Hemoglobinopathies: Basics & Beyond
- Hemoglobinopathy: Inherited disorders affecting globin chain structure or synthesis.
- Classification:
- Structural: Altered globin (e.g., Sickle cell anemia, HbC).
- Quantitative (Thalassemias): Reduced synthesis of normal globin chains.
- Normal Adult Hemoglobins:
- HbA: $α_2β_2$ (>95%)
- HbA2: $α_2δ_2$ (1.5-3.5%)
- HbF: $α_2γ_2$ (<1-2%)

⭐ HbF (Fetal Hemoglobin) has a higher oxygen affinity than HbA, facilitating oxygen transfer from mother to fetus across the placenta.
Sickle Cell Saga: Bend & Break
- Pathophysiology: β-globin gene mutation ($Glu6Val$) leads to HbS. Under hypoxia, HbS polymerizes, causing RBCs to sickle.
- Clinical Features:
- Vaso-occlusive Crises (VOC): Pain (dactylitis, acute chest syndrome, stroke).
- Chronic Hemolysis: Anemia, jaundice, gallstones.
- Aplastic Crisis: Parvovirus B19.
- Functional asplenia: ↑ Infection risk.
- Diagnosis:
- Screening: Sickling test (sodium metabisulfite).
- Confirmatory: Hb electrophoresis or HPLC (shows HbS).
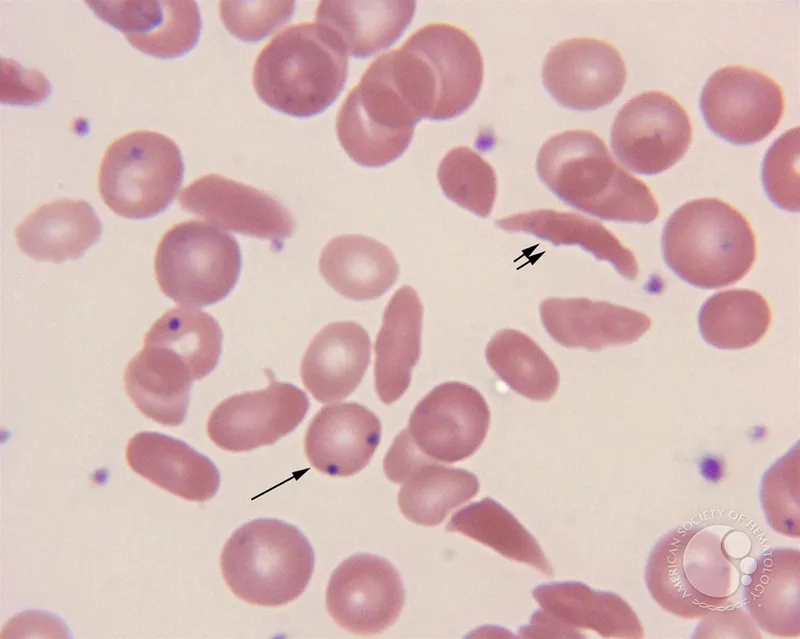
- Peripheral smear: Sickled cells, Howell-Jolly bodies.
- Management Principles:
- Avoid triggers, hydration, analgesia.
- Hydroxyurea (↑ HbF).
- Folic acid, infection prophylaxis (e.g., penicillin until age 5).
- Transfusions for severe anemia/crisis.
⭐ Acute Chest Syndrome is a leading cause of death in sickle cell disease patients and is characterized by new pulmonary infiltrate on chest X-ray plus fever and/or respiratory symptoms.
Thalassemia Tales: Chain Reaction
- Pathophysiology: Reduced synthesis of α or β globin chains → imbalanced globin chain production, ineffective erythropoiesis.
- Types:
Feature Alpha (α) Thalassemia Beta (β) Thalassemia Defect Gene deletions (Chr 16) Point mutations (Chr 11) Key Abnormal Hb Hb Bart's (γ4), HbH (β4) ↑HbA2 (>3.5%), ↑HbF Severe Form Hydrops fetalis (--/--) Major (Cooley's Anemia - β0/β0) - Clinical: Microcytic hypochromic anemia (↓MCV, ↓MCH), jaundice, splenomegaly, iron overload. "Crew-cut" skull X-ray (β-Major).
- Diagnosis: CBC, peripheral smear (target cells, anisopoikilocytosis); Hb electrophoresis/HPLC.
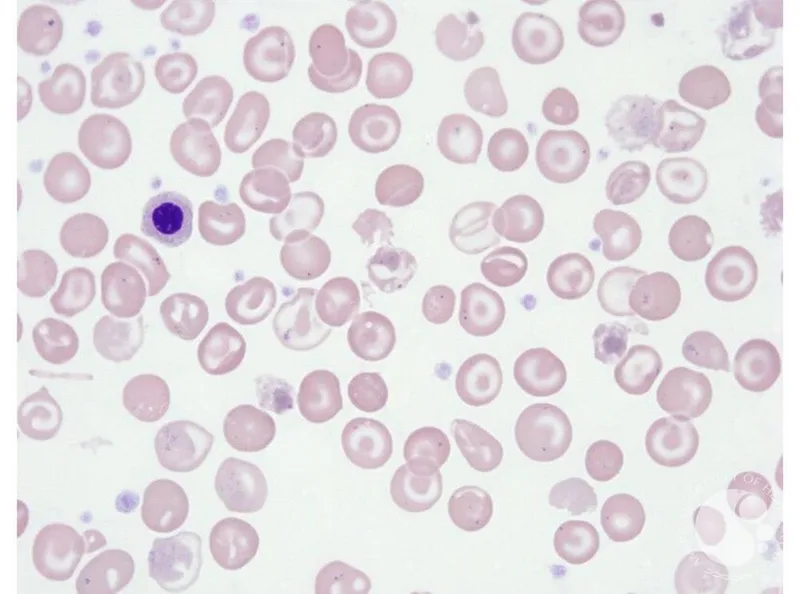
⭐ In β-Thalassemia Major, extramedullary hematopoiesis can lead to characteristic bone deformities like "crew-cut" skull on X-ray and hepatosplenomegaly due to ineffective erythropoiesis.
Hb Variants: The Odd Bunch
| Feature | HbC Disease | HbE Disease/Trait | Methemoglobinemia |
|---|---|---|---|
| Defect | $Glu6Lys## Hb Variants: The Odd Bunch |
(β-globin) | $Glu26Lys## Hb Variants: The Odd Bunch
(β-globin) | Oxidized Heme (Fe³⁺) | | Key Clinical | Mild hemolytic anemia, target cells, crystals | SE Asia. Mild microcytic anemia, target cells | Cyanosis, chocolate blood. Normal $PaO_2## Hb Variants: The Odd Bunch
|
| Treatment | Supportive | Supportive | Methylene blue |* HbD-Punjab: $Glu121Gln$ (β-globin). Common in NW India (Punjab). Mild hemolysis or asymptomatic. Homozygotes similar to sickle cell trait.
⭐ Methemoglobinemia: Arterial blood remains "chocolate-brown" despite O₂ exposure; pulse oximetry unreliable (~85%).
Detective Work: Spotting Hb Issues
Initial clues for hemoglobinopathies come from basic hematology. Further specialized tests confirm the diagnosis and type.
- Screening Tests:
- CBC: RBC indices (MCV, MCH, MCHC).
- Peripheral Smear: Morphology (sickled cells, target cells, Heinz bodies, basophilic stippling).
- Confirmatory Tests:
- Hb Electrophoresis: Cellulose acetate (pH 8.6), Citrate agar (pH 6.2).
- HPLC: Quantitative & qualitative assessment.
- Specific Tests:
- Sickling Test (for HbS).
- Kleihauer-Betke Test (quantifies HbF).
- Molecular Diagnosis:
- DNA analysis: Specific mutations/deletions.
⭐ HPLC is currently the gold standard for neonatal screening and quantitative assessment of hemoglobin variants.
High‑Yield Points - ⚡ Biggest Takeaways
- Sickle Cell Anemia: β-globin gene mutation (GAG→GTG; Glu⁶→Val) forms HbS.
- HbS polymerizes under low O₂, causing sickling, vaso-occlusion, hemolysis.
- Hydroxyurea ↑ HbF, beneficial in Sickle Cell Disease.
- Thalassemias: Quantitative defect in globin synthesis; α-thalassemia (deletions), β-thalassemia (mutations).
- β-Thalassemia Major: Severe anemia, ineffective erythropoiesis; requires transfusions, iron chelation.
- ↑ HbA2 in β-thalassemia trait; ↑ HbF in severe β-thalassemias.
- Hb Bart's (γ₄) in α-thalassemia major (hydrops fetalis); HbH (β₄) in HbH disease.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

