisture-retentive (hydrogels, foams); antimicrobials if infected. Wagner grades 0-5.
⭐ Effective offloading is the cornerstone of diabetic foot ulcer management and prevention, significantly impacting healing outcomes.
-
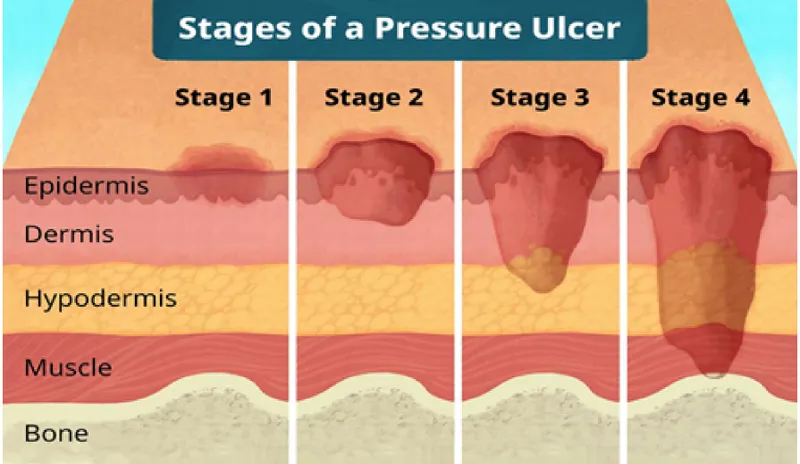
Pressure Ulcers:
- Prevention vital. Staging (I-IV, Unstageable, DTPI).
- Dressings: Stage I: Film. Stage II: Hydrocolloid/foam. Stage III/IV: Alginate/hydrofiber for exudate, consider antimicrobials.
-
Burns:
- Assess depth & %TBSA (Rule of Nines).
- Superficial (1st/2nd degree): Non-adherent, moisture-retentive.
- Deep (2nd/3rd degree): Antimicrobials (e.g., silver-based), pain control.
-
Venous Leg Ulcers (VLU):
- Key: Compression therapy.
- Dressings: Absorbent (foams, alginates) for exudate, under compression.
High‑Yield Points - ⚡ Biggest Takeaways
- Wound cleansing is crucial; normal saline is preferred for most acute wounds.
- Debridement removes necrotic tissue; autolytic debridement is slowest, surgical is fastest.
- Moist wound healing is superior to dry for epithelialization and reduced scarring.
- Occlusive dressings (e.g., hydrocolloids) promote moist healing and autolytic debridement.
- Silver-impregnated dressings are used for infected wounds or those at high risk of infection.
- Negative Pressure Wound Therapy (NPWT) promotes granulation tissue formation in complex wounds.
- Honey-based dressings offer antimicrobial and anti-inflammatory properties for certain wounds.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

