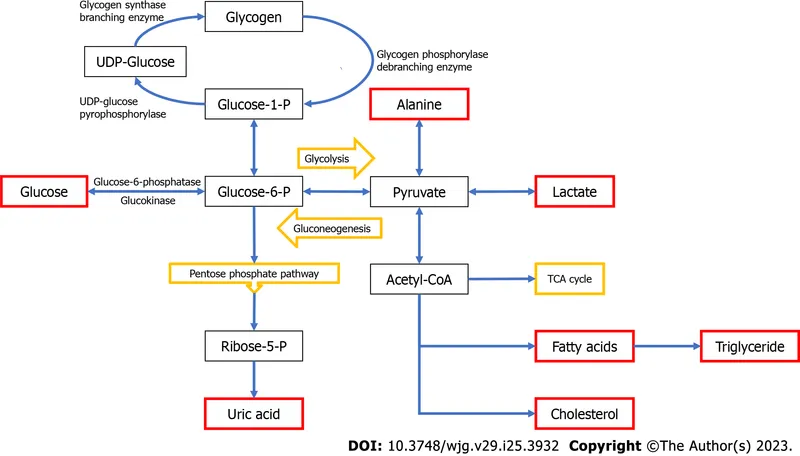
GSDs Overview - Glycogen's Glitches
- Glycogen Storage Diseases (GSDs): Group of inherited metabolic disorders.
- Caused by enzyme defects in glycogen synthesis or breakdown pathways.
- Result: Abnormal glycogen quantity or quality in tissues.
- Clinical impact: Primarily liver (e.g., hepatomegaly, hypoglycemia) and/or muscle (e.g., weakness, exercise intolerance).
- Classified broadly:
- Hepatic forms
- Myopathic forms
- Mixed (affecting multiple tissues)
⭐ Most Glycogen Storage Diseases are inherited in an autosomal recessive manner, except for GSD Type IX (Phosphorylase Kinase Deficiency) which can be X-linked.
Type I GSD (Von Gierke) - Sugar Stuck Starver
- Autosomal recessive; Glucose-6-Phosphatase deficiency. Gene: G6PC.
- 📌 Von Gierke's: Heavy Hepato-Renomegaly, Hypoglycemia, Hyperlipidemia, Hyperuricemia, Lactic Acidosis.
- Key Features: Severe fasting hypoglycemia (by 3-6 months), lactic acidosis, hyperuricemia, hyperlipidemia.
- Massive hepatomegaly, renomegaly.
- Doll-like facies, growth retardation.
- Normal glycogen structure.
- Dx: ↓ glucose, ↑ lactate, ↑ uric acid, ↑ lipids. Glucagon test: no glucose response, ↑ lactate. Enzyme assay/genetic test.
- Rx: Frequent feeds, uncooked cornstarch. Avoid fructose, galactose.
⭐ Von Gierke's disease (GSD Type Ia) is due to Glucose-6-Phosphatase deficiency, leading to severe fasting hypoglycemia, lactic acidosis, hyperuricemia, and hyperlipidemia.
Key GSDs Compared - Defect Lineup
| GSD Type (Name) | Defective Enzyme | Key Features / Affected Organs | Mnemonic 📌 |
|---|---|---|---|
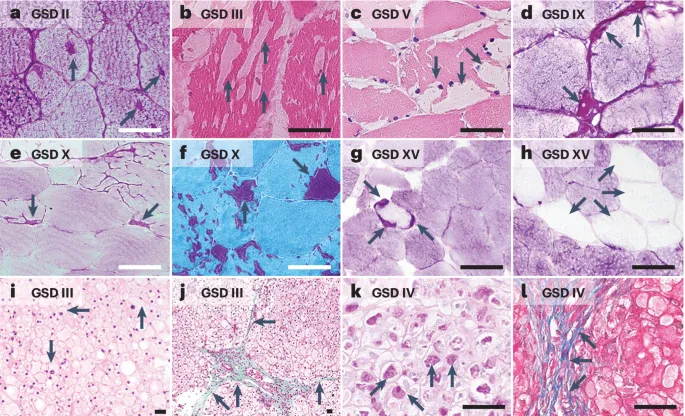
| II (Pompe) | Lysosomal α-1,4-glucosidase (acid maltase) | Massive cardiomegaly, profound hypotonia, hepatomegaly; lysosomal glycogen accumulation. Affects all organs. | Pompe affects the Pump (heart) |
| III (Cori/Forbes) | Debranching enzyme (amylo-1,6-glucosidase) | Hepatomegaly, fasting hypoglycemia, muscle weakness, hypotonia; normal lactate. Limit dextrinosis. | Cori = Can't Debranch |
| IV (Andersen) | Branching enzyme (amylo-1,4→1,6 transglucosidase) | Progressive hepatosplenomegaly, cirrhosis, failure to thrive; abnormal glycogen (amylopectin-like). | Andersen = Abnormal Branches |
| V (McArdle) | Muscle glycogen phosphorylase | Exercise intolerance, painful cramps, myoglobinuria (rhabdomyolysis) post-exercise; "second wind". Muscle. | McArdle = Muscle |
GSD Workup & Care - Glycogen Guide
- Management Goals:
- Maintain euglycemia (avoid fasting, frequent feeds/cornstarch).
- Support growth & development.
- Manage type-specific complications (e.g., GSD I: gout, renal).
- ERT for GSD II (Pompe).
- Genetic counseling.
⭐ Diagnosis of GSDs often involves a combination of clinical presentation, biochemical tests (blood glucose, lactate, CK), specific enzyme assays on tissue biopsy (liver, muscle) or blood cells, and molecular genetic testing.
High‑Yield Points - ⚡ Biggest Takeaways
- Von Gierke (I): G6Pase def.; severe fasting hypoglycemia, lactic acidosis, hepatomegaly, hyperuricemia.
- Pompe (II): Lysosomal α-1,4-glucosidase def.; cardiomegaly, hypotonia, macroglossia; "Pompe trashes the Pump".
- Cori (III): Debranching enzyme def.; milder Type I, normal lactate, gluconeogenesis intact.
- McArdle (V): Muscle glycogen phosphorylase def.; exercise intolerance, muscle cramps, myoglobinuria, second wind.
- Andersen (IV): Branching enzyme def.; cirrhosis, infantile hypotonia, abnormal glycogen.
- GSDs: Inherited enzyme defects in glycogen metabolism causing abnormal glycogen storage/usage.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more