Tetanus: Agent & Epi - Lockjaw Lowdown
- Agent: Clostridium tetani
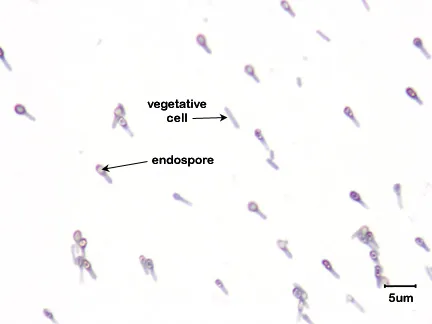
- Gram-positive, anaerobic, spore-forming bacillus.
- Produces potent neurotoxin: Tetanospasmin.
- Reservoir: Soil, dust, animal (especially horse) feces.
⭐ Spores of Clostridium tetani are highly resistant, found in soil and animal feces, and can survive for years.
- Transmission:
- Contamination of wounds (punctures, abrasions, burns) with spores.
- Unhygienic delivery practices (Neonatal Tetanus - NNT).
- Unsterile surgical procedures, ear piercing, tattooing, animal bites.
- Incubation Period: Typically 3-21 days (average 10 days); can range from 1 day to several months.
- Epidemiology (India):
- MNTE (Maternal and Neonatal Tetanus Elimination) status achieved (2015).
- Non-neonatal tetanus cases still occur.
- Higher risk in unimmunized or inadequately immunized individuals.
Tetanus: Clinical Features - Spasms & Symptoms
- Incubation: 3-21 days (avg. 10); shorter IP → severe disease.
- Early:
- Trismus (lockjaw): commonest initial sign.
- Neck stiffness, dysphagia, restlessness.
- Spasms (Tetanospasms):
- Painful, involuntary, reflex; triggered by minimal stimuli (noise, light).
- Generalized:
-
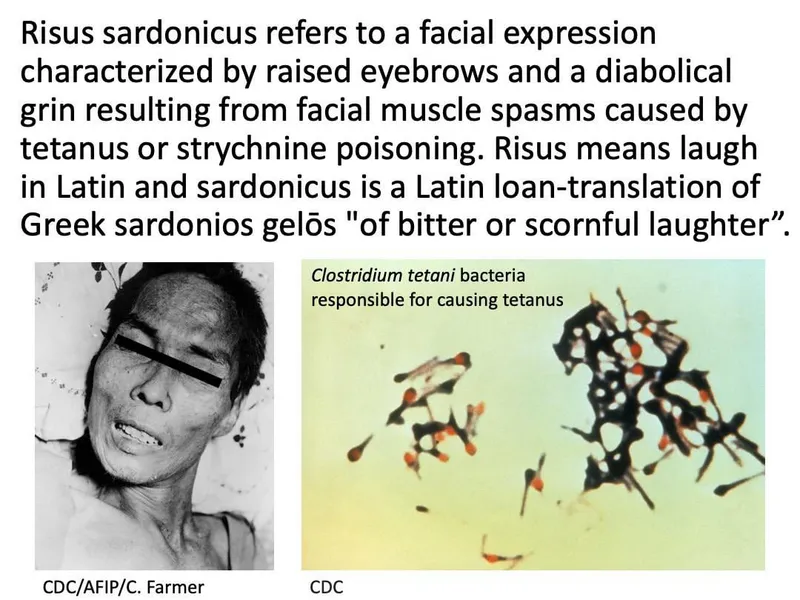
Risus sardonicus (fixed grin).
-
Opisthotonus (back arching).
-
Abdominal rigidity (board-like).
-
Laryngeal/pharyngeal spasms → respiratory distress.
-
- Autonomic dysfunction (severe cases): labile BP/HR, sweating, fever.
- Consciousness: Usually alert.
⭐ Tetanospasmin neurotoxin blocks inhibitory neurotransmitter (GABA, glycine) release in CNS, causing disinhibition of motor neurons & spasms.
Tetanus: Management - Unlocking the Patient
- Primary Goals: Neutralize unbound toxin, stop C. tetani growth, control spasms, ensure supportive care.
- Wound Management: Surgical debridement of necrotic tissue.
- Antitoxin:
- Human Tetanus Immunoglobulin (HTIG): 3000-5000 IU IM (single dose).
- Equine Antitoxin (ATS): 50,000-100,000 IU IV/IM (after sensitivity test, if HTIG unavailable).
- Antibiotic Therapy:
- Metronidazole (DOC): 500mg IV q6-8h for 10-14 days.
- Penicillin G (alternative): 10-12 million units/day IV (caution: may worsen spasms).
- Control of Spasms & Rigidity:
- Benzodiazepines: Diazepam 10-20mg IV q3-8h or Midazolam infusion.
- Magnesium Sulfate: 5g IV loading, then 1-2g/hr IV ($MgSO_4$).
- Severe cases: Neuromuscular blockers + mechanical ventilation.
- Supportive Measures: Airway protection, adequate nutrition, quiet/dark room, manage autonomic instability.
⭐ Human Tetanus Immunoglobulin (HTIG) is preferred over equine antitoxin (ATS) for passive immunization due to a lower risk of anaphylaxis.
Tetanus: Prevention & Control - Shield Against Tetanus
-
Active Immunization: Tetanus Toxoid (TT); Td vaccine for older children/adults.
- NIS: DPT (6, 10, 14 wks); Boosters: DPT (16-24 mths, 5-6 yrs), TT (10, 16 yrs).
- Pregnant Women: Two TT/Td doses (or one booster if primary series complete & last dose <10 yrs).
-
Passive Immunization (Post-Exposure Prophylaxis):
- Human Tetanus Immunoglobulin (hTIG): 250-500 IU IM.
- Equine Anti-Tetanus Serum (ATS): 3000-6000 IU IM (after sensitivity test).
-
Neonatal Tetanus (NNT) Prevention:
- Maternal immunization (TT/Td).
- Clean delivery practices & 📌 5 Cleans: Clean hands, surface, cord tie, blade, cord stump care.
-
Wound Management: Prompt surgical toilet, antibiotics (Metronidazole). Prophylaxis per flowchart.
-
Control Strategies: High routine immunization coverage, surveillance, clean deliveries.
⭐ India achieved Maternal and Neonatal Tetanus Elimination (MNTE) status in August 2015.
High‑Yield Points - ⚡ Biggest Takeaways
- Agent: C. tetani (anaerobe, spores); Toxin: Tetanospasmin (blocks GABA/glycine).
- Signs: Trismus (lockjaw), risus sardonicus, opisthotonus, painful spasms.
- NNT: Prevented by maternal TT & clean delivery; India achieved NNT elimination.
- Prophylaxis: Active immunization (TT/Td), passive (TIG), meticulous wound care.
- Clean Wounds: TT if <3 doses or last dose >10 yrs.
- Tetanus-prone Wounds: TT + TIG if <3 doses/unknown; TT if last dose >5 yrs.
- Pregnant Women: Two TT/Td doses or one booster if vaccinated_previously_vaccinated_
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

