Non-opioids: Intro & MOA - The Pain Tamers
- Definition: Diverse drug group for mild-moderate pain & fever; some possess significant anti-inflammatory effects (e.g., NSAIDs). Not structurally related to opioids, generally fewer side effects like dependence.
- Key Classes:
- NSAIDs (e.g., Ibuprofen, Diclofenac)
- Paracetamol (Acetaminophen) - analgesic, antipyretic, weak anti-inflammatory.
- Others (e.g., Nefopam - centrally acting, non-opioid).
- NSAID MOA - Primary Action:
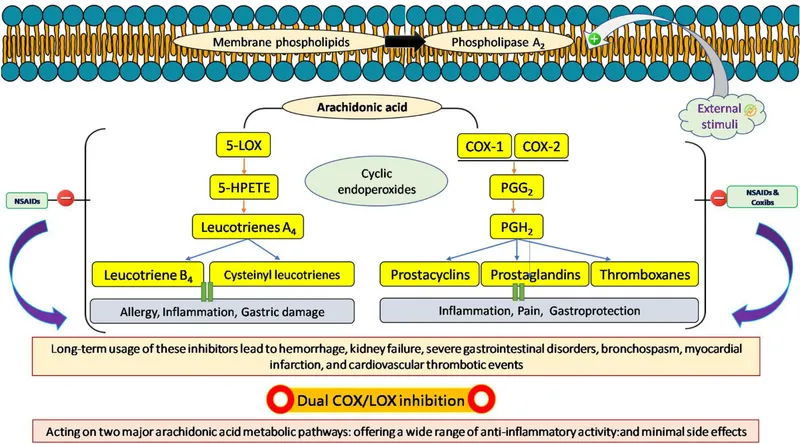
- Inhibit cyclooxygenase (COX) enzymes (isoforms COX-1 & COX-2).
- This blocks conversion of arachidonic acid (released by phospholipase A2) to prostaglandins (PGs), prostacyclin (PGI2), & thromboxane A2 (TXA2).
- PGs: Key mediators of pain, inflammation, fever.
- 📌 Mnemonic: "NSAIDs knock out COX, PGs can't box!"
⭐ Most NSAIDs non-selectively inhibit COX-1 & COX-2, yielding therapeutic effects but also side effects (e.g., gastric issues via COX-1 inhibition).

NSAIDs: Types & ADRs - COX & Effects
- COX Enzymes & Effects:
- COX-1 (Constitutive): GI protection (PGE2/PGI2), Platelet aggregation (TXA2), Renal function.
- COX-2 (Inducible/Constitutive): Inflammation, Pain, Fever. Also renal function, PGI2 (vasodilation, anti-platelet) in endothelium.
- NSAID Classes & Comparative ADRs:
| Class | Examples | Key ADRs (Relative Risk) |
|---|---|---|
| Non-selective | Ibuprofen, Aspirin, Diclofenac | GI: High (ulcers, bleed). Renal: AKI. CV: ↑BP, thrombotic risk (Aspirin cardioprotective at low dose). Antiplatelet effect. |
| Preferential COX-2 | Nimesulide, Meloxicam | GI: Moderate. Renal/CV: Similar to non-selective. |
| Selective COX-2 (Coxibs) | Celecoxib, Etoricoxib | GI: Lower. Renal: Similar. CV: ↑↑ Thrombotic risk (MI, stroke). No antiplatelet effect. ⚠️ Sulfa allergy (Celecoxib). |
* **GI:** ↓Protective PGs.
* **Renal:** ↓PGs → ↓RBF, Na+/H2O retention.
* **CV (Coxibs/Non-Aspirin NSAIDs):** Unopposed TXA2 or ↓PGI2 → prothrombotic.
* **AERD:** Leukotriene overproduction.
⭐ Aspirin: Irreversible COX-1 inhibition in platelets (antiplatelet effect for 7-10 days). Low dose (75-150 mg) for cardioprotection.
📌 COX-1 = Gut, Renal, Platelets (GRP). COX-2 = Inflammation, Pain, Fever (IPF).
Paracetamol: The Go-To - Beyond NSAIDs
- Mechanism: Weak COX inhibitor (mainly central); possible effects on COX-3, serotonergic pathways. Analgesic, antipyretic.
- ⚠️ No significant anti-inflammatory effect.
- Dosing:
- Adults: 0.5-1g QDS (max 4g/day).
- Pediatrics: 10-15 mg/kg/dose.
- Hepatotoxicity:
- Toxic metabolite: NAPQI (N-acetyl-p-benzoquinone imine) via CYP450 (mainly CYP2E1).
- Overdose depletes glutathione → NAPQI damages hepatocytes.
- Toxic dose (acute): >150 mg/kg or >7.5-10g.
- Risk factors: Chronic alcohol, malnutrition, enzyme inducers (e.g., rifampicin, isoniazid).
- Antidote: N-acetylcysteine (NAC).
- Replenishes glutathione, directly detoxifies NAPQI.
- Best if given within 8-10 hours post-ingestion.
⭐ Rumack-Matthew nomogram guides NAC therapy based on serum paracetamol levels vs. time post-ingestion.

Paracetamol Poisoning Management Flowchart:
Clinical Use: Smart Choices - Pick Wisely
Choose non-opioids by pain type, severity, patient risks. Paracetamol is cornerstone if NSAIDs risky.
- Paracetamol: Max dose 4g/day (adults). In severe hepatic impairment, limit to <2g/day.
- NSAIDs: Use lowest effective dose, shortest duration. ⚠️ AVOID if GFR <30 mL/min, active PUD, or 3rd trimester pregnancy.
- ⚠️ Interactions: NSAIDs with anticoagulants (↑bleeding); +ACEi/ARBs/diuretics (↑renal toxicity).
⭐ For osteoarthritis in elderly, paracetamol is first-line over NSAIDs due to better safety, despite weaker anti-inflammatory effects.
High‑Yield Points - ⚡ Biggest Takeaways
- Paracetamol: Central COX inhibition; hepatotoxicity (NAPQI) reversed by N-acetylcysteine; max 4g/day.
- NSAIDs: COX-1 & COX-2 inhibition; risks: GIT ulcers, renal impairment, bronchospasm.
- Selective COX-2 inhibitors: ↓ GIT side effects, but ↑ cardiovascular thrombotic risk (e.g., Etoricoxib).
- Nefopam: Centrally acting non-opioid; inhibits monoamine reuptake; causes tachycardia, sweating.
- Low-dose Ketamine: NMDA antagonist; potent analgesic for neuropathic pain, opioid-sparing.
- Gabapentinoids: Target α2δ Ca2+ channel subunit; first-line for neuropathic pain.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

