Placentation: Genesis - Conception's Cradle
Placentation is the formation, growth, and organization of the placenta, commencing shortly after fertilization.
- Early Development (Week 1):
- Fertilization → Zygote → Morula (approx. day 3-4) → Blastocyst (approx. day 5).
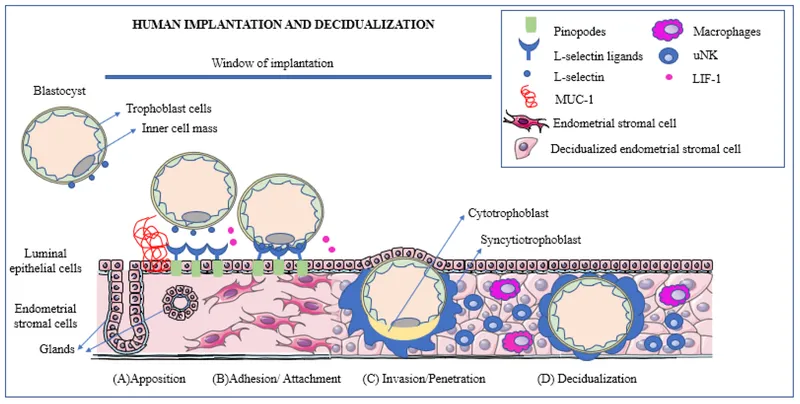
- Blastocyst components: Inner cell mass (embryoblast) and outer cell mass (trophoblast).
- Implantation (Days 6-10):
- Blastocyst adheres to and invades the uterine endometrium (decidua).
- Usual site: Posterior superior uterine wall.
- Trophoblast Differentiation (from Day 7-8):
- Cytotrophoblast: Inner layer, mitotically active cells.
- Syncytiotrophoblast: Outer, multinucleated syncytium; invasive, erodes maternal tissues.
- Responsible for hormone production, notably human Chorionic Gonadotropin (hCG).
⭐ Syncytiotrophoblast is responsible for hCG production, detectable in maternal blood around day 8-9 post-fertilization.
Placentation: Villous Voyage - Branching Wonders
- Chorionic Villi Development: Functional units of the placenta.
- Primary Villi (Day 11-13): Cytotrophoblast core, syncytiotrophoblast outer layer.
- Secondary Villi (Day 16): Extraembryonic mesoderm invades primary villi.
- Tertiary Villi (Day 21): Blood vessels develop within mesoderm; forms fetal part of placenta (chorion frondosum).
- Maternal Component: Decidua basalis (from endometrium).
- Fetal Component: Chorion frondosum (bushy chorion). Smooth chorion (chorion laeve) is avascular.
- Anchoring Villi: Attach chorionic plate to decidua basalis.
- Branching (Free) Villi: Site of main exchange.
⭐ Hofbauer cells, found in the stroma of chorionic villi, are placental macrophages of fetal origin involved in immune defense and villous remodeling.

Placentation: Circulation Central - The Exchange Express
- Structure: Mature placenta: fetal chorionic plate, maternal basal plate. Intervillous space (IVS) contains maternal blood.
- Maternal Flow: Spiral arteries → IVS (bathes villi) → endometrial veins.
- Driven by pressure gradient (approx. 70 mmHg uterine artery to 10 mmHg IVS).
- Fetal Flow: 2 Umbilical arteries (deoxygenated blood from fetus) → villous capillaries → 1 Umbilical vein (oxygenated blood to fetus).
- Placental Barrier: Separates maternal & fetal blood. Layers: syncytiotrophoblast, cytotrophoblast (prominent early, then reduces), villous stroma, fetal capillary endothelium. Thins with gestation to ↑ exchange efficiency.
⭐ Nitabuch's layer, a zone of fibrinoid degeneration at the materno-fetal junction, is believed to limit trophoblastic invasion into the myometrium.
- Key Exchange: O₂, CO₂, nutrients (glucose via facilitated diffusion), waste products, maternal IgG.

Placentation: Placental Powerhouse - Function Fiesta
- Respiration: O₂ delivery to fetus & CO₂ removal (simple diffusion).
- Nutrition: Transports glucose (facilitated), amino acids; transfers fatty acids, vitamins, minerals.
- Excretion: Removes fetal metabolic wastes (urea, uric acid, bilirubin).
- Endocrine Synthesis: Produces key hormones:
- hCG: Maintains corpus luteum early pregnancy.
- Progesterone: Maintains pregnancy; uterine quiescence.
- Estrogens (Estriol): Uterine growth, mammary development.
- hPL (Human Placental Lactogen):
⭐ Human Placental Lactogen (hPL) promotes fetal growth by altering maternal glucose metabolism and stimulating insulin resistance.
- Relaxin: Cervical softening, ligament relaxation.
- Protection & Immunity: Transfers maternal IgG (passive immunity); selective barrier.
High‑Yield Points - ⚡ Biggest Takeaways
- Implantation typically occurs on the posterior superior uterine wall.
- Decidual reaction: endometrial changes crucial for placentation and limiting invasion.
- Chorionic villi: functional units; tertiary villi contain fetal capillaries by week 3.
- Cytotrophoblast shell anchors placenta to decidua basalis, formed by proliferating cytotrophoblasts.
- Hofbauer cells are placental macrophages of fetal origin.
- Nitabuch's layer: fibrinoid layer at materno-fetal junction, prevents excessive trophoblast invasion.
- Spiral artery remodeling by extravillous trophoblasts is key for adequate uteroplacental perfusion.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

