VHD Overview & Pre-op Assessment - Valve Check Central
- Types: Stenosis (obstructed flow, e.g., AS, MS) & Regurgitation (leaky valve, e.g., AR, MR).
- Severity (Echo):
- Valve Area: Severe AS < 1.0 cm², Severe MS < 1.0 cm².
- Gradients (stenosis), Regurgitant Fraction/Volume (regurgitation).
- Symptoms: NYHA Class I-IV functional status.
- Pre-op Basics:
- ECG, CXR, Labs (CBC, Coagulation, RFT, LFT).
- Echocardiography: Key for diagnosis, severity, LV/RV function.
- IE Prophylaxis: High-risk pts (prosthetic valve, prior IE, specific CHD) for dental procedures involving gingival manipulation. Amoxicillin 2g PO. 📌 VHD Severity: Mild, Moderate, Severe.
⭐ Echocardiography is the cornerstone for diagnosis, severity assessment, and LV/RV function in VHD, guiding perioperative management.
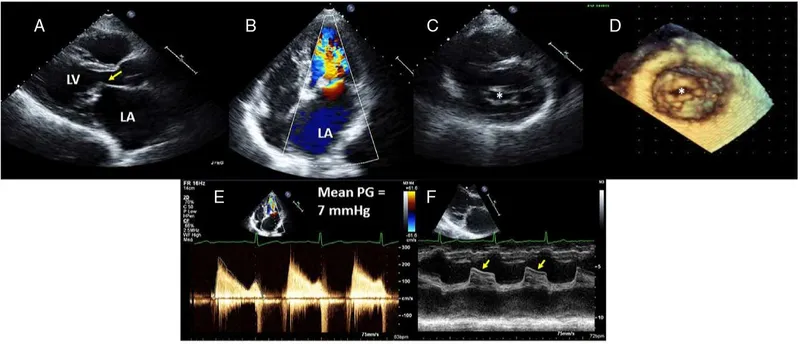
Aortic Stenosis - The Squeeze Play
📌 AS Triad: SAD (Syncope, Angina, Dyspnea). 📌 Anesthesia: 'Keep it Slow, Sinus, Supported (SVR)'.
- Pathophysiology:
- Left Ventricular Hypertrophy (LVH) from ↑ afterload; fixed Cardiac Output (CO).
- Critical AS: valve area < 0.6 cm².
- Hemodynamic Goals:
- Normal Sinus Rhythm (NSR): HR < 90 bpm (avoid tachycardia).
- Preload: Maintain adequate preload.
- Afterload: Maintain Systemic Vascular Resistance (SVR) & arterial pressure (SBP > 100 mmHg).
- Contractility: Support if needed.
- Anesthetic Choice:
- General Anesthesia (GA) preferred.
- Avoid significant ↓ SVR (careful with neuraxial, especially spinal).
- Vasopressors (e.g., phenylephrine) readily available.
- Invasive monitoring often indicated.
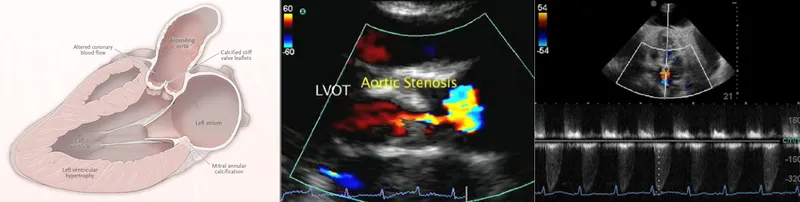
⭐ In severe Aortic Stenosis, maintaining afterload is critical; avoid spinal anesthesia due to risk of sudden hypotension and cardiovascular collapse.
Mitral Stenosis - Atrial Traffic Jam
- Pathophysiology: Obstructed LV inflow → LA pressure ↑ → LA enlargement, Atrial Fibrillation (AF) risk. Leads to pulmonary venous congestion & Pulmonary Hypertension (PHT: $mPAP$ > 20 mmHg). Severe MS: Valve area < 1.0 cm².
- Hemodynamic Goals: "Full, Slow, Constricted"
- Heart Rate: Slow (50-70 bpm) for diastolic filling. 📌 MS: 'Keep HR Low, LA pressure down.'
- Preload: Maintain/↑.
- Afterload: Maintain/↑.
- PVR: Avoid ↑ (hypoxia, hypercarbia).
- Anesthesia: Manage AF (rate control, cardioversion). Avoid drugs ↑ PVR (Ketamine in severe PHT, N2O with caution).
⭐ Tachycardia dramatically reduces diastolic filling time and increases left atrial pressure in Mitral Stenosis, potentially precipitating pulmonary edema.
Regurgitant Lesions - Leaky Pipes Patrol
- Pathophysiology & Key Features:
- Aortic Regurgitation (AR): Diastolic leak from aorta to LV → LV dilatation, eccentric hypertrophy, ↑ LV end-diastolic volume.
- Mitral Regurgitation (MR): Systolic leak from LV to LA → LA & LV volume overload, LA enlargement.
- Hemodynamic Goals: 📌 'Keep it Fast, Full, Forward.'
- Fast: Maintain or slightly ↑ Heart Rate (avoid bradycardia to ↓ regurgitant time & maintain cardiac output).
- Full: Maintain Preload (adequate venous return).
- Forward: ↓ Afterload (crucial to promote forward flow, reduce regurgitant fraction).
- Anesthetic Considerations:
- Emphasize afterload reduction: vasodilators (e.g., sodium nitroprusside, nitroglycerin).
- Inotropes (e.g., dobutamine, milrinone) if EF is compromised.
- Avoid myocardial depressants and bradycardia.
- Regional anesthesia with sympathectomy can be beneficial (reduces afterload).
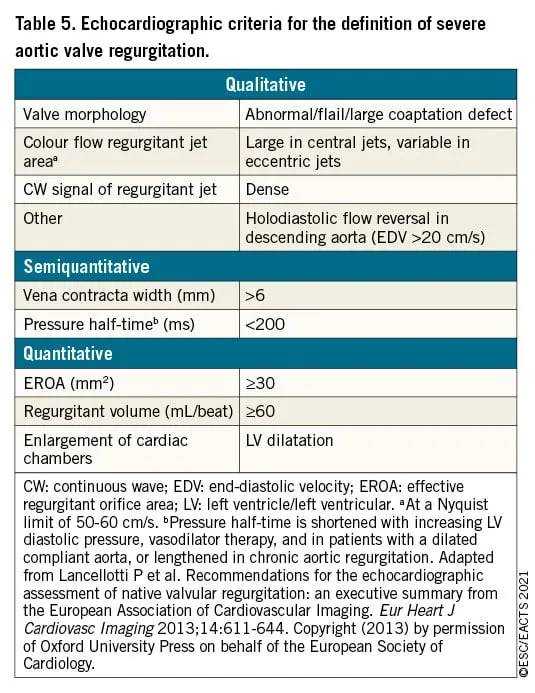
- Severity Thresholds (Examples):
- Severe AR: Regurgitant Volume >60mL/beat; Regurgitant Fraction >50%.
- Severe MR: Regurgitant Volume >60mL/beat; Regurgitant Fraction >50%.
⭐ The primary hemodynamic goal for severe Aortic or Mitral Regurgitation is afterload reduction to promote forward cardiac output and reduce regurgitant volume.
High‑Yield Points - ⚡ Biggest Takeaways
- Aortic Stenosis (AS): Slow, Sinus, Full. Avoid hypotension, tachycardia. Phenylephrine for pressure.
- Aortic Regurgitation (AR): Fast, Full, Forward. Avoid bradycardia, ↑ SVR. Inotropes, vasodilators useful.
- Mitral Stenosis (MS): Slow, Sinus, Full (cautious). Avoid tachycardia, pulmonary HTN triggers.
- Mitral Regurgitation (MR): Fast, Full, Forward. Maintain forward flow; avoid ↑ SVR, bradycardia.
- HOCM: Maintain preload, afterload. Avoid hypovolemia, tachycardia, vasodilation, ↑ contractility.
- TEE: Crucial intraop monitor for valvular surgery, guiding repair & assessing hemodynamics.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

