Indications & Contraindications - Who Gets New Lungs?
Indications:
- End-stage lung diseases (COPD, IPF, CF, PAH)
⭐ COPD: most common indication.
- Life expectancy < 18-24 months
- Severe functional impairment (NYHA III-IV)
- PFTs: FEV1 < 30% (COPD/CF); FVC < 60% or DLCO < 50% (IPF)
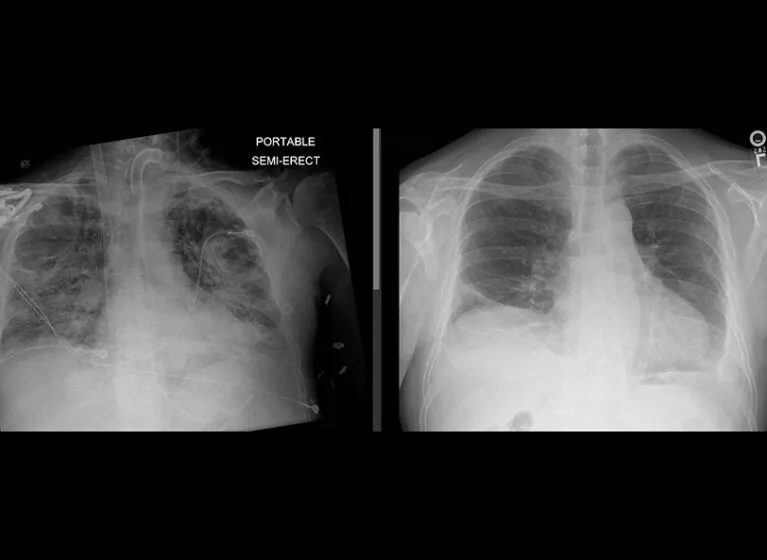
Contraindications:
| Absolute | Relative |
|---|---|
| Malignancy (active/recent <2-5y) | Age > 65 (SLT), > 60 (BLT) |
| Irreversible other major organ failure | BMI < 16 or > 35 |
| Active infection (HIV, uncontrolled Hep B/C) | Mech. ventilation/ECMO (bridge) |
| Current smoking/substance abuse (6m) | Prior extensive thoracic surgery/radiation |
| Severe psych illness/non-adherence | Colonization with resistant organisms |
Donor Selection & Allocation - Gifting Breath Anew
- Ideal Donor Criteria:
- Age < 55-65 yrs
- ABO compatible
- PaO2/FiO2 > 300 mmHg (on PEEP 5 cm H2O, FiO2 1.0)
- Clear CXR; no aspiration/trauma
- No active malignancy/systemic infection
- Smoking < 20 pack-years
- Extended Criteria Donors (ECD): Increasingly used to expand donor pool; criteria less stringent.
- Lung Allocation Score (LAS):
- Prioritizes candidates (≥ 12 yrs). Score 0-100 (↑score = ↑priority).
- Balances waitlist urgency & post-transplant survival benefit.
⭐ Key LAS components: Forced Vital Capacity (FVC), PaO2, 6-minute walk distance (6MWD), pulmonary artery pressure, O2 requirement, age, BMI, creatinine, diagnosis.

Surgical Aspects & Techniques - The Big Swap
- Incisions:
- Clamshell (bilateral anterolateral): DLT standard.
- Posterolateral thoracotomy: For SLT.
- Median sternotomy: Rare, specific cases.
- Procedure Types:
- SLT: IPF, emphysema (non-suppurative).
- DLT: CF, bronchiectasis (suppurative), PAH.
- Cardiopulmonary Bypass (CPB):
- Often for DLT / unstable patients.
- SLT: Off-pump preferred if stable.
- ECMO: Bridge to transplant / intraop support.
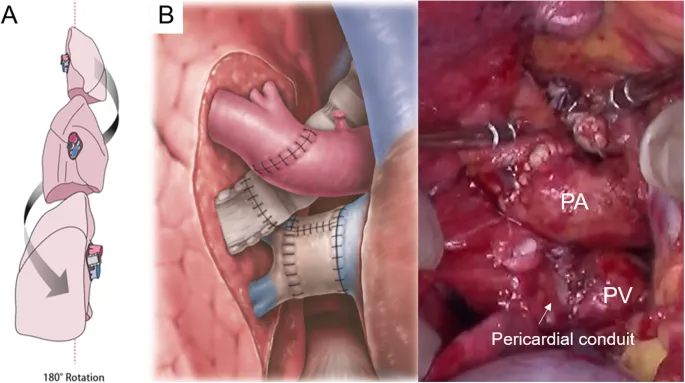
- Anastomotic Technique:
- Bronchial: Telescoping or end-to-end; membranous portion first, then cartilaginous.
- Vascular: Pulmonary Artery (PA) typically end-to-end; Left Atrial (LA) cuff for pulmonary veins.
⭐ Sequence: Bronchus → Pulm. Artery → Pulm. Veins (LA Cuff). 📌 Breathe Air Via Lungs (Bronchus, Artery, Veins).
- Size Matching: Vital; donor lung often reduced if oversized.
Post-Transplant Care & Hurdles - Navigating New Normals
-
Immunosuppression (Lifelong):
- Standard: Triple therapy - Calcineurin Inhibitor (CNI), Antimetabolite, Corticosteroids.
- CNIs (Tacrolimus, Cyclosporine): Nephrotoxicity, neurotoxicity. Tacrolimus target levels: 3-12 ng/mL (varies).
- Antimetabolites (Mycophenolate Mofetil, Azathioprine): GI upset, myelosuppression.
- Corticosteroids (Prednisone): Hyperglycemia, osteoporosis, infections.
- Induction therapy (e.g., Basiliximab, ATG) may be used peri-operatively.
- Standard: Triple therapy - Calcineurin Inhibitor (CNI), Antimetabolite, Corticosteroids.
-
Monitoring:
- Pulmonary Function Tests (PFTs): Spirometry (FEV1, FVC) regularly.
- Bronchoscopy with Transbronchial Biopsy (TBBx) & Bronchoalveolar Lavage (BAL): Surveillance for rejection/infection.
- Imaging: Chest X-ray, CT scans as indicated.
- Therapeutic drug monitoring for CNIs.
-
Key Hurdles & Complications:
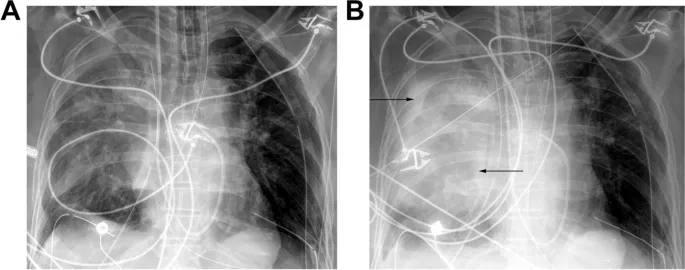
- Primary Graft Dysfunction (PGD): Acute lung injury within 72 hours post-transplant; graded 0-3.
- Rejection:
- Acute Cellular Rejection (ACR): T-cell mediated. Dx: Biopsy. Rx: Pulse steroids, optimize immunosuppression.
- Antibody-Mediated Rejection (AMR): Donor-Specific Antibodies (DSA). Dx: Biopsy (C4d), DSA. Rx: IVIG, plasmapheresis, rituximab.
- Chronic Lung Allograft Dysfunction (CLAD): Leading cause of late mortality.
- Bronchiolitis Obliterans Syndrome (BOS): Airflow obstruction (↓FEV1). Most common form.
- Restrictive Allograft Syndrome (RAS): Restrictive defects, fibrosis.
⭐ BOS, the most common phenotype of CLAD, is defined by a persistent decline in FEV1 to <80% of the post-transplant baseline. - Infections: High risk due to immunosuppression. + Bacterial: Pneumonia common early. + Viral: Cytomegalovirus (CMV) - prophylaxis/pre-emptive therapy (Valganciclovir). + Fungal: Aspergillus - prophylaxis (e.g., Voriconazole). - Other: Drug toxicities (renal, metabolic), malignancy (PTLD, skin cancer), cardiovascular disease.
High‑Yield Points - ⚡ Biggest Takeaways
- COPD, IPF, Cystic Fibrosis are key indications; DLT for suppurative diseases.
- Active malignancy & untreatable infections (e.g., B. cenocepacia) are absolute contraindications.
- Primary Graft Dysfunction (PGD) is a critical early complication from reperfusion injury.
- CLAD, notably Bronchiolitis Obliterans Syndrome (BOS), is the main cause of late graft failure.
- Standard immunosuppression is a triple-drug regimen (CNI, antimetabolite, steroids).
- CMV and Aspergillus are significant opportunistic infections post-transplant_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

