Basic Transplant Immunology - Code Crackers
- Key Antigens:
- Major Histocompatibility Complex (MHC) / Human Leukocyte Antigen (HLA): Primary targets.
- Class I (HLA-A, B, C): On all nucleated cells. Present antigens to CD8+ T-cells.
- Class II (HLA-DR, DQ, DP): On Antigen-Presenting Cells (APCs). Present antigens to CD4+ T-cells.
- Minor Histocompatibility Antigens (mHA): Peptides from polymorphic proteins; contribute to rejection.
- Major Histocompatibility Complex (MHC) / Human Leukocyte Antigen (HLA): Primary targets.
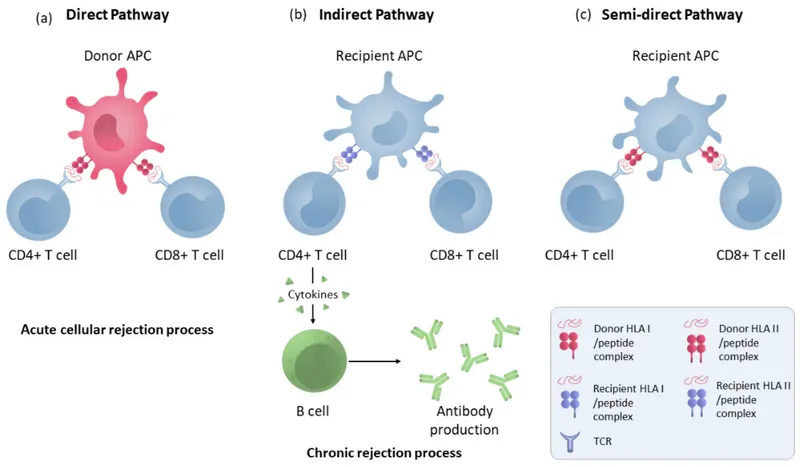
- Allorecognition Pathways: Recipient T-cell recognition of alloantigens.

* Direct: Donor APCs activate recipient T-cells. Key in acute rejection.
* Indirect: Recipient APCs present processed donor antigens. Key in chronic rejection.
⭐ HLA genes are the most polymorphic in the human genome, critical for immune specificity and transplant matching.
Graft Rejection Mechanisms - Unwanted Guests
📌 Rejection types: HAC (Hyperacute, Acute, Chronic)
- Hyperacute Rejection (Minutes-Hours)
- Pre-formed recipient anti-donor Abs (ABO, HLA).
- Type II hypersensitivity.
- Causes: Thrombosis, ischemic necrosis.
- Prevention: ABO crossmatching, lymphocytotoxic crossmatch.
⭐ Hyperacute rejection is mediated by pre-existing ABO or HLA antibodies.
- Acute Rejection (Days-Weeks, <6 months)
- Cellular (ACR): T-cell (CD8+, CD4+) mediated; Type IV hypersensitivity.
- Direct & indirect allorecognition.
- Path: Lymphocytic infiltrate, tubulitis, endotheliitis.
- Humoral (AMR): Antibody-mediated (de novo DSA); Type II hypersensitivity.
- Path: C4d deposition, vasculitis.
- Treatment: ↑ Immunosuppression (steroids, anti-lymphocyte Abs).
- Cellular (ACR): T-cell (CD8+, CD4+) mediated; Type IV hypersensitivity.
- Chronic Rejection (Months-Years)
- Alloimmune (T/B cells) & non-alloimmune factors.
- Path: Chronic inflammation, fibrosis, graft arteriosclerosis, organ-specific (e.g., bronchiolitis obliterans - lung).
- Often irreversible.
 oka
oka
Immunosuppressive Drugs - Peace Keepers

- Goal: Prevent & treat rejection, minimize toxicity.
- Phases: Induction (peri-op), Maintenance (lifelong), Rejection treatment (pulse).
- Key Classes:
- Calcineurin Inhibitors (CNIs): Cyclosporine, Tacrolimus.
- MOA: ↓ IL-2 production → ↓ T-cell activation.
- SE: Nephrotoxicity (⚠️), neurotoxicity, HTN, hyperglycemia. Cyclosporine: gingival hyperplasia. Tacrolimus: ↑ diabetes risk.
⭐ Cyclosporine and Tacrolimus are calcineurin inhibitors, vital for preventing T-cell mediated rejection.
- Antiproliferatives: Azathioprine (AZA), Mycophenolate (MMF).
- AZA MOA: Inhibits purine synthesis. SE: Bone marrow suppression (BMS).
- MMF MOA: Inhibits IMPDH → ↓ B & T cell proliferation. SE: GI upset, BMS.
- mTOR Inhibitors: Sirolimus, Everolimus.
- MOA: Inhibit mTOR → ↓ T-cell proliferation.
- SE: Hyperlipidemia, poor wound healing, mouth ulcers.
- Corticosteroids: Prednisolone.
- MOA: Broad anti-inflammatory.
- SE (long-term): Cushingoid, osteoporosis, ↑ infection risk.
- Biologics: Anti-thymocyte globulin (ATG) (T-cell depletion), Basiliximab (IL-2R antagonist).
- Calcineurin Inhibitors (CNIs): Cyclosporine, Tacrolimus.
GVHD & Tolerance - Special Ops
- Graft-versus-Host Disease (GVHD): Donor T-cells attack recipient tissues.
- Acute GVHD: <100 days. Targets: Skin (rash), Liver (jaundice, ↑LFTs), GIT (diarrhea).
- Chronic GVHD: >100 days. Multi-organ, autoimmune-like features.
- Pathophysiology (Acute GVHD):
- Phase 1: Host tissue damage (conditioning regimen).
- Phase 2: Donor T-cell activation, proliferation.
- Phase 3: Cellular & inflammatory effector damage.
- Prevention: Immunosuppression (e.g., Cyclosporine, Methotrexate), T-cell depletion.
- Tolerance: Graft acceptance without ongoing immunosuppression.
- Mechanisms: Clonal anergy/deletion, regulatory T-cells (Tregs).
- Chimerism (donor/recipient cell coexistence) promotes tolerance.

⭐ GVHD is a major complication of allogeneic hematopoietic stem cell transplantation (HSCT), primarily mediated by donor T-cells attacking recipient tissues like skin, liver, and the GI tract.
High‑Yield Points - ⚡ Biggest Takeaways
- Major Histocompatibility Complex (MHC/HLA) matching is paramount to prevent graft rejection.
- T-cells (CD4+ helpers, CD8+ cytotoxics) are central mediators of acute cellular rejection.
- Hyperacute rejection is immediate, caused by pre-formed anti-donor antibodies (ABO, HLA).
- Acute rejection can be cellular (T-cell mediated) or humoral (antibody-mediated, C4d+).
- Chronic rejection features gradual fibrosis and graft vascular disease (arteriosclerosis).
- Key immunosuppressants include calcineurin inhibitors, antimetabolites, and corticosteroids.
- Graft-versus-Host Disease (GVHD): Donor T-cells attack recipient in bone marrow/stem cell transplants.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

