MVD: Intro & Anatomy - Gut Feeling Gone Wrong
- Mesenteric Vascular Disease (MVD): Insufficient blood supply to intestines.
- Key Types:
- Acute Mesenteric Ischemia (AMI): Sudden arterial blockage.
- Chronic Mesenteric Ischemia (CMI): Gradual narrowing; "intestinal angina".
- Mesenteric Venous Thrombosis (MVT): Venous outflow obstruction.
- Primary Arteries:
- Celiac Trunk: Supplies foregut (e.g., stomach, duodenum).
- Superior Mesenteric Artery (SMA): Supplies midgut (e.g., jejunum, ileum, right colon).
- Inferior Mesenteric Artery (IMA): Supplies hindgut (e.g., left colon, rectum).
- Critical Collaterals:
- Marginal Artery of Drummond: Connects SMA & IMA branches.
- Arc of Riolan (Meandering Mesenteric Artery): Direct SMA-IMA link.
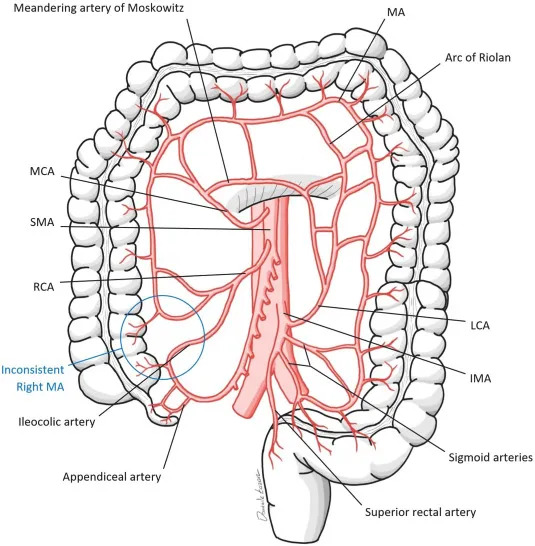
⭐ Superior Mesenteric Artery (SMA) is the most commonly affected vessel in acute mesenteric ischemia.
Acute Mesenteric Ischemia - Time Is Bowel
Life-threatening emergency; rapid diagnosis & intervention crucial. "Time is bowel." High mortality (~70-90% if delayed).
- Types & Causes:
- Arterial Embolic (~50%): Cardiac source (AF, MI).
- Arterial Thrombotic (~25%): Atherosclerosis (often prior CMI).
- Non-Occlusive (NOMI, ~20%): Low flow states (shock, vasopressors).
- Mesenteric Venous Thrombosis (MVT, ~5%): Hypercoagulability, malignancy. 📌 Hypercoagulable, Inflammation, Malignancy, Portal HTN (HIMP).
- Clinical:
⭐ Classic: Severe abdominal pain 'out of proportion' to physical findings.
- N/V/D, bloody stools (late). Peritoneal signs = infarction.
- Diagnosis:
- Labs: ↑ Lactate (> 2 mmol/L), acidosis (pH < 7.35), ↑ D-dimer.
- Imaging: CTA (gold standard).
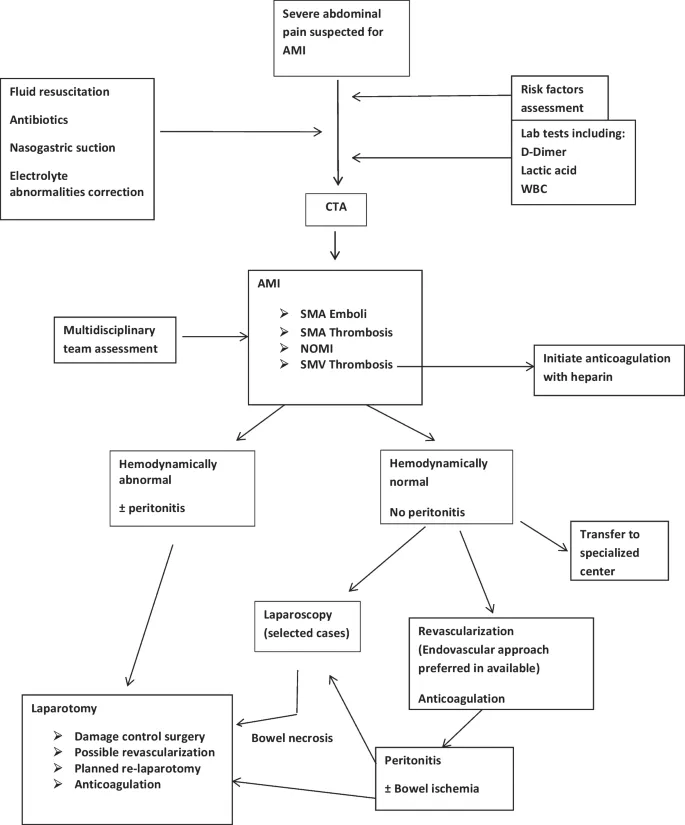
- Management Algorithm:
Chronic Mesenteric Ischemia - Slow Gut Starvation
- Pathophysiology: Atherosclerosis (most common, >90%) leading to ↓ blood flow, typically requiring >70% stenosis in ≥2 major mesenteric arteries (celiac, SMA, IMA).
- Clinical Presentation:
- Often insidious onset.
- ⭐ > Triad: Postprandial abdominal pain ("intestinal angina", ~30 min after meals, dull/crampy), significant weight loss (due to malabsorption & food fear), and food fear (sitophobia).
- Abdominal bruit may be present (~50%).
- Diagnosis:
- Duplex ultrasound (screening).
- CTA or MRA (confirmatory, preferred).
- Conventional angiography (gold standard, allows intervention).
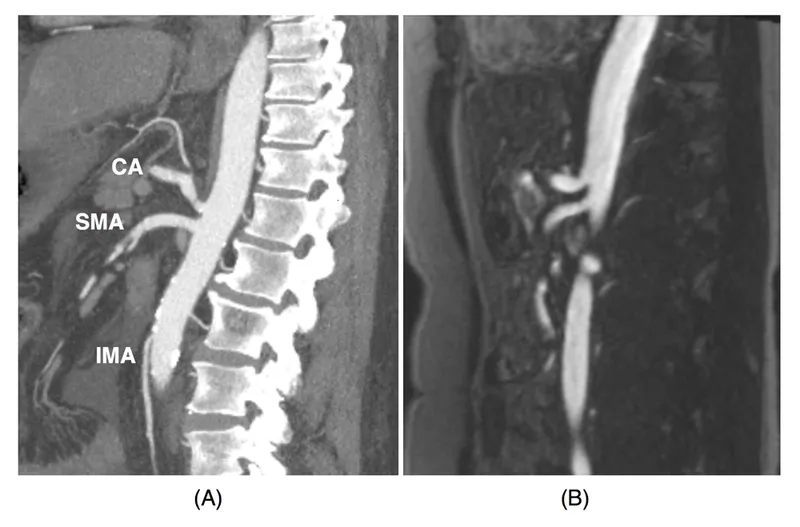
- Management: Revascularization (angioplasty/stenting or surgical bypass) is key. Nutritional support vital. 📌 Mnemonic: "Angina (intestinal), Weight loss, Food fear" (AWFul gut pain).
Related MVD Conditions - Vascular Villains
- Ischemic Colitis (IC)
- Most common mesenteric ischemia; typically non-occlusive (low flow).
- Key sites: Watershed areas (splenic flexure, rectosigmoid junction).
- Clinical: Sudden cramping LLQ pain, hematochezia, tenesmus.
- Imaging: "Thumbprinting" (submucosal edema/hemorrhage) on CT/barium.
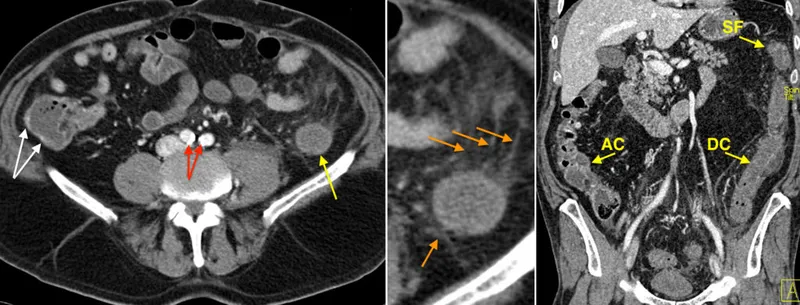
⭐ Ischemic colitis most commonly affects watershed areas like the splenic flexure and rectosigmoid junction.
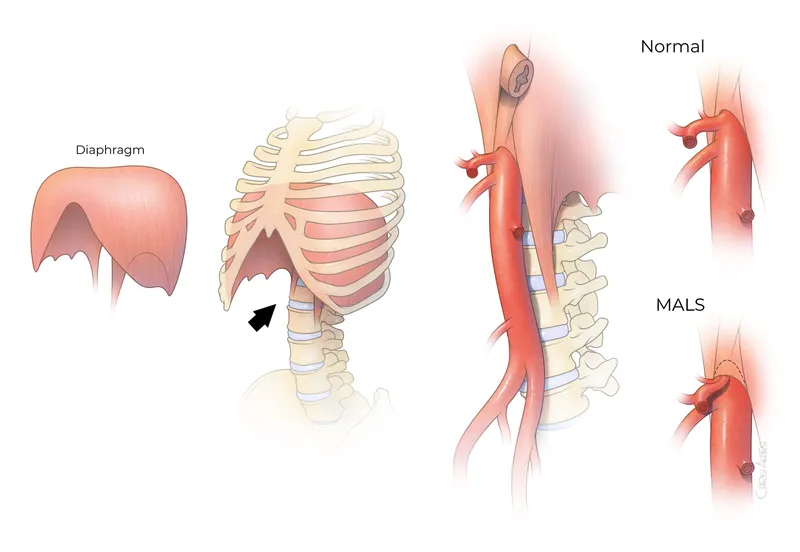
- Median Arcuate Ligament Syndrome (MALS)
- Celiac artery compression by the median arcuate ligament of diaphragm.
- Classic: Postprandial epigastric pain, weight loss, epigastric bruit (louder on expiration).
- Diagnosis: Duplex US (↑ celiac velocity with expiration), CT/MR angiography (focal stenosis, hooked appearance).
- Segmental Arterial Mediolysis (SAM)
- Rare non-atherosclerotic, non-inflammatory vasculopathy; causes dissection/aneurysm.
- Primarily affects splanchnic arteries (splenic, hepatic, SMA).
- Pathology: Lysis of outer arterial media → weakness.
- Presentation: Acute severe abdominal pain, intra-abdominal hemorrhage, shock; often younger patients.
High‑Yield Points - ⚡ Biggest Takeaways
- Acute Mesenteric Ischemia (AMI): Severe pain "out of proportion" to findings; SMA embolism (AFib) is most common.
- Chronic Mesenteric Ischemia (CMI): "Intestinal angina" (postprandial pain, weight loss, food fear) from atherosclerosis.
- Diagnosis: CT Angiography (CTA) is gold standard. ↑ lactate is a late, poor prognostic sign in AMI.
- AMI Treatment: Urgent revascularization (surgical/endovascular) ± bowel resection.
- Mesenteric Venous Thrombosis (MVT): Linked to hypercoagulable states; primary treatment is anticoagulation.
- Non-Occlusive Mesenteric Ischemia (NOMI): Due to low flow/vasoconstriction; treat cause, consider vasodilators.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

