Neonatal Skin - Fresh & Fragile
- Physiological Findings:
- Vernix Caseosa: Waxy, white, protective coating.
- Lanugo: Fine, soft hair; sheds weeks 1-2.
- Acrocyanosis: Peripheral cyanosis; resolves with warming.
- Cutis Marmorata: Mottled vascular pattern; cold stress.
- Physiological Desquamation: Peeling, esp. post-term.
- Benign Transient Rashes:
- Erythema Toxicum Neonatorum (ETN): "Flea-bitten" rash; macules, papules, pustules on erythematous base. Appears day 2-5, spares palms/soles.
⭐ ETN smear shows numerous eosinophils.
- Transient Neonatal Pustular Melanosis (TNPM): Pustules at birth → collarettes of scale → pigmented macules. Neutrophils on smear.
- Milia: Tiny white keratin cysts; face (nose, chin).
- Miliaria: Sweat duct obstruction.
- Miliaria Crystallina: Superficial clear vesicles.
- Miliaria Rubra (Prickly Heat): Erythematous papules/pustules.
- Sebaceous Gland Hyperplasia: Yellowish papules on nose/cheeks; maternal androgens.
- Erythema Toxicum Neonatorum (ETN): "Flea-bitten" rash; macules, papules, pustules on erythematous base. Appears day 2-5, spares palms/soles.

Birthmarks - Unique Stamps
- Vascular Birthmarks:
- Nevus Simplex (Salmon Patch/Stork Bite): Common, flat, pink patches (nape, eyelids, glabella). Usually fade by 1-2 years.
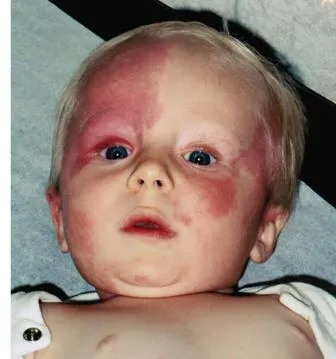
- Port-Wine Stain (Nevus Flammeus): Dark red/purple vascular malformation. Permanent, grows with child. If V1 ophthalmic trigeminal distribution, suspect Sturge-Weber syndrome.
- Infantile Hemangioma (Strawberry Nevus): Bright red, raised. Proliferate in first months, then involute. Propranolol for complicated cases (e.g., visual obstruction).
- Pigmented Birthmarks:
- Mongolian Spot (Congenital Dermal Melanocytosis): Blue-grey macules, lumbosacral area. Common in Asian/darker skin. Fade in childhood.
- Café-au-Lait Macules (CALMs): Light brown, flat. Multiple (>6 lesions, >5mm prepubertal, >15mm postpubertal) suggest Neurofibromatosis Type 1 (NF1).
- Congenital Melanocytic Nevus (CMN): Brown/black. Risk of melanoma ↑ with size (especially giant CMNs >20cm).
- Epidermal Nevi:
- Nevus Sebaceous (of Jadassohn): Yellowish, waxy, hairless plaque (often scalp). Risk of secondary benign/malignant neoplasms (e.g., BCC) in adulthood.
⭐ Port-wine stain in the V1 trigeminal nerve distribution is highly suggestive of Sturge-Weber syndrome, which can involve ipsilateral glaucoma and leptomeningeal angiomas causing seizures and neurological deficits.
Pediatric Infections - Tiny Invaders
- Impetigo: S. aureus, Group A Strep. Honey-colored crusts (non-bullous); flaccid bullae (bullous). Topical/oral antibiotics.
- Molluscum Contagiosum: Poxvirus. Flesh-colored, umbilicated papules. Spontaneous resolution common.
- Scabies: Sarcoptes scabiei. Intense nocturnal pruritus. Burrows (interdigital, wrists, axillae). Permethrin 5% cream. Treat contacts.

- Tinea Capitis: Dermatophytes. Scalp scaling, alopecia, black dots, kerion. Oral griseofulvin.
⭐ Wood's lamp: Microsporum spp. fluoresce green.
- Viral Warts (Verrucae): HPV. Common (vulgaris), flat (plana), plantar. Salicylic acid, cryotherapy.
- Hand-Foot-Mouth Disease (HFMD): Coxsackie A. Oral, hand, foot vesicles. Supportive care.
Inflammatory Dermatoses - Itchy Issues
- Atopic Dermatitis (AD): "Itch that rashes"; chronic, relapsing.
- Infants: Face, extensors. Spares diaper area.
- Children: Flexures.
- Associated with atopic march. Filaggrin mutations.
- Tx: Emollients, topical steroids, TCIs.
- Seborrheic Dermatitis (SD): Greasy scales, erythema.
- Infants: "Cradle cap" (scalp), face, diaper area.
- Malassezia implicated.
- Tx: Antifungal shampoos, mild topical steroids.
- Psoriasis: Well-demarcated silvery plaques.
- Extensors, scalp, nails. Auspitz sign, Koebner.
- Guttate psoriasis: Post-streptococcal.
- Contact Dermatitis:
- Irritant (ICD): Direct injury (e.g., diapers, soaps).
- Allergic (ACD): Type IV hypersensitivity (e.g., nickel). Patch test.
⭐ Infantile atopic dermatitis typically affects the face (cheeks, chin, forehead) and extensor surfaces, often sparing the diaper area.

High‑Yield Points - ⚡ Biggest Takeaways
- Neonatal acne (first weeks, resolves) vs. Infantile acne (3-6 months, may scar, more persistent).
- Erythema toxicum neonatorum: Benign "flea-bitten" rash with eosinophils, resolves in days.
- Mongolian spots: Common benign blue-grey lumbosacral macules, typically fade during childhood.
- Infantile hemangiomas: Characteristically proliferate then involute; propranolol for problematic lesions.
- Atopic dermatitis: Key feature is intense pruritus; distribution varies with age (infant vs. child).
- Diaper dermatitis: Irritant contact is most common; Candidal infection presents with satellite pustules.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

