Pregnancy Diagnosis & Duration - Proof & Puzzles
- Diagnosis Stages:
- Presumptive: Amenorrhea, N/V, quickening (16-22 wks - later in primigravida).
- Probable: Hegar's sign (6-8 wks), Goodell's sign (6 wks), Chadwick's sign (6-8 wks), positive hCG (now preferred over physical signs).
- Positive: FHS (Doppler 8-10 wks; Fetoscope 18-20 wks), fetal movements (examiner >20 wks), USG (cardiac activity 6-7 wks).
- Duration Estimation:
- USG CRL (1st trimester - gold standard); BPD, HC, AC, FL later.
- Naegele's Rule: LMP + 9 months + 7 days (less accurate than USG).
- Forensic Aspects:
- Puzzles: Superfecundation (multiple ova, same cycle, different acts); Superfetation (new conception in existing pregnancy - rare).
- Delivery Signs: Recent (lochia, colostrum); Remote (parous os, old striae).
⭐ While Hegar's sign (softening of uterine isthmus at 6-8 weeks) remains a probable sign, ultrasound and hCG provide superior diagnostic accuracy in modern practice.
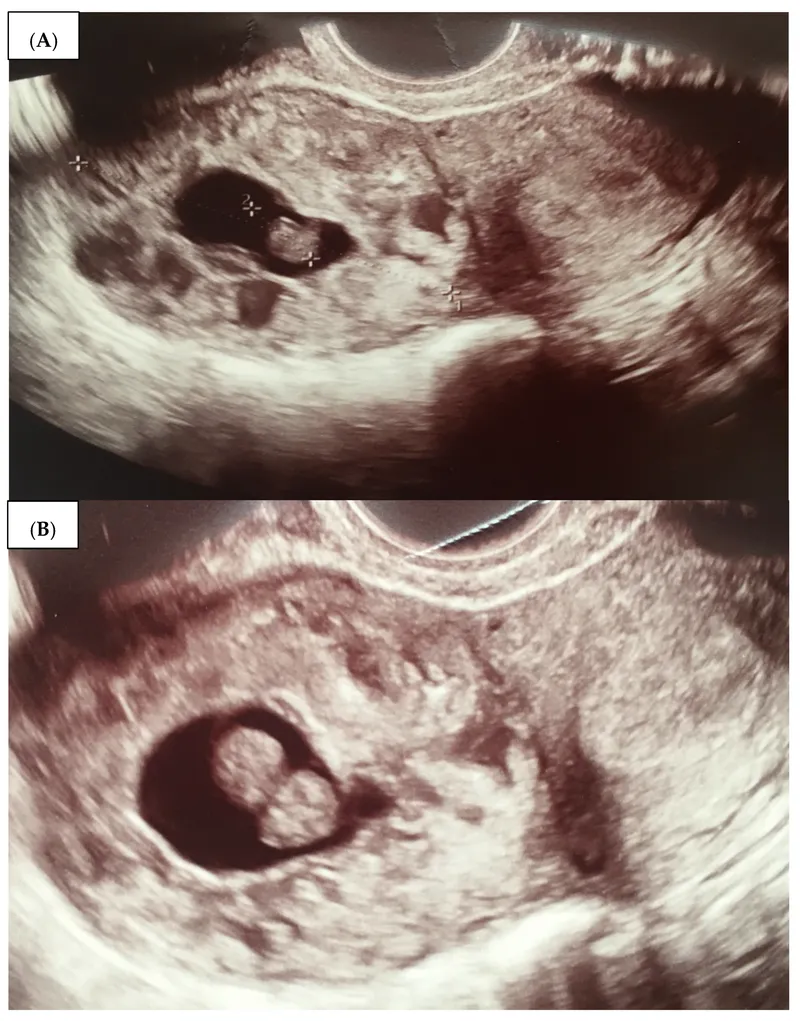
Delivery & Birth Status - Life's Legal Line
- Delivery: Expulsion/extraction of fetus.
- Live Birth: Post-expulsion, breathes or shows any sign of life (heartbeat, cord pulsation, muscle movement), irrespective of gestation/cord.
- Stillbirth: Fetus born dead after 20-28 weeks gestation (varies by guidelines); no signs of life.
- Signs of Live Birth:
- Respiration: Primary. Hydrostatic Test (lungs float). 📌 Float for Life.
- Circulation: Heartbeat, cord pulsation.
- Muscular Movement: Voluntary.
- Signs of Stillbirth:
- Maceration: Aseptic autolysis (skin slippage, soft skull).
- Mummification: Dry, shriveled.
- Viability: Fetus capable of independent existence (modern practice: >24 weeks with advanced care; traditional: >28 weeks or >1000g).
- Legal Implications:
- Infanticide (Sec 80, 81 BNS).
- Concealment of birth (Sec 83 BNS).
⭐ Hydrostatic Test: Key for live birth; lungs float if respired. Beware false +ves (putrefaction) & false -ves (brief gasps).
Abortion & MTP Act - Lawful Limits
MTP Act, 1971 (Amended 2021) regulates termination. Key lawful limits:
- Up to 20 weeks: Opinion of 1 Registered Medical Practitioner (RMP).
- Grounds: Risk to woman's life/health (physical/mental), rape, contraceptive failure (married woman/partner).
- 20-24 weeks: Opinion of 2 RMPs.
- For special categories: Rape survivors, minors, women with disabilities (physical/mental), substantial fetal malformation, change in marital status (widowhood/divorce), humanitarian settings/disaster.
- Beyond 24 weeks: Medical Board approval for fetal abnormalities incompatible with life or significant maternal health risk ONLY. Strict criteria - not for manageable conditions with limited life expectancy.
*Special categories detailed in the point above.
⭐ MTP Amendment Act, 2021: Increased gestation limit to 24 weeks for defined special categories of women; Medical Board approval beyond 24 weeks limited to abnormalities incompatible with life or severe maternal health risk.
- Consent:
- Woman's consent is paramount.
- If <18 years or mentally ill: Guardian's consent required.
- 📌 "20-24-Board": Key limits for 1 RMP, 2 RMPs, & Medical Board approval respectively based on gestational age.
Infanticide & Neonatal Deaths - Tiny Tragedies
- Infanticide: The term "infant" clinically refers to a child up to 1 year. BNS sections 90, 91, 93 address specific acts related to causing death of children before/after birth and concealment of birth, rather than defining "infanticide" as a distinct crime.
- Neonatal Death: Death within first 28 days of life. Early (<7 days), Late (7-28 days).
- Common Causes: Prematurity, Birth Asphyxia (most common in India), Infections (Sepsis, Pneumonia), Congenital Malformations, Trauma (accidental/non-accidental).
- Signs of Live Birth:
- Evidence of breathing (e.g., air in lungs/stomach).
- 📌 Hydrostatic Test (Docimasia Pulmonum): Historical test with limited reliability; comprehensive examination required.
- Battered Baby Syndrome (Caffey's Syndrome):
- Multiple injuries, various healing stages.
- Key indicators: Subdural hematoma, retinal hemorrhages, metaphyseal fractures.
- Sudden Infant Death Syndrome (SIDS):
- Sudden, unexplained death in an infant <1 year (peak incidence 2-4 months).
- Risk factors include prone sleeping position.
⭐ The Hydrostatic test (Galen's test) is a historical test for live birth; modern forensic practice emphasizes comprehensive examination as this test has limitations and potential for false results.
High‑Yield Points - ⚡ Biggest Takeaways
- Superfecundation: two ova, same cycle, different acts. Superfetation: fertilization in a subsequent cycle.
- Recent delivery signs: lax perineum, lochia, subinvoluted uterus.
- Criminal abortion (BNS 88-89) vs. legal termination under MTP Act (Amendment) 2021.
- Fetal viability: key for infanticide; modern assessment considers case-by-case basis with neonatal care advances, not strictly 28 weeks / 1000g.
- Live birth: determined by comprehensive evaluation including histological lung examination, alveolar expansion, food in stomach; hydrostatic test unreliable.
- Paternity disputes: resolved by DNA fingerprinting.
- Maternal deaths: common causes include hemorrhage, sepsis, illegal abortions.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

