Initial Steps - The Grand Unveiling
-
Incisions: Primary access to body cavities.
- I-shaped: Midline, xiphisternum to pubis. Most common.
- Y-shaped: Bilateral subclavicular to xiphisternum, then midline. For neck organ exposure.
- Modified Y-shaped: Extends to acromion processes.
-
Cavity Opening Order: Usually abdomen → thorax → cranium.
-
Fluid Collection: Before organ disturbance.
- Pleural, pericardial, peritoneal fluids: Note volume, appearance. Samples for analysis.
-
Evisceration Techniques: Systematic organ removal.
Technique Method Key Feature Virchow Organs removed individually 📌 V for Very slow, one by one Rokitansky In-situ dissection, then en-masse/block removal Widely used Ghon En-bloc removal (cervical, thoracic, abdominal) Organ systems preserved Letulle En-masse removal of all organs All organs together
- Professional Discretion: The decision to perform autopsy and specific techniques used is dictated by BNSS guidelines, local protocols, and professional discretion to protect public interest and address legal, public health, and safety issues under the BNS framework.
⭐ Rokitansky method involves in-situ dissection and is commonly practiced in India for medico-legal autopsies under BNSS procedures due to its thoroughness and ability to maintain organ relationships initially while meeting BNS evidentiary requirements.
Thoracic Cavity - Heart & Lungs Check
- Heart:
- Weight: M 300-350g, F 250-300g. Pericardial sac: fluid (<50ml), adhesions.
- Chambers, valves: hypertrophy, dilatation, vegetations, stenosis.
- Coronaries: atherosclerosis (% stenosis), thrombosis. Myocardium: infarcts, scars, hypertrophy.
- Dissection: Inflow-outflow, short-axis.
⭐ Lines of Zahn in thrombus indicate ante-mortem formation.
- Lungs:
- Weights: R ~450g, L ~375g. Pleura: adhesions, effusions (nature, volume).
- Parenchyma: congestion, edema, consolidation, emphysema, masses. Pulmonary arteries: emboli.
- Bronchi: contents, mucosa. Hilar nodes: examine.
- Thymus & Great Vessels:
- Thymus: prominent (children), atrophy (adults).
- Great vessels (Aorta, Pulm. Artery): atherosclerosis, aneurysms, dissection.
Abdomino-Pelvic Scan - Gut & Glands Tour
-
In-situ & ex-vivo exam. Note organ relations, adhesions.
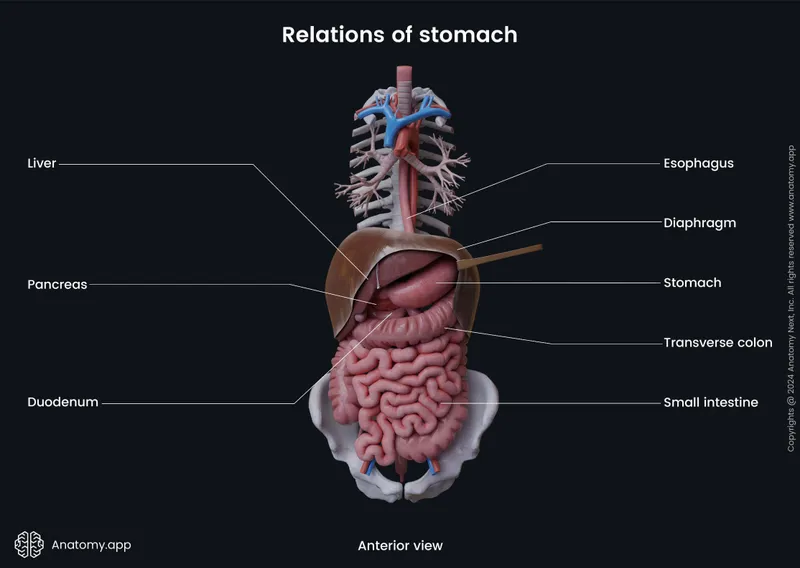
-
Liver: Wt: 1200-1600g. Capsule (Glisson's), cut surface, gallbladder (wall, stones, bile).
⭐ Rokitansky-Aschoff sinuses (gallbladder wall) = chronic cholecystitis.
-
Spleen: Wt: ~150g. Capsule, consistency, cut surface.
-
Pancreas: Retroperitoneal. Consistency, hemorrhage, necrosis.
-
Kidneys: Wt: ~150g each. Capsule. Cut: cortex, medulla, pelvicalyceal system (dilation, stones).
-
Adrenals: Cortex & Medulla. Note size, hemorrhage.
-
GIT:
- Stomach: Contents, rugae, mucosa (ulcers, erosions).
- Intestines: Contents, mucosa (ulcers, polyps). Appendix.
-
Urinary Bladder: Urine (vol, appearance), mucosa.
-
Pelvic Organs:
- Female: Uterus, Ovaries (cysts, corpora lutea), Tubes.
- Male: Prostate (size, consistency), Seminal vesicles. 📌 Retroperitoneal: SAD PUCKER (Adrenals, Aorta/IVC, Duodenum (2,3), Pancreas (not tail), Ureters, Colon (A/D), Kidneys, Esophagus, Rectum).
Cranial Vault - Brain & CNS Insights
- Scalp Reflection & Skull Removal:
- Scalp: Coronal incision (ear-to-ear), reflect anteriorly & posteriorly.
- Skull Cap: Circumferential saw lines; avoid deep dural penetration.
- Meninges Examination:
- Dura Mater: Examine for epidural/subdural hematomas, infection.
- Leptomeninges (Pia-Arachnoid): Check for subarachnoid hemorrhage, meningitis (exudates).
- Brain Examination:
- Weight: Normal Adult M: ~1350g; F: ~1250g.
- External: Inspect gyri, sulci, symmetry, signs of herniation (uncal, tonsillar).
- Slicing Methods:
- Virchow's: Serial transverse sections, posterior to anterior.
- Coronal: Slices perpendicular to brain's long axis.

- Internal Structures: Ventricular system (size, contents), basal ganglia, thalamus, brainstem, cerebellum.
⭐ Duret hemorrhages (small bleeds in pons/midbrain) are a key indicator of transtentorial herniation, often due to markedly increased intracranial pressure (↑ICP).
- Pituitary Gland: Examine in sella turcica after brain removal.
- Spinal Cord: Examine if trauma or specific neurological deficits are suspected pre-mortem (requires separate procedure).
High‑Yield Points - ⚡ Biggest Takeaways
- Dissection methods: Modern forensic autopsies employ modified Rokitansky/Virchow approaches with systematic documentation per forensic standards.
- Heart blood: Multiple sites preferred (right ventricle for toxicology, peripheral blood for post-mortem redistribution analysis).
- Stomach: Note contents (quantity, nature, smell); secure with double ligatures.
- Brain: 10% formalin fixation with adequate time; imaging correlation for herniation, edema.
- Lungs: Examine for froth (drowning), edema, emboli.
- Spleen: Can be diffluent in septicemia.
- Preservatives: 10% neutral buffered formalin for histology; specific collection methods for toxicology.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

