Introduction & Pathophysiology - Sizzling Science
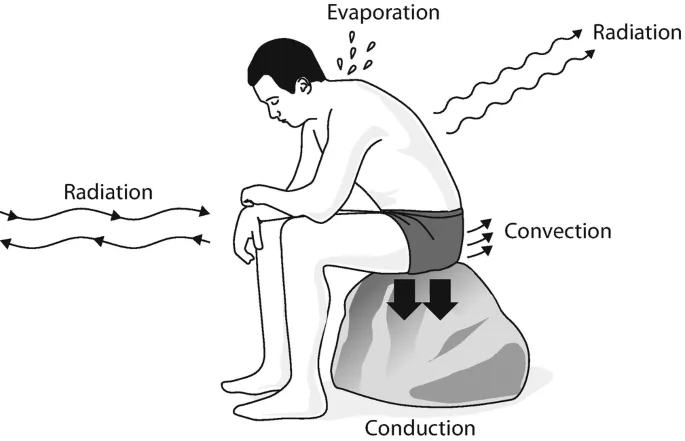
- Thermoregulation: Body balances heat gain (metabolism, environment) & loss (radiation, conduction, convection, evaporation).
- Acclimatization: Physiological adaptation to heat over days/weeks (↑sweat rate, ↓electrolyte loss).
- Pathophysiology: Excessive heat → thermoregulatory failure → hyperthermia.
- Cellular injury (protein denaturation, membrane damage) → organ dysfunction.
- Systemic Inflammatory Response Syndrome (SIRS) can occur.
- Risk Factors:
- Extremes of age (infants, elderly >65 yrs).
- Chronic diseases (CVD, diabetes, respiratory).
- Medications (diuretics, anticholinergics, β-blockers, antipsychotics).
- Dehydration, obesity, alcohol.
- High humidity, strenuous exertion, lack of acclimatization.
⭐ Evaporation is the primary heat loss mechanism, significantly impaired by high humidity (>75%).
Spectrum & Diagnosis - Degrees of Danger
| Feature | Heat Cramps | Heat Syncope | Heat Exhaustion | Heat Stroke (Classic/Exertional) |
|---|---|---|---|---|
| Core Temp | Normal/Slight ↑ | Normal/Slight ↑ | <40°C | >40°C |
| CNS | Alert | Transient LOC/dizzy | Fatigue, weakness, headache; No severe CNS | Severe CNS (delirium, seizures, coma) |
| Skin | Normal | Cool, moist | Profuse sweat; Cool/clammy | Classic: Hot, DRY. Exertional: SWEATY. |
| Muscles | Spasms (legs, abd) | - | Myalgia | Rhabdo (exertional) |
| CVS | Normal | Orthostatic hypotension | Tachycardia, hypotension | Tachycardia, hypotension → shock |
| GIT | - | - | Nausea, vomiting | Nausea, vomiting |
| Key Features | Isolated cramps; Normal temp | Brief LOC post-exertion | Systemic; Temp <40°C; No severe CNS. Water/salt depletion. | Temp >40°C; Severe CNS. EMERGENCY. |
⭐ Defining feature: Heat stroke vs. exhaustion is CNS dysfunction (AMS, seizures, coma) & core temp >40°C.
Management Principles - Chill & Conquer
- General: ABCs, remove from heat, rest, cooling, fluid & electrolyte replacement.
- Heat Cramps: Cool environment, ORS, gentle muscle stretching.
- Heat Syncope: Supine, legs elevated, cool environment, oral fluids.
- Heat Exhaustion: Cool place, oral rehydration (ORS). IV 0.9% saline if severe/vomiting. Monitor core temp.
- Heat Stroke: ⚠️ EMERGENCY! IMMEDIATE AGGRESSIVE COOLING.
- Target core temp: ~39°C (102.2°F).
- Methods: Evaporative (tepid water + fan), ice packs (neck, axillae, groin), cooling blankets, cold water immersion.
- IV isotonic crystalloids.
- Manage complications (seizures: benzodiazepines).
- ⚠️ Antipyretics (paracetamol, aspirin) NOT effective/harmful.

⭐ In heat stroke management, rapid cooling to a target core temperature of ~39°C is paramount; antipyretics are ineffective.
Prevention & Control - Beat The Heat
- Individual Measures: Acclimatize (gradual exposure); hydrate regularly (avoid alcohol/caffeine); wear light-colored, loose-fitting clothes; schedule outdoor activities in cooler parts of day; use sunscreen; never leave children/pets in parked cars.
- 📌 AVOID HEAT: Acclimatize, Ventilate, Overhydration (avoid, but hydrate well!), Inform (stay informed), Dress light, Hydrate, Energy (conserve), Activity (limit peak heat), Time (schedule wisely).
- Community/Public Health Measures: Heat Action Plans (HAPs), Heat Health Warning Systems (HHWS), public cooling centers, urban planning (green spaces), awareness campaigns.
- Focus on Vulnerable Populations: Elderly, infants/young children, pregnant women, outdoor workers, athletes, individuals with chronic conditions.

⭐ Acclimatization, achieved over 7-14 days of heat exposure, significantly improves physiological tolerance to heat stress by enhancing sweating efficiency and cardiovascular stability.
High‑Yield Points - ⚡ Biggest Takeaways
- Heat stroke: life-threatening, core temp >40°C with altered mental status.
- Heat exhaustion: core temp <40°C, fatigue, no major CNS issues.
- Heat stroke management: immediate rapid cooling (evaporative/immersion).
- Acclimatization over 7-14 days is key for prevention.
- High-risk: elderly, infants, chronic diseases, certain drugs (e.g., diuretics, anticholinergics).
- Heat cramps: painful spasms from electrolyte loss; treat with oral saline.
- Prickly heat (miliaria): blocked sweat ducts; keep skin cool, dry.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

