Testicular Tumors - Nuts & Bolts
- Most common solid malignancy in men: 15-35 yrs.
- Incidence: 1-2% of male cancers.
- Risk Factors:
- Cryptorchidism (most significant, ↑4-10x risk)
- Family history
- Previous testicular Ca
- Klinefelter syndrome
- DES exposure
- Types:
- Germ Cell Tumors (GCTs): >95% (seminoma & non-seminoma)
- Non-Germ Cell Tumors (NGCTs): <5% (e.g., Leydig, Sertoli, Lymphoma)
- Presentation: Painless testicular mass.
⭐ Cryptorchidism is the single most important risk factor, increasing the likelihood of developing testicular cancer by 4 to 10 times.
Tumor Types - The Rogue's Gallery
- Germ Cell Tumors (GCTs): ~95% of testicular tumors.
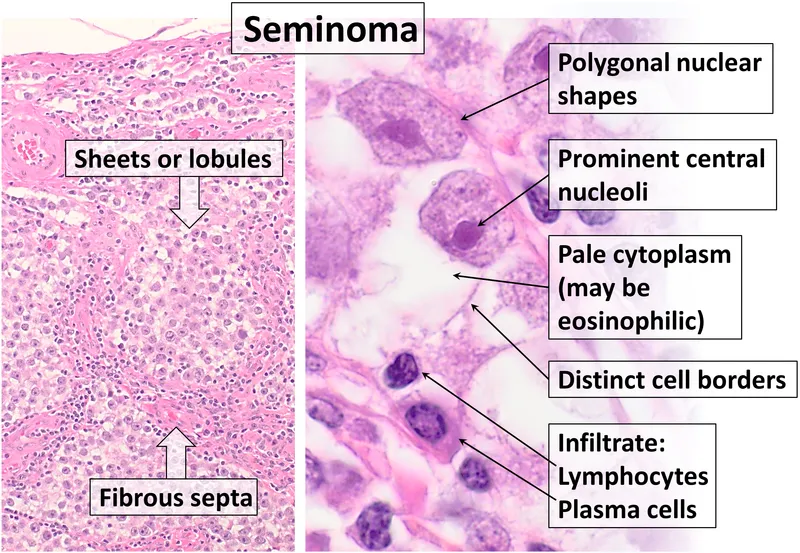
- Seminoma (50% of GCTs):
- Most common type. Peak: 30-40 yrs.
- Markers: PLAP (+), hCG (±, if syncytiotrophoblasts), LDH (±). AFP always negative.
- Classic, Anaplastic, Spermatocytic variants.
- Non-Seminomatous GCTs (NSGCTs):
- Embryonal Carcinoma (20%):
- Aggressive. Peak: 20-30 yrs.
- Markers: AFP (±), hCG (±), CD30 (+).
- Yolk Sac Tumor (Endodermal Sinus Tumor):
- Most common in infants/children (<3 yrs).
- Markers: AFP (+++). Schiller-Duval bodies (pathognomonic).
- Choriocarcinoma (<1%):
- Highly malignant, early hematogenous spread.
- Markers: hCG (+++).
- Teratoma (5%):
- Mature, Immature, with somatic-type malignancy.
- Markers: AFP (±), hCG (±). Often chemoresistant.
- Embryonal Carcinoma (20%):
- Seminoma (50% of GCTs):
- Non-Germ Cell Tumors (Sex Cord-Stromal Tumors): ~5%
- Leydig Cell Tumors: Androgen/estrogen secretion. Reinke crystals.
- Sertoli Cell Tumors: Usually benign.
- Gonadoblastoma: Associated with dysgenetic gonads.
⭐ > Yolk Sac Tumor is the most common testicular tumor in pre-pubertal children, typically presenting before 3 years of age and strongly associated with ↑AFP.
Signs & Sleuthing - The Detective Work
- Presentation:
- Painless testicular mass (commonest).
- Dull ache, scrotal heaviness.
- Acute pain (~10%; hemorrhage/infarction).
- Metastatic: cough, back pain, neck mass.
- Gynecomastia (hCG-producing tumors).
- Examination:
- Firm, non-tender mass in testis.
- Check contralateral testis, abdomen, supraclavicular nodes.
- Investigations:
- Scrotal USG: Initial imaging.
- Seminoma: hypoechoic, homogeneous.
- NSGCT: heterogeneous, cystic, calcified.
- Tumor Markers: AFP, β-hCG, LDH.
⭐ AFP is NEVER elevated in pure Seminoma. (Key for Yolk Sac, Embryonal Ca).
- β-hCG: ↑ Choriocarcinoma, Embryonal Ca, ~15-20% Seminomas.
- LDH: Indicates tumor burden.
- Staging: CT (Chest, Abdomen, Pelvis).
- Diagnosis/Treatment: Radical inguinal orchiectomy.
- ⚠️ Avoid trans-scrotal biopsy (risk of tumor spillage).
- Scrotal USG: Initial imaging.
Staging & Strategy - The Game Plan
Staging uses AJCC TNM system & serum markers (S) post-orchiectomy.
- T (Tumor): pTis, pT1 (testis), pT2 (tunica vaginalis/LVI), pT3 (spermatic cord), pT4 (scrotum).
- N (Nodes): N0 (none), N1 (≤2cm), N2 (>2-5cm), N3 (>5cm).
- M (Metastasis): M0 (none), M1a (non-regional nodes/lung), M1b (other visceral).
- S (Markers): Post-orchiectomy. S0 (normal). S1, S2, S3 by highest marker value:
- LDH (xULN): S1 (>1.5-10), S2 (>10)
- hCG (mIU/mL): S1 (5-<5k), S2 (5k-50k), S3 (>50k)
- AFP (ng/mL): S1 (1k-<10k), S2 (≥10k)
IGCCCG classifies metastatic GCTs: Good, Intermediate, Poor prognosis.
⭐ For clinical Stage I Seminoma, adjuvant single-dose Carboplatin (Area Under Curve 7) is a key option reducing relapse vs surveillance, an alternative to radiotherapy.
High‑Yield Points - ⚡ Biggest Takeaways
- Testicular tumors: Peak incidence 15-35 years; often painless scrotal mass.
- Seminoma: Most common GCT, radiosensitive, can have ↑ β-hCG.
- Non-seminomas (NSGCTs): Include yolk sac (↑ AFP), choriocarcinoma (↑ β-hCG), teratoma.
- Tumor Markers: AFP (never in pure seminoma), β-hCG, LDH (tumor burden).
- Management: Radical inguinal orchiectomy is initial step for diagnosis & treatment.
- Risk Factor: Cryptorchidism is the most significant predisposing factor.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

