Bone Composition - Skeleton's Scaffolding
- Provides structural support, protection, mineral storage (Ca, P), site for hematopoiesis.
- Matrix Components:
- Organic (~30-40% "Osteoid"): Primarily Type I collagen (provides tensile strength); also proteoglycans, osteonectin, osteocalcin.
- Inorganic (~60-70%): Mainly Hydroxyapatite crystals [$Ca_{10}(PO_4)_6(OH)_2$] (provides compressive strength).
- Cellular Components:
- Osteoblasts: Synthesize osteoid (bone formation).
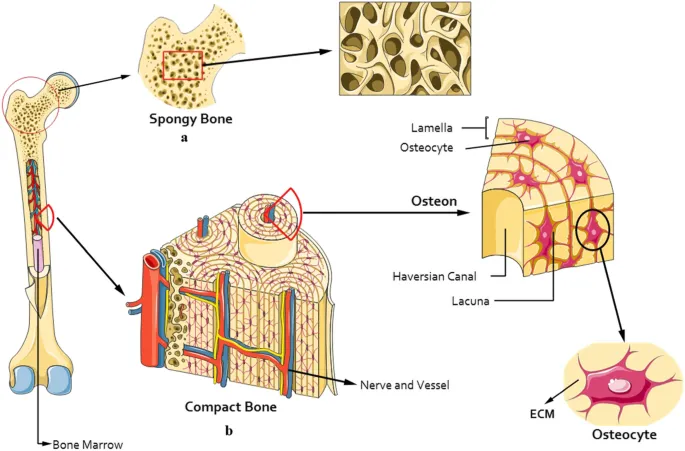
- Osteocytes: Mature cells in lacunae; mechanosensation, matrix maintenance.
- Osteoclasts: Multinucleated; bone resorption in Howship's lacunae.
- Osteoprogenitor cells: Mesenchymal stem cells; differentiate into osteoblasts.
⭐ Osteocalcin, a vitamin K-dependent protein secreted by osteoblasts, is a specific marker for bone formation and turnover.
Ossification & Growth - Blueprint to Build
Ossification: Bone formation by osteoblasts, replacing pre-existing tissue.
- Intramembranous Ossification:
- Direct bone formation from mesenchyme.
- Forms flat bones (skull, clavicle).
- Endochondral Ossification:
- Hyaline cartilage model replaced by bone.
- Forms most bones (long bones, vertebrae).
- Primary center (diaphysis), secondary (epiphyses).
Bone Growth:
- Length (Interstitial): Occurs at epiphyseal growth plates.
- Zones (epiphysis to diaphysis): Resting, Proliferation, Hypertrophy, Calcification, Ossification.
- 📌 Mnemonic (Zones): Real People Have Career Options (RPHCO).
- Width (Appositional): Periosteal osteoblasts add layers externally; osteoclasts resorb bone from medullary cavity.
Factors: Hormones (GH, TH, sex steroids), Nutrition (Vit. D, Ca, P), Mechanical stress (Wolff's Law: bone adapts to load).
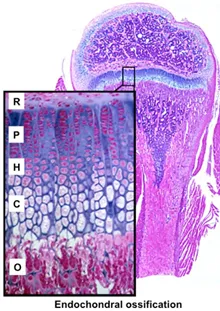
⭐ Epiphyseal fusion (closure of growth plates) indicates skeletal maturity and is critical for age estimation in subadults. Fusion sequence is generally predictable.
Skeletal Ageing - Time Tells Tales
Age estimation from skeletal remains is crucial for identification under BSA provisions. Methods vary by developmental stage, with modern forensic approaches emphasizing multiple methods in combination and advanced imaging (CT, MRI) for optimal accuracy.
- Subadults (up to ~25 years):
- Epiphyseal Fusion: Primary method with population-specific variations. Long bones, clavicle, pelvis show predictable fusion. Females generally fuse 1-2 years earlier (individual variation acknowledged).
- Dental Development: Tooth formation & eruption highly reliable.
- Adults:
- Pubic Symphysis: Surface changes (e.g., Suchey-Brooks method).
- Sternal Rib Ends: Metamorphosis (e.g., Iscan's phases).
- Cranial Sutures: High variability makes this less reliable (e.g., sagittal closes late 20s - significant variation).
- Microscopic Methods: Osteon counting, dental cementum annulation, dental pulp chamber evaluation.
⭐ The medial clavicular epiphysis, fusing around 22-25 years, is a key indicator for young adult age estimation under BSA evidence standards.
Growth Factors - Nature's Nurturers
- Systemic Hormones:
- Growth Hormone (GH): Via IGF-1; ↑ longitudinal bone growth.
- Thyroid Hormones (T3/T4): Essential for skeletal maturation. Deficiency → cretinism.
- Sex Hormones (Estrogen, Testosterone): Pubertal spurt; epiphyseal fusion. Estrogen: maintains bone density.
- Parathyroid Hormone (PTH): Regulates $Ca^{2+}$/phosphate; regulates bone remodeling.
- Calcitonin: Opposes PTH action; ↓ osteoclast activity.
- Vitamin D (Calcitriol): ↑ $Ca^{2+}$ absorption; essential for mineralization.
- Local Factors:
- Insulin-like Growth Factors (IGF-1, IGF-2): Mediate GH effects; stimulate osteoblast activity.
- Fibroblast Growth Factors (FGFs): Role in skeletal patterning.
⭐ FGFR3 gene mutation causes Achondroplasia (most common form of dwarfism).
- Bone Morphogenetic Proteins (BMPs): Potent osteoinductive agents (TGF-β superfamily).
- Cytokines (e.g., IL-1, IL-6): ↑ bone resorption (e.g., during inflammation).
High‑Yield Points - ⚡ Biggest Takeaways
- Primary ossification centers appear prenatally; secondary centers (epiphyses) postnatally.
- Long bone growth at epiphyseal plates; fusion signals skeletal maturity.
- Subadult age estimation: dental development & epiphyseal fusion are key.
- Cortical remodeling (Haversian systems) is continuous, distinguishes adult/juvenile bone.
- Cranial suture closure: While providing general adult age indication, high variability makes it unreliable standalone; pubic symphysis & sternal rib ends more reliable.
- Advanced imaging & histological analysis provide accurate adult age estimation.
- Bone density peaks in young adulthood, then ↓ decreases with age.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

