Ethanol's Entry & ADH Action - Booze Breakdown Begins
-
Ethanol Entry & Distribution:
- Rapid absorption: Stomach (~20%), Small Intestine (~80%).
- Distributes in total body water; readily crosses Blood-Brain Barrier (BBB) & placenta.
-
ADH Pathway: The Primary Breakdown Route:
- Location: Cytosol of hepatocytes. (📌 'C' for Cytosol, 'C' for $C_2H_5OH$)
- Enzyme: Alcohol Dehydrogenase (ADH).
- Reaction: $CH_3CH_2OH + NAD^+ \xrightarrow{ADH} CH_3CHO + NADH + H^+$
- Product: Acetaldehyde ($CH_3CHO$) - highly reactive & toxic.
- Cofactor Dynamics: $NAD^+$ consumed, $NADH$ produced $\rightarrow$ ↑ $NADH/NAD^+$ ratio (key metabolic impact).
- Kinetics: Zero-order above ~10 mg/dL (or ~2 mM) ethanol.
- Metabolizes a constant amount: approx. 7-10 g/hour.

⭐ Alcohol metabolism predominantly follows zero-order kinetics at pharmacologically relevant concentrations, meaning a constant amount is processed per unit time, irrespective of blood alcohol levels above a certain threshold.
Acetaldehyde's End & MEOS Role - Toxic Takedown Time
Acetaldehyde Fate (ALDH Pathway)
- Oxidized to Acetate by Aldehyde Dehydrogenase (ALDH), mainly ALDH2.
- Location: Mitochondria (📌 'M'ighty 'M'itochondria 'M'op up Acetaldehyde).
- Reaction: $CH_3CHO + NAD^+ + H_2O \xrightarrow{ALDH} CH_3COOH + NADH + H^+$
- Product: Acetate (→ Acetyl-CoA → TCA cycle).
- ALDH2 Deficiency: Flushing, nausea (common in East Asians, due to acetaldehyde buildup).
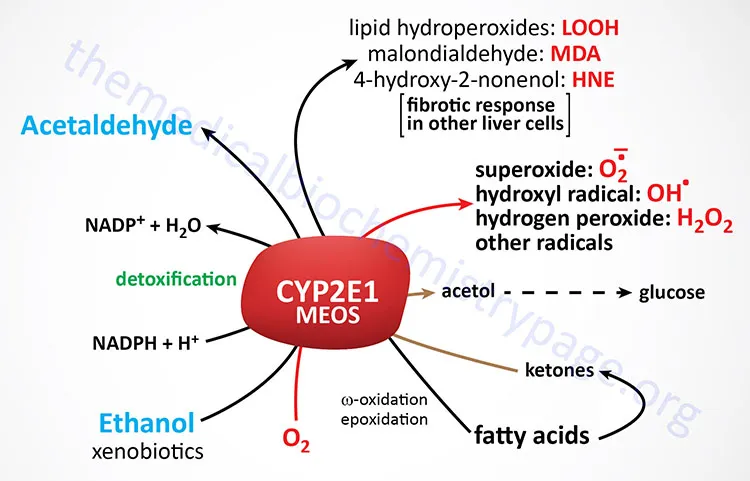
Microsomal Ethanol Oxidizing System (MEOS)
- Alternative pathway; active at high ethanol concentrations.
- Location: Smooth Endoplasmic Reticulum (SER) of liver cells.
- Key Enzyme: CYP2E1 (a Cytochrome P450 isoform).
- Reaction: $CH_3CH_2OH + NADPH + H^+ + O_2 \xrightarrow{CYP2E1} CH_3CHO + NADP^+ + 2H_2O$
- Chronic alcohol use induces CYP2E1:
- Contributes ~10-20% to overall ethanol metabolism.
- Results in:
- ↑ Alcohol tolerance.
- ↑ Acetaldehyde & Reactive Oxygen Species (ROS) → hepatotoxicity.
- Altered drug metabolism (e.g., paracetamol, leading to ↑ toxicity).
⭐ Chronic alcohol consumption induces the MEOS pathway, particularly CYP2E1, leading to increased alcohol tolerance and altered drug metabolism.
Metabolic Mayhem & Clinical Links - Clinical Chaos Chronicles
Chronic alcohol intake elevates NADH/NAD+ ratio, leading to widespread metabolic disruption. Acetaldehyde accumulation also causes significant toxicity.
Key Metabolic Derangements (due to ↑NADH/NAD+):
- 📌 Mnemonic for overall ↑NADH/NAD+ effects: 'LACTate HIKEs' (Lactic Acidosis, Hypoglycemia, Acetyl-CoA to Ketones/Fatty acids, Hyperuricemia, steatosis).
Acetaldehyde Toxicity:
- Acute: Flushing, nausea, headache (ALDH2 deficiency worsens).
- Chronic: Liver damage (fibrosis, cirrhosis), carcinogen.
Other Major Clinical Links:
- Wernicke-Korsakoff syndrome (Thiamine deficiency).
- Alcoholic Ketoacidosis (AKA).
- Fetal Alcohol Syndrome (FAS).
- Methanol/Ethylene Glycol Poisoning:
- Methanol $\rightarrow$ Formic acid (blindness).
- Ethylene Glycol $\rightarrow$ Oxalic acid (renal failure).
- Antidotes: Fomepizole, Ethanol.
- Disulfiram: Inhibits ALDH $\rightarrow$ acetaldehyde buildup (aversive).
⭐ Fomepizole is a competitive inhibitor of alcohol dehydrogenase and is the preferred antidote for methanol and ethylene glycol poisoning.

High‑Yield Points - ⚡ Biggest Takeaways
- Ethanol primarily metabolized by cytosolic ADH then mitochondrial ALDH.
- ADH is the rate-limiting enzyme in this pathway.
- MEOS (CYP2E1) is an inducible system, important at high alcohol concentrations.
- Acetaldehyde is toxic, causing flushing, nausea, and organ damage.
- Disulfiram inhibits ALDH, leading to acetaldehyde accumulation and severe symptoms.
- ↑ NADH/NAD+ ratio from alcohol metabolism causes lactic acidosis, hypoglycemia, fatty liver.
- Fomepizole (ADH inhibitor) or ethanol treats methanol/ethylene glycol poisoning.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

