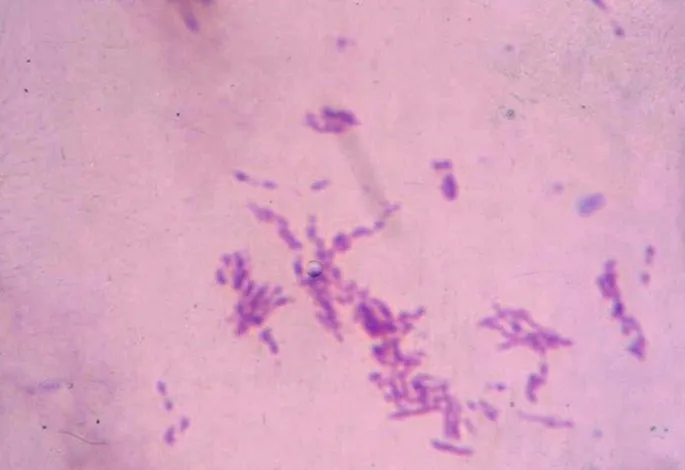
Introduction & Microbiology - Ancient Affliction
- Causative agent: Mycobacterium leprae (Hansen's bacillus).
- Acid-fast, obligate intracellular bacillus; rod-shaped.
- Slow generation time: 12-14 days.
- Optimal growth temperature: 27-33°C (cooler body areas).
- Reservoirs: Humans, nine-banded armadillos.
- Transmission: Primarily respiratory droplets; prolonged close contact.
- Long incubation period: Avg 2-5 years (up to 20 years).
⭐ Mycobacterium leprae is an obligate intracellular parasite that cannot be cultured on artificial media.

Classification - Spectrum Story
Leprosy is a spectrum based on host Cell-Mediated Immunity (CMI).
-
Ridley-Jopling (R-J) Spectrum:
- Tuberculoid (TT): ↑CMI, few bacilli. Well-defined lesions, early nerve damage.
- Lepromatous (LL): ↓CMI, many bacilli. Diffuse lesions, late nerve damage.
- Borderline (BT, BB, BL): Intermediate, unstable forms.
-
WHO Classification (Treatment):
- Paucibacillary (PB): ≤5 skin lesions AND smear negative. (Mainly TT, BT).
- Multibacillary (MB): >5 skin lesions OR smear positive OR >1 nerve involved. (Mainly LL, BL, BB).
⭐ CMI is strongest in Tuberculoid (TT) leprosy (few bacilli, localized) and weakest in Lepromatous (LL) leprosy (many bacilli, disseminated).
Clinical Features - Nerve & Skin Tales
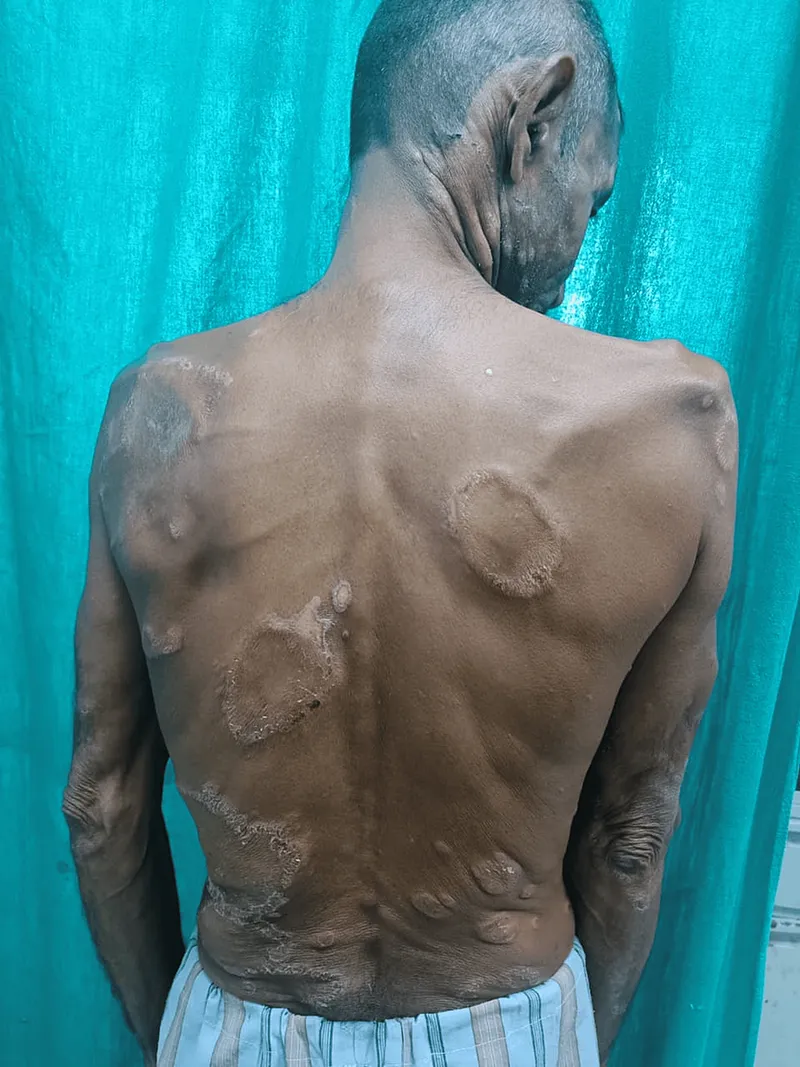
- Skin Lesions ("Patches & Plaques")
- One/more hypopigmented or reddish skin patches.
- Definite sensory loss (touch, pain, temperature) within patches.
- Plaques, nodules; skin can be shiny, dry, or thickened.
- Late: Madarosis (eyebrow/eyelash loss), leonine facies (LL).
- Nerve Damage ("Silent Sabotage")
- Thickened, often tender, peripheral nerves (e.g., ulnar, common peroneal, great auricular).
- Sensory loss: Fine touch, pain, temperature affected early.
- Motor loss: Muscle weakness, paralysis leading to deformities (e.g., claw hands, foot drop, lagophthalmos).
- Autonomic dysfunction: Anhidrosis (reduced sweating), dry/cracked skin.

⭐ The ulnar nerve is the most commonly affected peripheral nerve in leprosy, followed by the common peroneal nerve.
Diagnosis - Unmasking Hansen's
- Slit-Skin Smear (SSS):
- Sites: Earlobes, active lesions. Ziehl-Neelsen (ZN) stain for Acid-Fast Bacilli (AFB).
- Bacteriological Index (BI): Measures bacillary load, graded 0 to 6+.
- Morphological Index (MI): Percentage of solid, uniformly stained (viable) bacilli; MI ↓ with effective treatment.
- Histopathology (Biopsy): Confirms diagnosis & classifies leprosy type (e.g., granuloma structure, lymphocyte infiltration, bacillary presence).
- Nerve Biopsy: Useful in pure neuritic leprosy when skin lesions are absent.
- PCR: Detects M. leprae DNA; high sensitivity, especially in paucibacillary (PB) or early cases.
⭐ The Lepromin test (Fernandez and Mitsuda reactions) is negative in lepromatous leprosy (LL, BL) and positive in tuberculoid leprosy (TT, BT), indicating Cell-Mediated Immunity (CMI) status.
Management & Reactions - Healing & Hazards
- MDT Regimens (WHO):
Category Drugs Duration PB Rifa (600mg M) + Dap (100mg D) 6 mo MB Rifa (600mg M) + Dap (100mg D) + Clofa (300mg M, 50mg D) 12 mo SLPB SDR: Rifa (600mg) + Oflox (400mg) + Mino (100mg) Single - Lepra Reactions: MDT always continued.
⭐ Thalidomide is drug of choice for severe Type 2 lepra reaction (ENL) but is strictly contraindicated in pregnancy due to teratogenicity.
High‑Yield Points - ⚡ Biggest Takeaways
- Caused by Mycobacterium leprae; primarily affects skin and peripheral nerves.
- Spectrum: Paucibacillary (PB) (strong CMI, e.g., TT) to Multibacillary (MB) (poor CMI, e.g., LL).
- Cardinal signs: anesthetic skin lesions, thickened peripheral nerves, positive slit-skin smear (MB).
- Lepra Reactions: Type 1 (Reversal, cell-mediated) and Type 2 (ENL, immune complex).
- Treatment: WHO Multidrug Therapy (MDT) with Rifampicin, Dapsone, Clofazimine.
- Nerve damage is the hallmark, leading to significant disability and deformity.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more