Surgical Sepsis - Code Red Germs
- Key Pathogens & Significance:
- Staphylococcus aureus (esp. MRSA): Leading cause of SSIs; toxin-mediated.
- Streptococcus pyogenes (GAS): Rapidly progressive necrotizing infections.
- Enterococci (esp. VRE): High-level antibiotic resistance.
- Pseudomonas aeruginosa: Opportunistic, biofilm former, common in burns/ICU.
- Escherichia coli & other Enterobacterales (ESBL/CRE): Gut translocation, MDR.
- Bacteroides fragilis: Predominant anaerobe in intra-abdominal sepsis.
- Clostridium spp. (C. perfringens, C. difficile): Gas gangrene, colitis.
- Candida spp.: Fungal sepsis in high-risk patients.
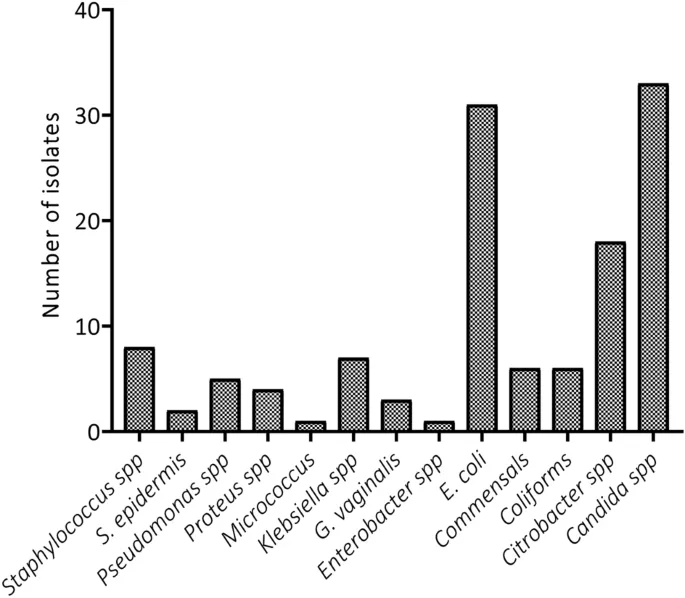
⭐ Carbapenem-Resistant Enterobacterales (CRE) are a critical threat in surgical ICUs, associated with high mortality due to limited treatment options.
Surgical Sepsis - Red Alert Clues
- Clinical Signs (Suspect Sepsis):
- Temperature > 38°C or < 36°C
- Heart Rate > 90 bpm
- Respiratory Rate > 20 breaths/min
- Altered mental status
- Systolic BP < 100 mmHg
- Source of infection (e.g., surgical site, wound, catheter)
- Key Lab Markers:
- WBC > 12,000/µL or < 4,000/µL, or >10% immature bands
- ↑ C-reactive protein (CRP)
- ↑ Procalcitonin (PCT > 0.5 ng/mL is significant)
- ↑ Serum lactate > 2 mmol/L (indicates tissue hypoperfusion)
- Hyperglycemia (Blood glucose > 140 mg/dL in non-diabetic patient)
- Acute oliguria (Urine output < 0.5 mL/kg/hr for ≥ 2 hrs despite fluid resuscitation)
- Scoring (Risk Stratification & Diagnosis):
- qSOFA (quick SOFA): For rapid bedside assessment. Score ≥ 2 suggests high risk of poor outcome.
- Respiratory Rate ≥ 22/min
- Altered mentation (GCS < 15)
- Systolic BP ≤ 100 mmHg
- SOFA (Sequential Organ Failure Assessment): Assesses degree of organ dysfunction. An acute increase of ≥ 2 SOFA points confirms sepsis.
- qSOFA (quick SOFA): For rapid bedside assessment. Score ≥ 2 suggests high risk of poor outcome.
⭐ Procalcitonin (PCT) is a more specific biomarker for bacterial sepsis compared to CRP and its levels correlate with severity of infection, guiding antibiotic stewardship.
Surgical Sepsis - The Rescue Mission
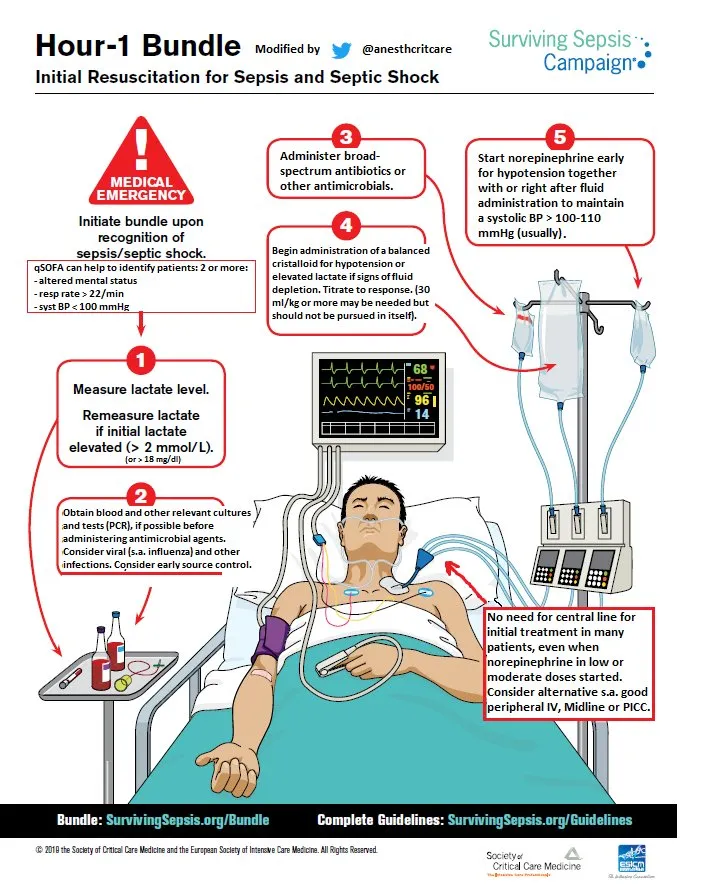
- Core Strategy: Rapidly implement Surviving Sepsis Campaign (SSC) Hour-1 Bundle. Time is tissue!
- Lactate: Measure; remeasure if initial > 2 mmol/L.
- Cultures: Obtain blood cultures before antibiotics.
- Antibiotics: Administer broad-spectrum IV antibiotics (e.g., Piperacillin-Tazobactam + Vancomycin depending on suspected source/local resistance) within 1 hour.
- Fluids: Rapid 30 mL/kg crystalloid for hypotension or lactate ≥ 4 mmol/L.
- Pressors: Vasopressors (Norepinephrine 1st line) if MAP < 65 mmHg post-fluids to ensure organ perfusion.
- Source Control: THE cornerstone in surgical sepsis. 📌 "Drain the Pus, Cut the Dead, Remove the Bad!"
- Urgently identify & control infection: drainage of abscess, debridement of necrotic tissue, removal of infected hardware/catheters.
- Target: definitive control within 6-12 hours of diagnosis.
- Monitoring & Support: Continuous hemodynamic monitoring (e.g., Arterial line), qSOFA/SOFA scores, glucose control, DVT prophylaxis.
⭐ Early and adequate source control is often the most critical intervention in surgical sepsis, significantly impacting outcomes.
Surgical Sepsis - Damage & Defense
- Damage: Systemic Inflammatory Response Syndrome (SIRS) progresses to sepsis, septic shock, & Multiple Organ Dysfunction Syndrome (MODS).
- Key mediators: TNF-α, IL-1, IL-6.
- Endothelial damage, microvascular thrombosis, cellular dysoxia.
- Organ dysfunction: Lungs (ARDS), kidneys (AKI), liver, CNS.
- Defense: Host immune response aims to eradicate infection & restore homeostasis.
- Crucial: Early recognition, source control (drainage, debridement), appropriate antibiotics, hemodynamic support.
- Preventive measures: Asepsis, timely intervention.
⭐ MODS is the most common cause of late death in sepsis patients, often initiated by gut-origin sepsis and translocation of bacteria/endotoxins across a compromised gut barrier (gut-lymph hypothesis).
High‑Yield Points - ⚡ Biggest Takeaways
- Sepsis: Life-threatening organ dysfunction (SOFA score ↑ by ≥2) from dysregulated infection response.
- qSOFA (Altered Mentation, SBP ≤100 mmHg, RR ≥22/min) for rapid sepsis suspicion.
- Septic Shock: Sepsis needing vasopressors for MAP ≥65 mmHg & lactate >2 mmol/L despite fluids.
- Hour-1 Bundle: Lactate, cultures, broad-spectrum antibiotics, rapid fluids, vasopressors. Critical for survival.
- Early source control (drainage, debridement) is paramount in surgical sepsis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

