Preoperative Assessment - Vascular Vitals
- Immediate Assessment (ABCDE): Prioritize Circulation. Secure airway (RSI often needed due to full stomach risk), ensure oxygenation/ventilation.
- History (AMPLE): If patient condition allows; focus on anticoagulants, allergies, last meal.
- Key Investigations:
- Stat Labs: Crossmatch (minimum 4-6 units), FBC, comprehensive coagulation screen (PT/INR, aPTT, fibrinogen, TEG/ROTEM if available).
- Imaging: FAST scan for AAA rupture/trauma; CT Angio if stable enough.
- Risk Stratification:
- ASA status (often ASA IV/V E).
- Cardiac: RCRI. Urgency: Emergent.
- Hemodynamic Goals & Resuscitation:
- Large-bore IV access (2 x 14-16G).
- Ruptured AAA: Permissive hypotension (SBP 80-90 mmHg) until proximal control. Avoid aggressive crystalloid resuscitation.
- MTP Activation: Anticipate massive blood loss. 📌 MTP: PRBC:FFP:Platelets 1:1:1.
- Consent: Implied consent for life-saving surgery if patient unconscious/incapacitated.
⭐ The lethal triad in trauma (acidosis, hypothermia, coagulopathy) is highly relevant in ruptured AAA.
Specific Emergencies - Rupture & Race
| Emergency | Patho Highlights | Classic Presentation | Anesthetic Goals | Monitoring Nuances |
|---|---|---|---|---|
| rAAA | Atherosclerosis, wall weak | Hypotension, pulsatile mass, pain (triad) | Permissive SBP 80-100 mmHg pre-clamp, RSI, MTP, 2x large IVs. | A-line pre-induction, CVC, TEE. |
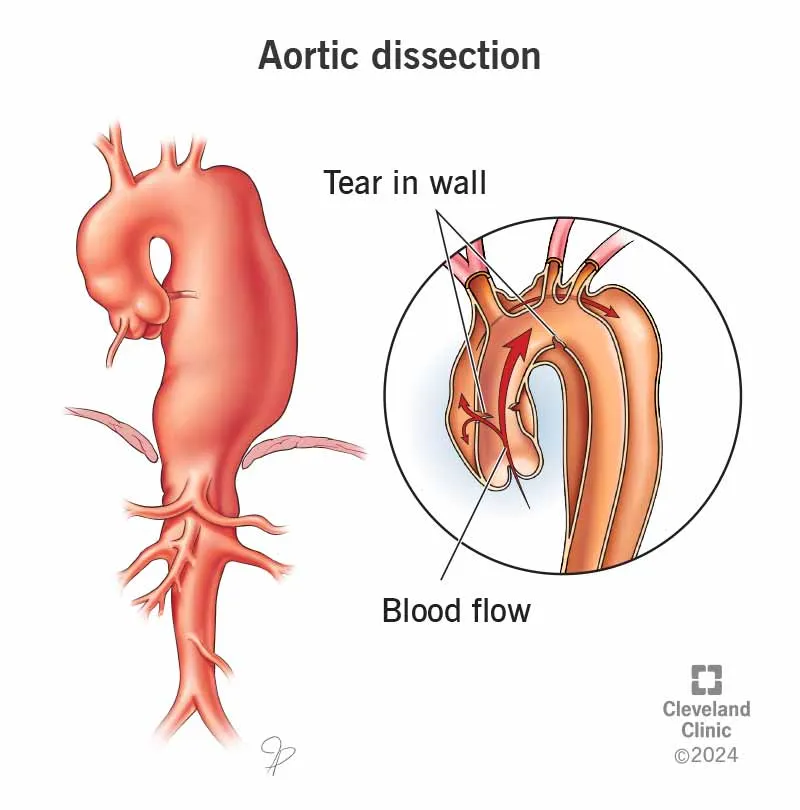
| Acute Aortic Dissection | Intimal tear, false lumen. 📌 Stanford/DeBakey | Tearing chest/back pain, pulse deficits | Type A: SBP 100-120 mmHg, HR <60 bpm. Type B: Similar goals. | Bilateral A-lines, CVC, TEE. |
| Acute Limb Ischemia | Embolus/thrombus | 6 P's (Pain, Pallor, Pulselessness, etc.) | Manage reperfusion injury (↑K+, acidosis), heparin (ACT 250-300s). | A-line, NIRS. |
| Carotid Blowout | Post-Rx/surgery, tumor erosion | Sentinel bleed, active neck hemorrhage | Secure airway (difficult!), volume resuscitation, BP control (balance bleeding/cerebral perfusion). | A-line, large IVs. |
Intraoperative Management - OR Balancing Act
- Monitoring & Access:
- Invasive: Arterial line (BP, ABGs), CVC (access, CVP); PA catheter (severe cardiac dysfunction).
- IV Access: ≥2 large-bore (14-16G) or rapid infusion catheter.
- Fluid & Blood Management:
- Permissive Hypotension: SBP 80-90 mmHg (pre-control in rAAA).
- MTP:
- Activate early.
- Ratio 1:1:1 (PRBC:FFP:Platelets).
- Warm products.
- Cell salvage: Use if appropriate.
- TXA: 1g IV load, then 1g/8h (within 3h injury).
- Anesthetic Techniques:
- Standard: GA with RSI.
- Induction: Etomidate/Ketamine (hemodynamic stability).
- Maintenance: Volatile or TIVA.
- Regional: Usually contraindicated (unstable, coagulopathy).
- Vasopressors/Inotropes:
- Noradrenaline (first-line). Vasopressin (adjunct for refractory shock).
- Inotropes for myocardial dysfunction.
- Special: One-Lung Ventilation (OLV):
- If thoracic aorta involved (e.g., TAAA repair).
⭐ Goal-directed fluid therapy using dynamic parameters (e.g., SVV, PPV) is preferred over static pressure monitoring in managing major hemorrhage.
Postoperative Care - Aftermath Alert
- Immediate ICU Transfer & Continued Resuscitation: Vital for ongoing stabilization.
- Pain Management: Multimodal approach.
- Opioids, regional techniques (if suitable post-op).
- Paracetamol, NSAIDs (use cautiously).
- Complication Monitoring: Vigilance is key.
-
Reperfusion Injury: Hyperkalemia, acidosis, rhabdomyolysis.
-
Abdominal Compartment Syndrome (ACS): Bladder pressure >20 mmHg with organ dysfunction.
-
Acute Kidney Injury (AKI).
-
Myocardial Infarction, Stroke.
-
Limb ischemia (post-revascularization).
-
- Ventilatory Support & Weaning: As clinically indicated.
⭐ Monitoring for abdominal compartment syndrome is crucial after ruptured Abdominal Aortic Aneurysm (rAAA) repair, especially with massive fluid resuscitation.
High‑Yield Points - ⚡ Biggest Takeaways
- Rapid Sequence Intubation (RSI) is crucial for aspiration risk in emergencies like ruptured AAA.
- Permissive hypotension pre-clamp for ruptured AAA; manage hypertension post-clamp.
- Essential: Large-bore IVs, arterial line for monitoring and massive transfusion readiness.
- Aortic cross-clamping: abrupt ↑afterload/BP. Declamping: ↓SVR, hypotension, metabolic washout.
- Prioritize goal-directed fluid/blood product resuscitation (often 1:1:1 ratio).
- Maintain normothermia; monitor for renal injury and coagulopathy.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

