Skeletal Foundations - Bone Blueprint Basics
- Bone: Dynamic, mineralized connective tissue; provides structure, protection, mineral storage.
- Composition:
- Organic (~30%): Collagen (Type I) → flexibility, tensile strength.
- Inorganic (~70%): Calcium hydroxyapatite → rigidity, compressive strength.
- Bone Cells:
- Osteoblasts: Build bone (ossification). 📌 (B for Build)
- Osteocytes: Mature cells, maintain matrix, mechanosensors.
- Osteoclasts: Carve/resorb bone. 📌 (C for Carve)
- Structure: Compact (cortical) & Spongy (cancellous/trabecular) bone.
- Types: Long (femur), Short (carpals), Flat (skull), Irregular (vertebrae), Sesamoid (patella).
- Parts of Long Bone: Epiphysis (ends), Diaphysis (shaft), Metaphysis (growth zone).
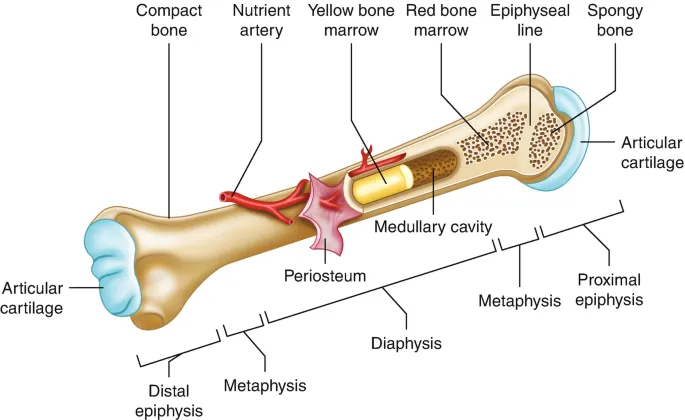
⭐ The clavicle is the first bone to ossify (intrauterine life, 5th-6th week) and the last to fuse (around 25 years).
The Skull & Teeth - Cranial Case Crackers
- Sex (Skull):
- Mastoid: Sexual dimorphism with overlap between populations
- Supraorbital Ridges: Probabilistic indicator requiring statistical analysis
- Nuchal Crest: Population-variable expression
- Frontal: General tendency with significant individual variation
- Mandible: Chin square, gonial angle <125° (M); Pointed, >125° (F) - requires comprehensive assessment
- Age (Skull):
- Suture Closure: Highly variable and unreliable for precise estimation
- Basilar Suture: Fuses 18-25 yrs.
⭐ Basilar suture fusion (18-25 yrs) is a key age marker in young adults. Other methods like pubic symphysis changes are more reliable for adult age estimation.
- Age (Teeth):
- Eruption: Sequence (Wisdom teeth 17-21 yrs).
- Modern Methods: Radiographic and biochemical techniques preferred over outdated approaches
- Demirjian's Method: Subadult dental maturity.
- Ancestry (Skull): Nasal aperture, orbital shape, prognathism - probabilistic population-specific traits requiring statistical analysis.
- ID (Teeth): Records, restorations, wear, anomalies - admissible under BSA provisions.
Pelvis & Long Bones - Pelvic Pointers & Limb Lengths
- Pelvis (Sex Determination):
- Subpubic Angle: Female >90°; Male <90°.
- Greater Sciatic Notch: Female: Wide (L-shape); Male: Narrow (J-shape).
- Pelvic Inlet: Female: Circular/Oval; Male: Heart-shaped.
- Obturator Foramen: Female: Triangular; Male: Oval.
- Sacrum: Female: Short, wide; Male: Long, narrow.
- Preauricular Sulcus: Common in females.
- 📌 Mnemonic: "Female Pelvis for Fetus: Wider, Shallower, Lighter."
- Long Bones (Stature Estimation):
- Measure max length (femur, tibia, humerus, radius, ulna).
- Apply population-specific regression formulae.
- Femur: Most accurate.
- Multiple bones: ↑ accuracy.
- Adjust for age, sex.
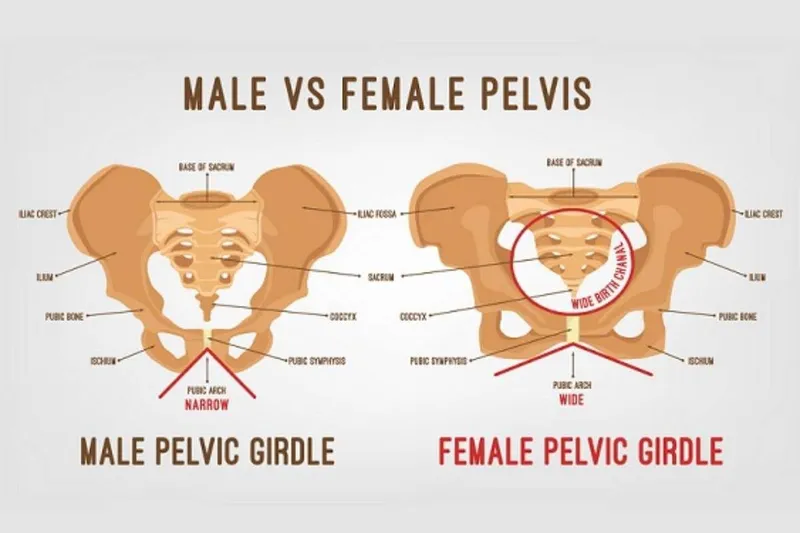
⭐ The subpubic angle is a primary indicator for sex determination from the pelvis: typically >90° in females and <90° in males.
Age & Ossification - Bony Age Almanac
- Principle: Age estimation via appearance & fusion of ossification centers.
- Primary (diaphysis): Prenatal.
- Secondary (epiphysis): Postnatal.
- Key Timelines (Approx.):
- Birth: Distal Femur, Prox. Tibia, Calcaneus, Talus, Cuboid.
- Elbow (📌CRITOE): Capitulum 1yr, R.head 3-5yrs, Int. epicondyle 5-7yrs, Trochlea 8-10yrs, Olecranon 10-12yrs, Ext. epicondyle 11-13yrs. Fusion ~2yrs earlier ♀.
- Shoulder, Hip, Knee: Fusion 16-23yrs.
- Clavicle (Medial): Fuses 22-25yrs.
- Sacrum (S1-S5): Fuses 18-25yrs.
- Xiphoid: Fuses ~40yrs.
- Factors: Sex (♀ earlier by 1-2yrs), nutrition, hormones.
- Methods: X-ray exam, CT/MRI for detailed ossification analysis, direct bone observation. Greulich-Pyle and Tanner-Whitehouse (TW) methods commonly used in forensic contexts.
⭐ The medial end of the clavicle is one of the last epiphyses to fuse, typically between 22-25 years, making it crucial for age estimation in young adults under BSA evidence requirements.
High‑Yield Points - ⚡ Biggest Takeaways
- Pelvis remains highly reliable for sex determination, but modern 3D imaging and statistical methods enhance accuracy of skull and other elements.
- Epiphyseal fusion and dental eruption with advanced CT/MRI imaging improve subadult age estimation precision.
- Multi-factorial approach using pubic symphysis, auricular surface, and histological methods for adult age estimation.
- Stature estimation requires population-specific formulae with consideration of error ranges and secular trends.
- Hyoid bone fracture suggests strangulation/hanging but absence doesn't exclude these causes.
- Adult skeleton: 206 bones (minor variations possible); children have more due to unfused parts.
- Frontal sinus patterns with advanced imaging and DNA analysis aid positive identification.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

