CAD Basics & Anatomy - Neck's Vital Pipes
Carotid Artery Disease (CAD): Atherosclerotic plaque buildup causing stenosis (narrowing) of carotid arteries, mainly extracranial. Reduces cerebral blood flow, increasing TIA/stroke risk.
- Common Carotid Artery (CCA): Bifurcates at C3-C4 level into ICA & ECA.
- Internal Carotid Artery (ICA): Supplies brain (Circle of Willis). No neck branches.
- Carotid Bulb/Sinus: Dilation at ICA origin; baroreceptors (CN IX), chemoreceptors (CN IX, X).
- External Carotid Artery (ECA): Supplies face, neck, scalp. Has neck branches.

⭐ The carotid bifurcation is the most common site for atherosclerotic plaque development.
Pathophysiology & Risks - Plaque Attack Central
- Atherosclerosis: Chronic inflammation from endothelial injury (e.g., at carotid bifurcation) → LDL influx, macrophage foam cells → fatty streak → fibrous plaque.
- Plaque Types:
- Stable: Thick fibrous cap, small lipid core, less inflammation.
- Vulnerable: Thin cap, large necrotic lipid core, ↑inflammation. Prone to rupture/ulceration → thromboembolism.
- Risk Factors:
- Non-Modifiable: Age (>60), Male sex, Family history (genetics).
- Modifiable: Hypertension (HTN), Diabetes Mellitus (DM), Hyperlipidemia (HLD), Smoking.
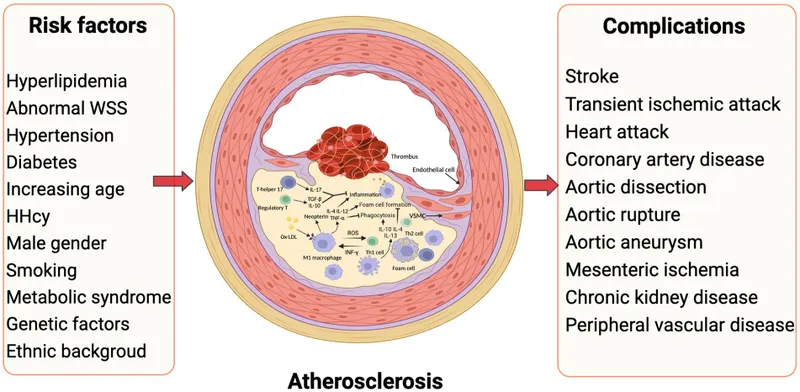
⭐ Hemorrhage into a plaque is a key event leading to acute symptoms.
Symptoms & Diagnosis - Stroke Alarms
-
Presentation: Often asymptomatic. Symptomatic disease includes:
- Transient Ischemic Attack (TIA): Focal deficit <24 hrs.
- Amaurosis Fugax: Transient monocular blindness (ipsilateral ICA).
- Reversible Ischemic Neurologic Deficit (RIND): Deficit >24 hrs, <3 weeks.
- Stroke (CVA): Permanent deficit.
- Clinical features depend on territory: e.g., contralateral weakness/sensory loss, aphasia.
- 📌 FAST (Face, Arms, Speech, Time) for stroke recognition.
-
Diagnostic Modalities:
- Duplex Ultrasound (DUS): First-line, non-invasive. Grades stenosis (NASCET criteria). Intervention often considered for symptomatic >50% stenosis, or asymptomatic >70% stenosis.
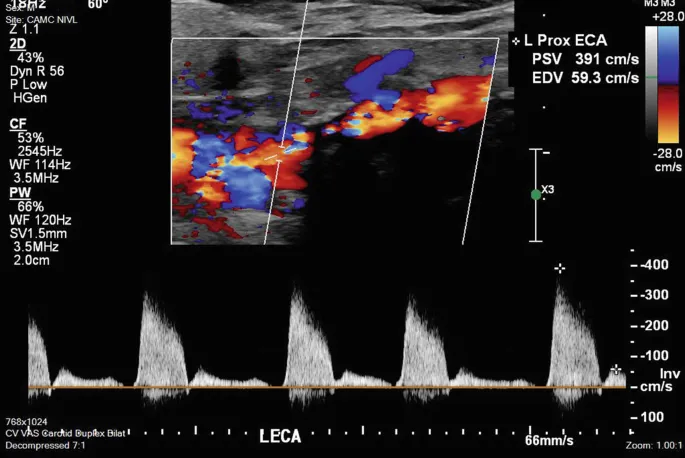
- CTA/MRA: Provide detailed anatomy, useful for surgical planning if DUS unclear or intervention planned.
- DSA (Digital Subtraction Angiography): Gold standard, invasive. Reserved for equivocal cases or pre-intervention.
- Duplex Ultrasound (DUS): First-line, non-invasive. Grades stenosis (NASCET criteria). Intervention often considered for symptomatic >50% stenosis, or asymptomatic >70% stenosis.
⭐ Amaurosis fugax (transient monocular blindness, often described as a "curtain falling") is a classic symptom of ipsilateral Internal Carotid Artery (ICA) disease.
Diagnostic Algorithm:
Comparison of Diagnostic Modalities:
| Modality | Sensitivity | Specificity | Invasiveness | Cost | Key Notes |
|---|---|---|---|---|---|
| Duplex US | High | High | Non-invasive | Low | Screening, stenosis grading (NASCET velocity criteria) |
| CTA | Very High | Very High | Minimally | Medium | Radiation, contrast, good for calcification |
| MRA | Very High | Very High | Non-invasive | High | No radiation, contrast (gadolinium), artifacts |
| DSA | Highest | Highest | Invasive | High | Gold standard, risk of stroke, pre-intervention |
Management Decisions - Scalpels or Stents
- Optimal Medical Therapy (OMT): Antiplatelets (Aspirin, Clopidogrel), Statins, BP control, Lifestyle modification.
- Intervention Thresholds (NASCET/ACAS/ACST criteria):
- Symptomatic (TIA/Stroke): ≥70% stenosis; 50-69% (select: male, recent stroke).
- Asymptomatic: ≥60% stenosis (select: low surgical risk, >5yr life expectancy).
- CEA steps: Open plaque removal, often patch angioplasty.
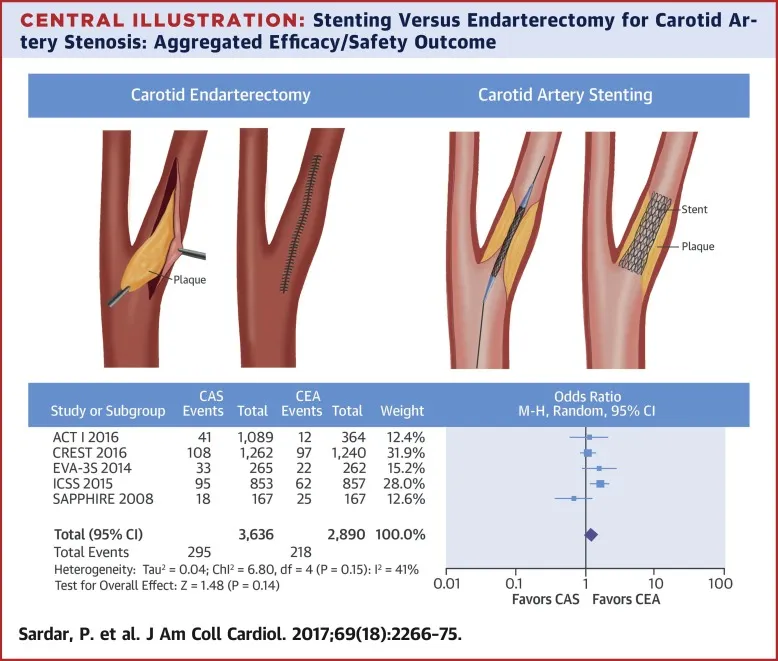
| Feature | CEA (Scalpel) | CAS (Stent) |
|---|---|---|
| Suited For | Standard risk; Complex plaque | High surgical risk; Hostile neck; Post-CEA restenosis |
| Pros | Durable; ↓Long-term stroke | Less invasive; Quicker recovery |
| Cons | Incision; Nerve injury (CN VII,X,XII) | ↑Peri-op stroke/MI (some trials); Restenosis |
| Complications | Stroke/MI, Nerve injury, Hyperperfusion | Stroke/MI, Groin issues, Restenosis |
Prevention & Follow-Up - Keeping Pipes Clear
- Primary Prevention:
- Aggressive risk factor modification: Control HTN, DM, dyslipidemia; smoking cessation.
- Secondary Prevention (Post-TIA/Stroke/Intervention):
- Antiplatelet therapy (e.g., Aspirin, Clopidogrel).
- High-intensity statin therapy.
- Post-Operative Care (CEA/CAS):
- BP control (avoid hypo/hypertension).
- Neuro checks (for stroke, nerve injury).
- Wound care (hematoma, infection).
- Long-Term Surveillance:
- Duplex Ultrasound: 1, 6, 12 months post-op, then annually to detect restenosis.
⭐ Dual antiplatelet therapy (DAPT) is often recommended for at least 30 days after Carotid Artery Stenting (CAS).
High‑Yield Points - ⚡ Biggest Takeaways
- Carotid bifurcation/proximal ICA: most common atherosclerotic site.
- Symptomatic patients (TIA, stroke) with >50% stenosis (NASCET) strongly benefit from revascularization.
- Asymptomatic patients: consider intervention for >60-70% stenosis, based on risk factors.
- Duplex ultrasound: initial diagnostic tool; DSA remains gold standard if needed.
- Carotid Endarterectomy (CEA): gold standard surgical treatment for suitable patients.
- Carotid Artery Stenting (CAS): alternative for high surgical risk or specific anatomies.
- Amaurosis fugax (transient monocular blindness): a critical warning sign.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

